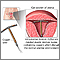
An intrauterine device (IUD) is a small plastic T-shaped device used for birth control. It is inserted into the uterus (womb) where it stays to prevent pregnancy.
Description
An IUD is often inserted by your health care provider during your monthly period. Any type of IUD can be inserted quickly and easily in the provider's office or clinic. Before placing the IUD, the provider washes the cervix with an antiseptic solution. After this, the provider:
- Slides a plastic tube containing the IUD through the vagina and into the uterus.
- Pushes the IUD into the uterus with the help of a plunger.
- Removes the tube, leaving two small strings that dangle outside the cervix within the vagina.
The strings have two purposes:
- They let the provider or woman check that the IUD stays properly in position.
- They are used to pull the IUD out of the uterus when it is time to remove it. This should only be done by a provider.
This procedure can cause discomfort and pain, but not all women have the same side effects. During insertion, you may feel:
- Little pain and some discomfort
- Cramping and pain
- Dizzy or lightheaded
Some women have cramps and backaches for 1 to 2 days after insertion. Other may have cramps and backaches for weeks or months. Over-the-counter pain medicines can ease the discomfort.
Why the Procedure is Performed
IUDs are an excellent choice if you want:
- A long-term and effective birth control method
- To avoid risks and side effects of contraceptive hormones
But you should learn more about IUDs when deciding if you want to get an IUD.
An IUD can prevent pregnancy for 3 to 10 years. Exactly how long the IUD will prevent pregnancy depends on the type of IUD you are using.
IUDs can also be used as an emergency contraception. It must be inserted within 5 days of having unprotected sex.
A newer type of IUD releases a low dose of a hormone into the uterus each day for a period of 3 to 8 years. This increases the effectiveness of the device as a birth control method. It also has the added benefits of reducing or stopping menstrual flow. It may help protect against cancer (endometrial cancer) in women who are at risk for developing the disease.
Risks
While uncommon, IUDs carry some risks, such as:
- There is a small chance of getting pregnant while using an IUD. If you do get pregnant, your provider can remove the IUD to lower the risk for miscarriage or other problems.
- A higher risk of an ectopic pregnancy, but only if you do get pregnant while using an IUD. An ectopic pregnancy is one that occurs outside the womb. It can be serious, even life threatening.
- An IUD may penetrate the uterine wall and require surgery to remove.
Before the Procedure
Talk with your provider about whether an IUD is a good choice for you. Also ask your provider:
- What you can expect during the procedure
- What your risks might be
- What you should watch for after the procedure
For the most part, an IUD can be inserted at any time:
- Right after giving birth
- After an elective or spontaneous miscarriage
If you have an infection in your vagina, cervix or uterus, you should not have an IUD inserted until the infection is cured.
Your provider may advise you to take an over-the-counter painkiller before getting the IUD inserted. If you are sensitive to pain in your vagina or cervix, ask for a local anesthetic to be applied before the procedure starts.
After the Procedure
You may want to have someone drive you home after the procedure. Some women have mild cramping, low backache, and spotting for a couple of days.
If you have a progestin-releasing IUD, it takes about 7 days for it to start to work. You do not need to wait to have sex. But you should use a backup form of birth control, such as a condom, for the first week.
Your provider will want to see you 2 to 4 weeks after the procedure to be sure the IUD is still in place. Ask your provider to show you how to check that the IUD is still in place, and how often you should check it.
In rare cases, an IUD can slip partly or all of the way out of your uterus. This is generally seen after pregnancy. If this happens, contact your provider right away. DO NOT try to remove an IUD that has come part of the way out or has slipped out of place.
Contact your provider right away if you have:
- Flu-like symptoms
- Fever
- Chills
- Cramps
- Pain, bleeding, or fluid leaking from your vagina
Alternative Names
Mirena; Kyleena; Skyla; Liletta; ParaGard; IUS; Intrauterine system; LNG-IUS; Contraception - IUD
Images
References
Bonnema RA. Contraception. In: Kellerman RD, Rakel DP, Heidelbaugh JJ, Lee EM, eds. Conn's Current Therapy 2024. Philadelphia, PA: Elsevier; 2024:1246-1249.
Curtis KM, Nguyen AT, Tepper NK, et al. U.S. Selected Practice Recommendations for Contraceptive Use, 2024. MMWR Recomm Rep. 2024;73(3):1-77. PMID: 39106301 pubmed.ncbi.nlm.nih.gov/39106301/.
Gilner JB, Rhee EHJ, Padro A, Kuller JA. Reproductive genetics. In: Gershenson DM, Lentz GM, Valea FA, Lobo RA, eds. Comprehensive Gynecology. 8th ed. Philadelphia, PA: Elsevier; 2022:chap 2.
Review Date 10/15/2024
Updated by: John D. Jacobson, MD, Professor Emeritus, Department of Obstetrics and Gynecology, Loma Linda University School of Medicine, Loma Linda, CA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.