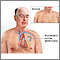
An implantable cardioverter-defibrillator (ICD) is a device that detects a life-threatening, abnormal heartbeat. If it occurs, the device sends an electrical shock to the heart to change the rhythm back to normal. This article discusses what you need to know after you have had an ICD inserted.
Note: Care of certain special defibrillators may be different than described below.
When You're in the Hospital
A type of heart specialist cardiologist)called an electrophysiologist or a surgeon made a small incision (cut) in your chest wall. A device called an ICD was inserted under your skin and muscle. The ICD is the size of a large cookie. Leads, or electrodes, were placed in your heart and were connected to your ICD.
The ICD can quickly detect life-threatening abnormal heartbeats (arrhythmias). It is designed to convert any abnormal heart rhythm back to normal by sending an electrical shock to your heart. This action is called defibrillation. This device can also work as a pacemaker.
What to Expect at Home
When you leave the hospital, you will be given a card to keep in your wallet. This card lists the details of your ICD and has contact information for emergencies.
Carry your ICD identification card with you AT ALL TIMES. The information it contains will tell all health care providers you see what type of ICD you have. Not all ICDs are the same. You should know what type of ICD you have and which company made it. This can let other providers check the device to see if it works right.
Wound Care
You should be able to do most of your normal activities within 3 to 4 days after surgery. But you will have some limits for up to 4 to 6 weeks.
Do not do these things for 2 to 3 weeks:
- Lift anything heavier than 10 to 15 pounds (4.5 to 7 kilograms)
- Push, pull, or twist too much
- Wear clothes that rub on the wound
Keep your incision completely dry for 4 to 5 days. After that, you may take a shower and pat it dry. Always wash your hands before touching the wound.
For 4 to 6 weeks, do not lift your arm higher than your shoulder on the side of your body where your ICD was placed.
Follow-up
You will need to see your cardiologist regularly for monitoring. Your cardiologist will make sure your ICD is working correctly and will check to see how many shocks it has sent and how much power is left in the battery. Your first follow-up visit will probably be about 1 month after your ICD is placed.
ICD batteries are designed to last 4 to 8 years. Regular checks of the battery are needed to see how much power it has left. You will need minor surgery to replace your ICD when the battery begins to run down.
Be Careful Around Things With Magnets
Most devices will not interfere with your defibrillator, but some with strong magnetic fields might. Ask your cardiologist if you have questions about any specific device.
Most appliances in your home are safe to be around. This includes your refrigerator, washer, dryer, toaster, blender, personal computer and fax machine, hair dryer, stove, CD player, remote controls, and microwave.
There are several devices you should keep at least 12 inches (30.5 centimeters) away from the site where your ICD is placed under your skin. These include:
- Battery-powered cordless tools (such as screwdrivers and drills)
- Plug-in power tools (such as drills and table saws)
- Electric lawnmowers and leaf blowers
- Slot machines
- Stereo speakers
Tell all providers that you have an ICD. Some medical equipment may harm your ICD. Because MRI machines have powerful magnets, talk to your provider before having an MRI.
Stay away from large motors, generators, and equipment. Do not lean over the open hood of a running car. Also stay away from:
- Radio transmitters and high-voltage power lines
- Products that use magnetic therapy, such as some mattresses, pillows, and massagers
- Electrical or gasoline-powered appliances
If you have a cell phone:
- Do not put it in a pocket on the same side of your body as your ICD.
- When using your cell phone, hold it to your ear on the opposite side of your body.
Be careful around metal detectors and security wands.
- Handheld security wands may interfere with your ICD. Show your wallet card and ask to be hand searched.
- Most security gates at airports and stores are OK. But do not stand near these devices for long periods. Your ICD may set off alarms.
When to Call the Doctor
Tell your cardiologist about every shock you feel from your ICD. The settings of your ICD may need to be adjusted, or your medicines may need to be changed.
Also contact your cardiologist if:
- Your wound looks infected. Signs of infection are redness, increased drainage, swelling, and pain.
- You are having the symptoms you had before your ICD was implanted.
- You are dizzy, have chest pain, or are short of breath.
- You have hiccups that do not go away.
- You were unconscious for a moment.
- Your ICD has sent a shock and you still do not feel well or you pass out. Talk to your provider about when to call the office or 911 or the local emergency number.
Alternative Names
ICD - discharge; Defibrillation - discharge; Arrhythmia - ICD discharge; Abnormal heart rhythm - ICD discharge; Ventricular fibrillation - ICD discharge; VF - ICD discharge; V Fib - ICD discharge
References
Al-Khatib SM, Stevenson WG, Ackerman MJ, et al. 2017 AHA/ACC/HRS guideline for management of patients with ventricular arrhythmias and the prevention of sudden cardiac death: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines and the Heart Rhythm Society. J Am Coll Cardiol. 2018;72(14):e91-e220. PMID: 29097296 pubmed.ncbi.nlm.nih.gov/29097296/.
Chung MK, Daubert JP. Pacemakers and implantable cardioverter-defibrillators. In: Libby P, Bonow RO, Mann DL, Tomaselli GF, Bhatt DL, Solomon SD, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine. 12th ed. Philadelphia, PA: Elsevier; 2022:chap 69.
Glikson M, Nielsen JC, Kronborg MB, et al. 2021 ESC Guidelines on cardiac pacing and cardiac resynchronization therapy: Developed by the Task Force on cardiac pacing and cardiac resynchronization therapy of the European Society of Cardiology (ESC) With the special contribution of the European Heart Rhythm Association (EHRA). European Heart Journal. 2021;42(35):3427-3520. PMID: 34455430 pubmed.ncbi.nlm.nih.gov/34455430/.
Miller JM, Ellenbogen KA. Therapy for cardiac arrhythmias. In: Libby P, Bonow RO, Mann DL, Tomaselli GF, Bhatt DL, Solomon SD, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine. 12th ed. Philadelphia, PA: Elsevier; 2022:chap 64.
Santucci PA, Wilber DJ. Electrophysiologic interventional procedures and surgery. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 54.
Swerdlow C, Ploux S. Transvenous implantable cardiac defibrillator: clinical aspects. In: Jalife J, Stevenson WG, eds. Zipes and Jalife's Cardiac Electrophysiology: From Cell to Bedside. 8th ed. Philadelphia, PA: Elsevier; 2022:chap 122.
Patient Instructions
Review Date 7/14/2024
Updated by: Michael A. Chen, MD, PhD, Associate Professor of Medicine, Division of Cardiology, Harborview Medical Center, University of Washington Medical School, Seattle, WA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.