You should visit your health care provider regularly, even if you feel healthy. The purpose of these visits is to:
- Screen for medical issues
- Assess your risk for future medical problems
- Encourage a healthy lifestyle
- Update vaccinations and other preventive care services
- Help you get to know your provider in case of an illness
Information
Even if you feel fine, you should still see your provider for regular checkups. These visits can help you avoid problems in the future. For example, the only way to find out if you have high blood pressure is to have it checked regularly. High blood sugar and high cholesterol level also may not have any symptoms in the early stages. Simple blood tests can check for these conditions.
There are specific times when you should see your provider or receive specific health screenings. The US Preventive Services Task Force (USPSTF) publishes a list of recommended screenings, and these are updated as needed. Below are screening guidelines for men ages 40 to 64.
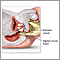
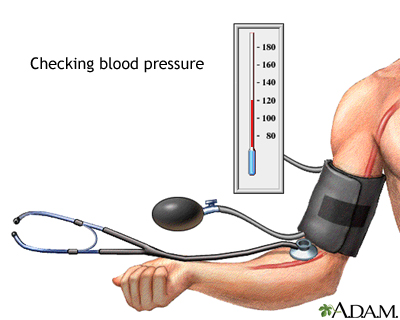
BLOOD PRESSURE SCREENING
Have your blood pressure checked at least once every year. Watch for blood pressure screenings in your area. Ask your provider if you can stop in to have your blood pressure checked. You can also check your blood pressure using the automated machines at some local grocery stores and pharmacies.
Ask your provider if you need your blood pressure checked more often if:
- You have diabetes, heart disease, kidney problems, are overweight or have obesity, or have certain other health conditions
- You have a first-degree relative with high blood pressure
- You are Black
- Your blood pressure top number is from 120 to 129 mm Hg, or the bottom number is from 70 to 79 mm Hg
If the top number is 130 mm Hg or greater, but lower than 140 mm Hg, or the bottom number is 80 mm Hg or greater, but lower than 90 mm Hg, this is considered stage 1 hypertension. Readings above these are considered stage 2 hypertension. Schedule an appointment with your provider to learn how you can reduce your blood pressure. Record your blood pressure numbers and bring this information to share with your provider.
CHOLESTEROL SCREENING
The American Heart Association recommends beginning cholesterol screening at age 20 for all men with no known risk factors for coronary heart disease and repeat every 4 to 6 years.
Cholesterol screening should take place more often if:
- Changes occur in lifestyle (including weight gain and diet)
- You have diabetes, heart disease, kidney problems, high blood pressure, stroke, blood flow problems in the legs or feet, or certain other conditions
- Your provider recommends it because you are taking medicines to control high cholesterol
COLORECTAL CANCER SCREENING
If you are under age 45, talk to your provider about getting screened. You may need to be screened if you have a strong family history of colon cancer or polyps. Screening may also be considered if you have risk factors such as a history of inflammatory bowel disease or polyps.
If you are age 45 to 75, you should be screened for colorectal cancer. There are several screening tests available:
- Colonoscopy every 10 years
- A stool-based fecal occult blood (FOBT) or fecal immunochemical test (FIT) every year
- A stool DNA test every 1 to 3 years
- Flexible sigmoidoscopy every 5 years or every 10 years with FIT) done every year
- CT colonography (virtual colonoscopy) every 5 years
You may need a colonoscopy more often if you have risk factors for colorectal cancer, such as:
- Ulcerative colitis or Crohn disease
- A personal or family history of colorectal cancer or polyps
- A family history of inherited colorectal cancer syndromes such as familial adenomatous polyps (FAP) or hereditary nonpolyposis colorectal cancer (HNPCC)
DENTAL EXAM
- Go to the dentist once or twice every year for an exam and cleaning. Your dentist will evaluate if you have a need for more frequent visits.
PREDIABETES AND TYPE 2 DIABETES SCREENING
You should be screened for prediabetes and type 2 diabetes starting at age 35 if you are overweight or have obesity. Screening should be repeated every 3 years if you still are overweight or have obesity.
Screening may need to start earlier and be repeated more often if you have other risk factors for diabetes, such as:
- You have a first degree relative with diabetes
- You have high blood pressure, prediabetes, or a history of heart disease
EYE EXAM
- Have an eye exam every 2 to 4 years ages 40 to 54 and every 1 to 3 years ages 55 to 64. Your provider may recommend more frequent eye exams if you have vision problems or glaucoma risk.
- Have an eye exam that includes an examination of your retina (back of your eye) at least every year if you have diabetes.
IMMUNIZATIONS
Commonly recommended vaccines include:
- Flu shot: you should get one every year.
- COVID-19 vaccine: recommended for all people age 6 months and older. Talk with your provider about what is best for you.
- Tetanus-diphtheria and acellular pertussis (Tdap) vaccine: have Tdap as one of your tetanus-diphtheria vaccines if you did not receive it as an adolescent.
- Tetanus-diphtheria: have a booster (Td or Tdap) every 10 years.
- Varicella vaccine: receive 2 doses if you never had chickenpox or the varicella vaccine and were born in 1980 or after.
- Hepatitis B vaccine: receive 2, 3, or 4 doses, depending on your exact circumstances, if you did not receive these as a child or adolescent, until age 59.
- Measles, mumps, and rubella (MMR) vaccine: receive 1 to 2 doses if you are not already immune to MMR. Your provider can tell you if you are immune.
- Shingles (herpes zoster) vaccine: 2 doses at or after age 50.
Ask your provider if you should receive other immunizations, especially if you have certain medical conditions, such as diabetes or are at increased risk for some diseases such as pneumonia.
INFECTIOUS DISEASE SCREENING
- All adults ages 18 to 79 should get a one-time test for hepatitis C.
- All people ages 15 to 65 should get a one-time test for human immunodeficiency virus (HIV).
- Annual HIV screening is recommended for people at increased risk, such as being sexually active with men of unknown HIV status or having other risk factors such as injection drug use.
Depending on your lifestyle and medical history, you may need to be screened for infections such as syphilis, chlamydia, and other infections.
LUNG CANCER SCREENING
You should have an annual screening for lung cancer with low-dose computed tomography (LDCT) if:
- You are age 50 to 80 years AND
- You have a 20 pack-year smoking history AND
- You currently smoke or have quit within the past 15 years
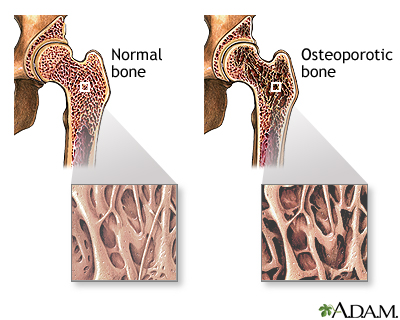
OSTEOPOROSIS SCREENING
- If you are age 50 to 69 and have risk factors for osteoporosis, you should discuss screening with your provider.
- Risk factors can include long-term steroid use, low body weight, smoking, heavy alcohol use, having a fracture after age 50, or a family history of hip fracture or osteoporosis.
PHYSICAL EXAM
Your blood pressure, height, weight, and body mass index (BMI) should be checked at every exam.
During your exam, your provider may ask you about:
- Depression and anxiety
- Diet and exercise
- Alcohol, tobacco, and drug use
- Safety, such as use of seat belts and smoke detectors
- Your medicines and risk for interactions
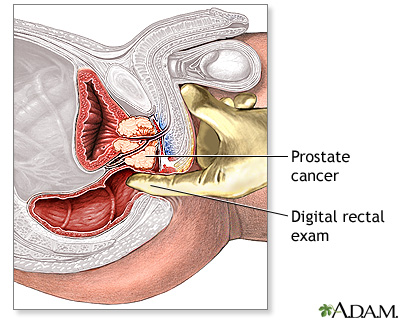
PROSTATE CANCER SCREENING
If you're 55 through 69 years old, before having the test, talk to your provider about the pros and cons of having a prostate specific antigen (PSA) blood test. Ask about:
- Whether screening decreases your chance of dying from prostate cancer
- Whether there is any harm from prostate cancer screening, such as side effects from testing or overtreatment of cancer when discovered
- Whether you have a higher risk of prostate cancer than others
If you are younger than age 55, screening is not generally recommended. You should talk with your provider about if you have a higher risk for prostate cancer. Risk factors include:
- Having a family history of prostate cancer (especially a brother or father who were diagnosed before age 65)
- Being African American
If you choose to be tested, the PSA blood test is repeated over time (yearly or less often), though the best frequency is not known.
Prostate physical examinations are no longer routinely done on men with no symptoms.
SKIN EXAM
- Have had skin cancer before
- Have close relatives with skin cancer
- Have a weakened immune system
Professional organizations do not recommend for or against performing a skin self-exam.
TESTICULAR EXAM
The USPSTF recommends against performing testicular screening. Doing testicular exams has been shown to have little to no benefit.
Alternative Names
Health maintenance visit - men - ages 40 to 64; Physical exam - men - ages 40 to 64; Yearly exam - men - ages 40 to 64; Checkup - men - ages 40 to 64; Men's health - ages 40 to 64; Preventive care - men - ages 40 to 64
References
American Academy of Ophthalmology website. Clinical statement: Comprehensive adult medical eye examination PPP 2020. www.aao.org/education/preferred-practice-pattern/comprehensive-adult-medical-eye-evaluation-ppp. Updated November 2020. Accessed October 24, 2025.
American Dental Association website. Your top 9 questions about going to the dentist - answered! www.mouthhealthy.org/en/dental-care-concerns/questions-about-going-to-the-dentist. Accessed October 24, 2025.
American Diabetes Association Professional Practice Committee. 2. Diagnosis and Classification of Diabetes: Standards of Care in Diabetes-2025. Diabetes Care. 2025 Jan 1;48(1 Suppl 1):S27-S49. doi: 10.2337/dc25-S002. PMID: 39651986; PMCID: PMC11635041 pubmed.ncbi.nlm.nih.gov/39651986/.
American Heart Association website. How to get your cholesterol tested. www.heart.org/en/health-topics/cholesterol/how-to-get-your-cholesterol-tested. Last reviewed February 19, 2024. Accessed November 1, 2025.
Barton MB, Wolff TA. The preventive health visit. In: Goldman L, Cooney K, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 12.
Bushnell C, Kernan WN, Sharrief AZ, et al. 2024 Guideline for the primary prevention of stroke: a guideline from the American Heart Association/American Stroke Association. Stroke. 2024;55(12):e344-e424. PMID: 39429201 pubmed.ncbi.nlm.nih.gov/39429201/.
Centers for Disease Control and Prevention website. Vaccines & immunizations. Adult immunization schedule by age (Addendum updated June 27, 2024). Recommendations for ages 19 years or older, United States, 2024. www.cdc.gov/vaccines/hcp/imz-schedules/adult-age.html. Updated July 1, 2025. Accessed October 24, 2025.
Grundy SM, Stone NJ, Bailey AL, et al. 2018 AHA/ACC/AACVPR/AAPA/ABC/ACPM/ADA/AGS/APhA/ASPC/NLA/PCNA Guideline on the management of blood cholesterol: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines [published correction appears in J Am Coll Cardiol. 201925;73(24):3237-3241]. J Am Coll Cardiol. 2019;73(24):e285-e350. PMID: 30423393 pubmed.ncbi.nlm.nih.gov/30423393/.
Mora S, Libby P, Ridker PM. Primary prevention of cardiovascular disease. In: Libby P, Bonow RO, Mann DL, Tomaselli GF, Bhatt DL, Solomon SD, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine. 12th ed. Philadelphia, PA: Elsevier; 2022:chap 25.
US Preventive Services Task Force website. A and B recommendations. www.uspreventiveservicestaskforce.org/uspstf/recommendation-topics/uspstf-a-and-b-recommendations. Accessed October 24, 2025.
US Preventive Services Task Force website. Final recommendation statement. Colorectal cancer: screening. www.uspreventiveservicestaskforce.org/uspstf/recommendation/colorectal-cancer-screening. Published May 18, 2021. Accessed October 24, 2025.
US Preventive Services Task Force website. Final recommendation statement. Falls prevention in community-dwelling older adults: Interventions. www.uspreventiveservicestaskforce.org/uspstf/recommendation/falls-prevention-community-dwelling-older-adults-interventions. Published June 4, 2024. Accessed October 24, 2025.
US Preventive Services Task Force website. Final recommendation statement. Hepatitis C virus infection in adolescents and adults: screening. www.uspreventiveservicestaskforce.org/uspstf/recommendation/hepatitis-c-screening. Published March 2, 2020. Accessed October 24, 2025.
US Preventive Services Task Force website. Final recommendation statement. Human immunodeficiency virus (HIV) infection: screening. www.uspreventiveservicestaskforce.org/uspstf/recommendation/human-immunodeficiency-virus-hiv-infection-screening. Published June 11, 2019. Accessed October 24, 2025.
US Preventive Services Task Force website. Final recommendation statement. Hypertension in adults: screening. www.uspreventiveservicestaskforce.org/uspstf/recommendation/hypertension-in-adults-screening. Published April 27, 2021. Accessed October 24, 2025.
US Preventive Services Task Force website. Final recommendation statement. Lung cancer: screening. www.uspreventiveservicestaskforce.org/uspstf/recommendation/lung-cancer-screening. Updated March 9, 2021. Accessed October 24, 2025.
US Preventive Services Task Force website. Final recommendation statement. Osteoporosis to prevent fracture: screening. www.uspreventiveservicestaskforce.org/uspstf/recommendation/osteoporosis-screening. Updated June 26, 2018. Accessed October 24, 2025.
US Preventive Services Task Force website. Final recommendation statement. Prediabetes and type 2 diabetes: screening. www.uspreventiveservicestaskforce.org/uspstf/recommendation/screening-for-prediabetes-and-type-2-diabetes. Updated August 24, 2021. Accessed October 24, 2025.
US Preventive Services Task Force website. Final recommendation statement. Prostate cancer: screening. www.uspreventiveservicestaskforce.org/uspstf/recommendation/prostate-cancer-screening. Updated May 8, 2018. Accessed October 24, 2025.
US Preventive Services Task Force website. Final recommendation statement. Skin cancer: screening. www.uspreventiveservicestaskforce.org/uspstf/recommendation/skin-cancer-screening. Updated April 18, 2023. Accessed October 24, 2025.
US Preventive Services Task Force website. Final recommendation statement. Testicular cancer: screening. www.uspreventiveservicestaskforce.org/uspstf/recommendation/testicular-cancer-screening. Published April 15, 2011. Accessed October 24, 2025.
Whelton PK, Carey RM, Mancia G, Kreutz R, Bundy JD, Williams B. Harmonization of the American College of Cardiology/American Heart Association and European Society of Cardiology/European Society of Hypertension Blood Pressure/Hypertension Guidelines: Comparisons, Reflections, and Recommendations. Circulation. 2022;146:868–877. DOI: 10.1161/CIRCULATIONAHA.121.054602. PMID: 35950927 pubmed.ncbi.nlm.nih.gov/35950927/.
Test Your Knowledge
Review Date 6/24/2025
Updated by: Frank D. Brodkey, MD, FCCM, Associate Professor, Section of Pulmonary and Critical Care Medicine, University of Wisconsin School of Medicine and Public Health, Madison, WI. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.