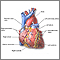
Heart bypass surgery creates a new route, called a bypass, for blood and oxygen to go around a blockage to reach your heart.
 Watch this video about:Heart bypass surgery
Watch this video about:Heart bypass surgeryDescription
Before your surgery, you will get general anesthesia. You will be asleep (unconscious) and pain-free during surgery.
Once you are unconscious, most often, the heart surgeon will make an 8 to 10-inch (20 to 25 cm) surgical cut in the middle of your chest. Your breastbone will be separated to create an opening. This allows your surgeon to see your heart and aorta, the main blood vessel leading from the heart to the rest of your body.
Most people who have heart bypass surgery are connected to a heart-lung bypass machine or bypass pump.
- Your heart is stopped while you are connected to this machine.
- This machine does the work of your heart and lungs while your heart is stopped for the surgery. The machine adds oxygen to your blood, moves blood through your body, and removes carbon dioxide.
Another type of bypass surgery does not use the heart-lung bypass machine. The procedure is done while your heart is still beating. This is called off-pump coronary artery bypass, or OPCAB.
During bypass surgery:
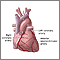
- The surgeon will take a vein or artery from another part of your body and use it to make a detour (or graft) around the blocked area in your artery. Your surgeon may use a vein, called the saphenous vein, from your leg.
- To reach this vein, a surgical cut will be made along the inside of your leg, between your ankle and groin. One end of the graft will be sewn to your coronary artery. The other end will be sewn to an opening made in your aorta.
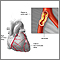
- A blood vessel in your chest, called the internal mammary artery (IMA), can also be used as the graft. One end of this artery is already connected to a branch of your aorta. The other end is attached to your coronary artery.
- Other arteries can also be used for grafts in bypass surgery. The most common one is the radial artery in your wrist.
After the graft has been created, your breastbone will be closed with wires, or if a different approach was used that would be closed as well. These wires stay inside you. The surgical cut will be closed with stitches.
This surgery can take 4 to 6 hours or longer, particularly if other procedures are performed (such as heart valve surgery). After the surgery, you will be taken to the intensive care unit.
Why the Procedure is Performed
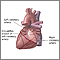
You may need this procedure if you have a blockage in one or more of your coronary arteries. Coronary arteries are the vessels that supply your heart with oxygen and nutrients that are carried in your blood.
When one or more of the coronary arteries becomes partly or totally blocked, your heart does not get enough blood. This is called ischemic heart disease, or coronary artery disease (CAD). It can cause chest pain (angina).
Coronary artery bypass surgery can be used to improve blood flow to your heart. Your health care provider may have first tried to treat you with medicines. You may have also tried exercise and diet changes, or coronary artery angioplasty with stenting.
CAD is different from person to person. The way it is diagnosed and treated will also vary. Heart bypass surgery is just one type of treatment.
Other procedures that may be used:
Risks
Risks for any surgery include:
- Bleeding
- Infection
- Death
Possible risks from having coronary bypass surgery include:
- Infection, including chest wound infection, which is more likely to happen if you are obese, have diabetes, or have already had this surgery
- Heart attack
- Stroke
- Heart rhythm problems
- Kidney failure
- Lung failure
- Depression and mood swings
- Low fever, tiredness, and chest pain, together called postpericardiotomy syndrome, which can last up to 6 months
- Memory loss, loss of mental clarity, or "fuzzy thinking"
Before the Procedure
Tell your surgeon or nurse if you are taking any medicines, including medicines, drugs, supplements, or herbs you bought without a prescription.
During the week before your surgery:
- You may be asked to temporarily stop taking medicines that keep your blood from clotting. These medicines are called blood thinners. This includes over-the-counter medicines and supplements such as aspirin, ibuprofen (Advil, Motrin), naproxen (Aleve, Naprosyn), and vitamin E. Many prescription medicines are also blood thinners.
- Ask your surgeon which medicines you should still take on the day of surgery.
On the day of surgery:
- Follow instructions about when to stop eating and drinking.
- Take the medicines your surgeon told you to take with a small sip of water.
- Arrive at the hospital on time.
After the Procedure
After the operation, you will spend 3 to 7 days in the hospital. You will spend the first night in an intensive care unit (ICU). You will probably be moved to a regular or transitional care room within 24 to 48 hours after the procedure.
Two to three tubes will be in your chest to drain fluid from around your heart. They are most often removed 1 to 3 days after surgery.
You may have a catheter (flexible tube) in your bladder to drain urine. You may also have intravenous (IV) lines for fluids. You will be attached to machines that monitor your pulse, temperature, and breathing. Nurses will constantly watch your monitors.
You may have several small wires that are connected to a pacemaker, which are pulled out prior to your discharge.
You will be encouraged to restart some activities and you may begin a cardiac rehabilitation program within a few days.
It takes 4 to 6 weeks to start feeling better after surgery. Your providers will tell you how to take care of yourself at home after the surgery.
Outlook (Prognosis)
Recovery from surgery takes time. You may not see the full benefits of your surgery for 3 to 6 months. In most people who have heart bypass surgery, the grafts stay open and work well for many years.
This surgery does not prevent the coronary artery blockage from coming back. You can do many things to slow this process down, including:
- Not smoking
- Eating a heart-healthy diet
- Getting regular exercise
- Treating high blood pressure
- Controlling high blood sugar (diabetes) and high cholesterol
- Taking your medicines as prescribed
Alternative Names
Off-pump coronary artery bypass; OPCAB; Beating heart surgery; Bypass surgery - heart; CABG; Coronary artery bypass graft; Coronary artery bypass surgery; Coronary bypass surgery; Coronary artery disease - CABG; CAD - CABG; Angina - CABG
Patient Instructions
- Angina - discharge
- Angina - what to ask your doctor
- Angina - when you have chest pain
- Angioplasty and stent - heart - discharge
- Antiplatelet medicines - P2Y12 inhibitors
- Aspirin and heart disease
- Bathroom safety for adults
- Being active after your heart attack
- Being active when you have heart disease
- Butter, margarine, and cooking oils
- Cardiac catheterization - discharge
- Cholesterol and lifestyle
- Cholesterol - drug treatment
- Controlling your high blood pressure
- Dietary fats explained
- Fast food tips
- Heart attack – discharge
- Heart attack - what to ask your provider
- Heart bypass surgery - discharge
- Heart disease - risk factors
- Heart pacemaker - discharge
- How to read food labels
- Low-salt diet
- Mediterranean diet
- Preventing falls
- Surgical wound care - open
- When you have nausea and vomiting
References
Doenst T, Taggart D, Gaudino MFL. Coronary artery bypass grafting. In: Sellke FW, del Nido PJ, Swanson SJ, eds. Sabiston and Spencer Surgery of the Chest. 10th ed. Philadelphia, PA: Elsevier; 2024:chap 91.
Lawton JS, Tamis-Holland JE, Bangalore S, et al. 2021 ACC/AHA/SCAI guideline for coronary artery revascularization: a report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. Circulation. 2022;145(3):e18-e114. PMID: 34882435 pubmed.ncbi.nlm.nih.gov/34882435/.
Morrow DA, de Lemos JA. Stable ischemic heart disease. In: Libby P, Bonow RO, Mann DL, Tomaselli GF, Bhatt DL, Solomon SD, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine. 12th ed. Philadelphia, PA: Elsevier; 2022:chap 40.
Teirstein PS, Kirtane AJ. Interventional diagnosis and treatment of coronary artery disease. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024;chap 59.
Review Date 5/5/2025
Updated by: Michael A. Chen, MD, PhD, Associate Professor of Medicine, Division of Cardiology, Harborview Medical Center, University of Washington Medical School, Seattle, WA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.