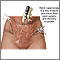
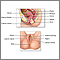
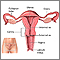
Pelvic inflammatory disease (PID) is an infection of a woman's womb (uterus), ovaries, or fallopian tubes.
Causes
PID is an infection caused by bacteria. When bacteria from the vagina or cervix travel to your womb, fallopian tubes, or ovaries, they can cause an infection.
Most of the time, PID is caused by the bacteria chlamydia or gonorrhea. These are sexually transmitted infections (STIs). Having unprotected sex with someone who has an STI can cause PID.
Bacteria normally found in the cervix can also travel into the uterus and fallopian tubes during a medical procedure such as:
- Childbirth
- Endometrial biopsy (removing a small piece of your womb lining to test for cancer)
- Getting an intrauterine device (IUD)
- Miscarriage
- Abortion
In the United States, nearly 1 million women have PID each year. About 1 in 8 sexually active women will have PID before age 20.
You are more likely to get PID if:
- You have a sex partner with gonorrhea or chlamydia.
- You have sex with many different people.
- You have had an STI in the past.
- You have recently had PID.
- You have contracted gonorrhea or chlamydia and have an IUD.
- You have had sex before age 20.
Symptoms
Common symptoms of PID include:
- Fever
- Pain or tenderness in the pelvis, lower belly, or lower back
- Fluid from your vagina that has an unusual color, texture, or smell
Other symptoms that may occur with PID:
- Bleeding after intercourse
- Chills
- Being very tired
- Pain when you urinate
- Having to urinate often
- Period cramps that hurt more than usual or last longer than usual
- Unusual bleeding or spotting during your period
- Not feeling hungry
- Nausea and vomiting
- Skipping your period
- Pain when you have intercourse
You can have PID and not have any severe symptoms. For example, chlamydia can cause PID with no symptoms. Women who have an ectopic pregnancy or who are infertile often have had PID caused by chlamydia. An ectopic pregnancy is when an egg grows outside of the uterus. It puts the mother's life in danger.
Exams and Tests
Your health care provider may do a pelvic exam to look for:
- Bleeding from your cervix. The cervix is the opening to your uterus.
- Fluid coming out of your cervix.
- Pain when your cervix is touched.
- Tenderness in your uterus, tubes, or ovaries.
You may have lab tests to check for signs of body-wide infection:
Other tests include:
- A swab taken of your vagina or cervix. This sample will be checked for gonorrhea, chlamydia, or other causes of PID.
- Pelvic ultrasound or CT scan to see what else may be causing your symptoms. Appendicitis or pockets of infection around your tubes and ovaries, called tubo-ovarian abscess (TOA), may cause similar symptoms.
- Pregnancy test.
Treatment
Your provider will often have you start taking antibiotics while waiting for your test results.
If you have mild PID:
- Your provider will give you a shot containing an antibiotic.
- You will be sent home with antibiotic pills to take for up to 2 weeks.
- You will need to follow-up closely with your provider.
If you have more severe PID:
- You may need to stay in the hospital.
- You may be given antibiotics through a vein (IV).
- Later, you may be given antibiotic pills to take by mouth.
There are many different antibiotics that can treat PID. Some are safe for pregnant women. Which type you take depends on the cause of the infection. You may receive a different treatment if you have gonorrhea or chlamydia.
Finishing the full course of antibiotics you've been given is extremely important for treating PID. Scarring inside the womb or of the tubes from PID may lead to the need to have surgery or undergo invitro fertilization (IVF) to become pregnant. Follow up with your provider after you've finished the antibiotics to make sure that you no longer have the bacteria in your body.
It's very important that you practice safer sex in order to reduce your risk of getting infections, which could lead to PID.
If your PID is caused by an STI like gonorrhea or chlamydia, your sexual partner must be treated as well.
- If you have more than one sexual partner, they must all be treated.
- If your partner is not treated, they can infect you again, or can infect other people in the future.
- Both you and your partner must finish taking all of the prescribed antibiotics.
- Use condoms until you both have finished taking antibiotics.
Possible Complications
PID infections can cause scarring of the pelvic organs. This can lead to:
- Long-term (chronic) pelvic pain
- Ectopic pregnancy
- Infertility
- Tubo-ovarian abscess
If you have a serious infection that does not improve with antibiotics, you may need surgery.
When to Contact a Medical Professional
Contact your provider if:
- You have symptoms of PID.
- You think you have been exposed to an STI.
- Treatment for a current STI does not seem to be working.
Prevention
Get prompt treatment for STIs.
You can help prevent PID by practicing safer sex.
- The only guaranteed way to prevent an STI is to not have sex (abstinence).
- You can reduce your risk by having a sexual relationship with only one person. This is called being monogamous.
- Your risk will also be reduced if you and your sexual partners get tested for STIs before starting a sexual relationship.
- Using a condom every time you have sex also reduces your risk.
Here is how you can reduce your risk for PID:
- Get regular STI screening tests.
- If you are a new couple, get tested before starting to have sex. Testing can detect infections that are not causing symptoms.
- If you are a sexually active woman age 24 or younger, get screened each year for chlamydia and gonorrhea.
- All women with new sexual partners or multiple partners should also be screened.
- Use of oral contraception also significantly reduces the risks of PID.
Alternative Names
PID; Oophoritis; Salpingitis; Salpingo - oophoritis; Salpingo - peritonitis
References
Centers for Disease Control and Prevention website. Sexually transmitted infections treatment guidelines, 2021. www.cdc.gov/std/treatment-guidelines/default.htm. Updated June 13, 2023. Accessed August 29, 2025.
Dionne JA, Marrazzo JM. Infections of the female pelvis. In: Blaser MJ, Cohen JI, Holland SM, et al, eds. Mandell, Douglas, and Bennett's Principles and Practice of Infectious Diseases. 10th ed. Philadelphia, PA: Elsevier; 2026:chap 111.
Eckert LO, Lentz GM. Genital tract infections: vulva, vagina, cervix, toxic shock syndrome, endometritis, and salpingitis. In: Gershenson DM, Lentz GM, Valea FA, Lobo RA, eds. Comprehensive Gynecology. 8th ed. Philadelphia, PA: Elsevier; 2022:chap 23.
Lipsky AM, Hart D. Acute pelvic pain. In: Walls RM, ed. Rosen's Emergency Medicine: Concepts and Clinical Practice. 10th ed. Philadelphia, PA: Elsevier; 2023:chap 29.
Seña AC, Swygard H, Cohen MS. Approach to the patient with a sexually transmitted infection. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 264.
Review Date 8/18/2025
Updated by: LaQuita Martinez, MD, Department of Obstetrics and Gynecology, Emory Johns Creek Hospital, Alpharetta, GA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.