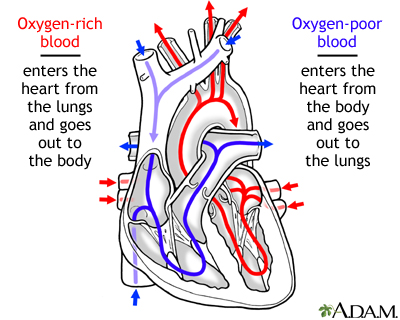
Heart failure is a condition in which the heart is no longer able to pump oxygen-rich blood to the rest of the body efficiently. This causes symptoms to occur throughout the body.
Causes
Heart failure is most often a long-term (chronic) condition, but it may come on suddenly. It can be caused by many different heart problems.
The condition may affect only the right side or only the left side of the heart. Both sides of the heart also can be involved.
Heart failure may be due to two different problems with the heart muscle:
- Your heart muscle cannot contract very well. This is called systolic heart failure, or heart failure with a reduced ejection fraction (HFrEF).
- Your heart muscle is stiff and does not fill up with blood easily even though pumping power is normal. This is called diastolic heart failure, or heart failure with a preserved ejection fraction (HFpEF).
As the heart's pumping becomes less effective, blood may back up in other areas of the body. Fluid may build up in the lungs, liver, gastrointestinal tract, and the arms and legs. This is called congestive heart failure or, more simply, just heart failure.
The most common causes of heart failure are:
- Coronary artery disease (CAD), a narrowing or blockage of the arteries that supply blood and oxygen to the heart. This can weaken the heart muscle over time or suddenly.
- High blood pressure that is not well controlled, leading to problems with stiffness of the heart muscle, or eventually leading to heart muscle weakening.
Other heart problems that may cause heart failure are:
- Congenital heart disease
- Heart attack (when coronary artery disease results in a sudden blockage of a heart artery)
- Heart valves that are leaky or narrowed
- Infection that weakens the heart muscle
- Some types of abnormal heart rhythms (arrhythmias)
Other diseases that can cause or contribute to heart failure:
- Amyloidosis
- Emphysema
- Overactive thyroid
- Sarcoidosis
- Severe anemia
- Too much iron in the body (usually due to hereditary hemochromatosis)
- Underactive thyroid
Symptoms
Symptoms of heart failure often begin slowly. At first, they may only occur when you are very active. Over time, you may notice breathing problems and other symptoms even when you are resting. Symptoms may also appear suddenly after the heart is damaged from a heart attack or other problem.
Common symptoms are:
- Cough
- Fatigue, weakness, faintness
- Loss of appetite
- Need to urinate at night
- Pulse that feels fast or irregular, or a sensation of feeling the heartbeat (palpitations)
- Shortness of breath when you are active or after you lie down
- Swollen (enlarged) liver or abdomen
- Swollen feet and ankles
- Waking up from sleep after a couple of hours due to shortness of breath
- Weight gain
Exams and Tests
Your health care provider will examine you for signs of heart failure:
- Fast or difficult breathing
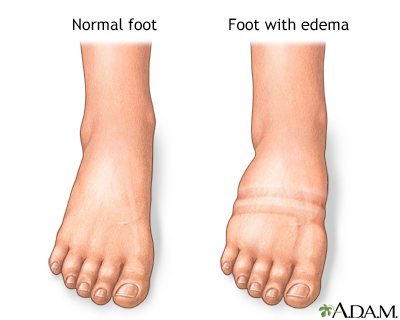
- Leg swelling (edema)
- Neck veins that stick out (are distended)
- Sounds (crackles) from fluid buildup in your lungs, heard through a stethoscope
- Swelling of the liver or abdomen
- Uneven or fast heartbeat and abnormal heart sounds
Many tests are used to diagnose and monitor heart failure.
After an electrocardiogram (ECG), an echocardiogram (echo) is most often the best first test for people when heart failure is being evaluated. Your provider will use it to guide your treatment.
Other imaging tests can look at how well your heart is able to pump blood, and how much the heart muscle is damaged.
Many blood tests may also be used to:
- Help diagnose and monitor heart failure
- Identify risks for various types of heart disease
- Look for possible causes of heart failure, or problems that may make your heart failure worse
- Monitor for side effects of medicines you may be taking
Treatment
MONITORING AND SELF CARE
If you have heart failure, your provider will monitor you closely. You will have follow-up visits at least every 3 to 6 months, but sometimes much more often. You will also have tests to check your heart function.
Knowing your body and the symptoms that mean your heart failure is getting worse will help you stay healthier and out of the hospital. At home, watch for changes in your heart rate, pulse, blood pressure, and weight.
Weight gain and leg swelling, especially over a few day, can be a sign that your body is holding on to extra fluid and your heart failure is getting worse. Talk to your provider about what you should do if your weight goes up or you develop more symptoms.
Limit how much salt you eat. Your provider may also ask you to limit how much fluid you drink during the day.
Other important changes to make in your lifestyle:
- Ask your provider how much alcohol you may drink.
- DO NOT smoke or use tobacco.
- Stay active. Walk or ride a stationary bicycle. Your provider can provide a safe and effective exercise plan for you. DO NOT exercise on days when your weight has gone up from fluid or you are not feeling well.
- Lose weight if you are overweight.
- Lower your cholesterol by changing your lifestyle.
- Get enough rest, including after exercise, eating, or other activities. This allows your heart to rest too.
MEDICINES, SURGERY, AND DEVICES
You will need to take medicines to treat your heart failure. Medicines treat the symptoms, prevent your heart failure from getting worse, and help you live longer. It is very important that you take your medicine as your health care team directs.
These medicines may:
- Help the heart muscle pump better
- Keep your blood from clotting
- Lower your cholesterol levels
- Open up blood vessels or slow your heart rate so your heart does not have to work as hard
- Reduce damage to your heart
- Reduce the risk for abnormal heart rhythms
- Replace potassium in your body
- Rid your body of excess fluid and salt (sodium)
It is very important that you take your medicine as directed. DO NOT take any other medicines or herbs without first asking your provider about them. Medicines that may make your heart failure worse include:
- Ibuprofen (Advil, Motrin)
- Naproxen (Aleve, Naprosyn)
The following surgeries and devices may be recommended for some people with heart failure:
- Coronary bypass surgery (CABG) or angioplasty with or without stenting may help improve blood flow to the damaged or weakened heart muscle.
- Heart valve surgery may be done if changes in a heart valve are causing your heart failure.
- A pacemaker can help treat slow heart rates or help both sides of your heart contract at the same time.
- A defibrillator sends an electrical pulse to stop life-threatening abnormal heart rhythms.
END-STAGE HEART FAILURE
Severe heart failure occurs when treatments no longer work. Certain treatments may be used when a person is waiting for (or instead of) a heart transplant:
- Intra-aortic balloon pump (IABP)
- Left or right ventricular assist device (LVAD)
- Total artificial heart
At a certain point, the provider will decide whether it is best to keep treating heart failure aggressively. The person, along with their family and providers, may want to discuss palliative or comfort care at this time.
Outlook (Prognosis)
Often, you can control heart failure by taking medicine, changing your lifestyle, and treating the condition that caused it.
Heart failure can suddenly get worse due to:
- Ischemia (lack of blood flow to the heart muscle)
- Eating high-salt foods
- Heart attack
- Infections or other illnesses
- Not taking medicines correctly
- New, abnormal heart rhythms
Most of the time, heart failure is a chronic illness. Some people develop severe heart failure that no longer responds to medicines, other treatments, and surgery.
People with heart failure may be at risk for dangerous heart rhythms. These people often receive an implanted defibrillator.
When to Contact a Medical Professional
Contact your provider if you develop:
- Increased cough or phlegm
- Sudden weight gain or swelling
- Weakness
- Other new or unexplained symptoms
Go to the emergency room or call the local emergency number (such as 911) if:
- You faint
- You have fast and irregular heartbeat (especially if you also have other symptoms)
- You feel a severe chest pain
Prevention
Most cases of heart failure can be prevented by living a healthy lifestyle and taking steps aimed at reducing your risk for heart disease.
.Alternative Names
CHF; Congestive heart failure; Left-sided heart failure; Right-sided heart failure - cor pulmonale; Cardiomyopathy - heart failure; HF
Patient Instructions
- ACE inhibitors
- Antiplatelet medicines - P2Y12 inhibitors
- Being active when you have heart disease
- Heart bypass surgery - discharge
- Heart failure - discharge
- Heart failure - fluids and diuretics
- Heart failure - home monitoring
- Heart failure - what to ask your doctor
- Heart pacemaker - discharge
- Implantable cardioverter defibrillator - discharge
References
Arnett DK, Blumenthal RS, Albert MA, et al. 2019 ACC/AHA guideline on the primary prevention of cardiovascular disease: a report of the American College of Cardiology/American Heart Association Task Force on clinical practice guidelines. Circulation. 2020;141(16):e774. PMID: 30879355 pubmed.ncbi.nlm.nih.gov/30879355/.
Felker GM, Teerlink JR. Diagnosis and management of decompensated heart failure. In: Bonow RO, Mann DL, Tomaselli, GF, et al, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine. 13th ed. Philadelphia, PA: Elsevier; 2026:chap 57.
Heidenreich PA, Bozkurt B, Aguilar D, et al. 2022 AHA/ACC/HFSA guideline for the management of heart failure: a report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. Circulation. 2022;145(18):e895-e1032. PMID: 35363499 pubmed.ncbi.nlm.nih.gov/35363499/.
Lam CSP, Shah SJ, Solomon SD. Heart failure with preserved and mildly reduced ejection fraction. In: Bonow RO, Mann DL, Tomaselli, GF, et al, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine. 13th ed. Philadelphia, PA: Elsevier; 2026:chap 59.
McMurray JJV, Pfeffer MA. Heart failure: Treatment and prognosis. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 46.
Rogers JG, O'Connor CM. Heart failure: Epidemiology, pathobiology, and diagnosis. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 45.
Wilcox JE, Mann DL. Management of heart failure patients with reduced ejection fraction. In: Bonow RO, Mann DL, Tomaselli, GF, et al, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine. 13th ed. Philadelphia, PA: Elsevier; 2026:chap 58.
Review Date 7/14/2024
Updated by: Michael A. Chen, MD, PhD, Associate Professor of Medicine, Division of Cardiology, Harborview Medical Center, University of Washington Medical School, Seattle, WA. Internal review and update on 07/01/2025 by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.