The main treatments for heart failure are making lifestyle changes and taking your medicines. However, there are procedures and surgeries that may help.
Pacemakers and Defibrillators
A heart pacemaker is a small, battery-operated device that sends a signal to your heart. The signal makes your heart beat at the correct pace.
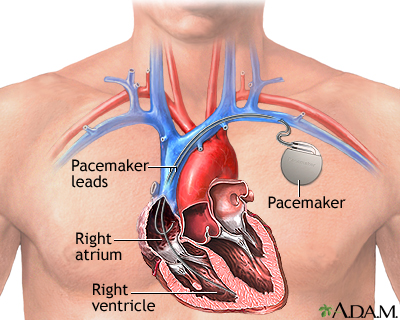
Pacemakers may be used:
- To correct abnormal heart rhythms. The heart may beat too slowly, too fast, or in an irregular manner.
- To better coordinate the beating of the heart in people with heart failure. These are called biventricular pacemakers.
When your heart is weakened, gets too large, and does not pump blood very well, you are at high risk for abnormal heartbeats that can lead to sudden cardiac death.
- An implantable cardioverter-defibrillator (ICD) is a device that can detect abnormal heart rhythms. If needed, it quickly sends an electrical shock to the heart to change the rhythm back to normal.
- Most biventricular pacemakers can also work as implantable cardio-defibrillators (ICD).
Procedures and Surgery to Improve Blood Supply to the Heart
The most common cause of heart failure is coronary artery disease (CAD), which is a narrowing of the small blood vessels that supply blood and oxygen to the heart. CAD may become worse and make it harder to manage your symptoms.
 Watch this video about:Coronary artery disease
Watch this video about:Coronary artery diseaseAfter performing certain tests, your health care provider may feel that opening a narrowed or blocked blood vessel will improve your heart failure symptoms. Suggested procedures may include:
Heart Valve Surgery
Blood that flows between the chambers of your heart, or out of your heart into the aorta, must pass through a heart valve. These valves open enough to allow blood to flow through. They then close, keeping blood from flowing backward.
When these valves do not work well (become too leaky or too narrow), blood does not flow correctly through the heart to the body. This problem may cause heart failure or make heart failure worse.
Heart valve surgery may be needed to repair or replace one of the valves.
Surgery for End-stage Heart Failure
Some types of surgery are done for severe heart failure when other treatments no longer work. These procedures are often used when a person is waiting for a heart transplant. They are also sometimes used long term in cases when transplant is not planned or possible.
Examples of some of these devices include left ventricular assist devices (LVAD), right ventricular assist devices (RVAD), or a total artificial hearts. They are considered for use if you have severe heart failure that cannot be controlled with medicine or a special pacemaker.
- A ventricular assist device (VAD) helps your heart pump blood from the pumping chambers of your heart to either the lungs or to the rest of your body. These pumps may be implanted in your body or connected to a pump outside your body.
- You may be on a waiting list for a heart transplant. Some people who get a VAD are very ill and may already be on a heart-lung bypass machine.
- Total artificial hearts are being developed, but are not yet in wide use.
Devices inserted through a catheter such as intra-aortic balloon pumps (IABP) are sometimes used.
- An IABP is a thin balloon that is inserted into an artery (most often in the leg) and threaded into the main artery exiting the heart (aorta).
- These devices can help maintain heart function in the short term. Because they can be placed quickly, they are useful for people who have a sudden and severe decline in heart function
- They are used in people who are waiting for recovery or for more advanced assist devices.
Alternative Names
CHF - surgery; Congestive heart failure - surgery; Cardiomyopathy - surgery; HF - surgery; Intra-aortic balloon pumps - heart failure; IABP - heart failure; Catheter based assist devices - heart failure
References
Aaronson KD, Pagani FD. Mechanical circulatory support. In: Libby P, Bonow RO, Mann DL, Tomaselli GF, Bhatt DL, Solomon SD, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine. 12th ed. Philadelphia, PA: Elsevier; 2022:chap 59.
Ewald GA, Milano CA, Rogers JG. Circulatory assist devices in heart failure. In: Felker GM, Mann DL, eds. Heart Failure: A Companion to Braunwald's Heart Disease. 4th ed. Philadelphia, PA: Elsevier, 2020:chap 45.
Heidenreich PA, Bozkurt B, Aguilar D, et al. 2022 AHA/ACC/HFSA guideline for the management of heart failure: a report of the American College of Cardiology/American Heart Association Joint Committee on clinical practice guidelines. J Am Coll Cardiol. 2023;81(15):1551. PMID: 35379503 pubmed.ncbi.nlm.nih.gov/35379503/.
Mann DL. Management of heart failure patients with reduced ejection fraction. In: Libby P, Bonow RO, Mann DL, Tomaselli GF, Bhatt DL, Solomon SD, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine. 12th ed. Philadelphia, PA: Elsevier; 2022:chap 50.
McMurray JJV, Pfeffer MA. Heart failure: treatment and prognosis. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 46.
Otto CM, Nishimura RA, Bonow RO, et al. 2020 ACC/AHA guideline for the management of patients with valvular heart disease: executive summary: a report of the American College of Cardiology/American Heart Association Joint Committee on clinical practice guidelines. Circulation. 2021;143(10):e784. PMID: 33332149 pubmed.ncbi.nlm.nih.gov/33332149/.
Review Date 5/5/2025
Updated by: Michael A. Chen, MD, PhD, Associate Professor of Medicine, Division of Cardiology, Harborview Medical Center, University of Washington Medical School, Seattle, WA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.


