An autoimmune disease occurs when the body's immune system attacks and destroys healthy body tissue by mistake. There are more than 80 autoimmune diseases.
Causes
The blood cells in the body's immune system help protect against harmful substances. Examples include bacteria, viruses, toxins, cancer cells, and blood and tissue from outside the body. These substances contain antigens. The immune system produces antibodies against these antigens that enable it to destroy these harmful substances.
When you have an autoimmune disease, your immune system does not distinguish between healthy tissue and potentially harmful antigens. As a result, your body sets off a reaction that damages or destroys normal tissues.
The exact cause of autoimmune diseases is unknown. One theory is that some microorganisms (such as bacteria or viruses) or medicines may trigger changes that confuse the immune system. This may happen more often in people who have genes that make them more prone to autoimmune diseases.
An autoimmune disease may result in:
- The destruction of body tissue
- Abnormal growth of an organ
- Changes in organ function
An autoimmune disease may affect one or more organ or tissue types. Areas often affected by autoimmune diseases include:
- Blood vessels
- Connective tissues
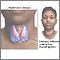
- Endocrine glands such as the thyroid or pancreas
- Joints
- Muscles
- Red blood cells
- Skin
A person may have more than one autoimmune disease at the same time. Common autoimmune diseases include:
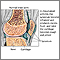
- Addison disease
- Celiac disease - sprue (gluten-sensitive enteropathy)
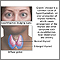
- Dermatomyositis
- Graves disease
- Hashimoto thyroiditis
- Inflammatory bowel disease (Crohn disease, ulcerative colitis)
- Multiple sclerosis
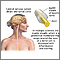
- Myasthenia gravis
- Pernicious anemia
- Reactive arthritis
- Rheumatoid arthritis
- Sjögren syndrome
- Systemic lupus erythematosus (lupus)
- Type I diabetes
Symptoms
Symptoms will vary, based on the type and location of the faulty immune response. Common symptoms include:
Exams and Tests
Your health care provider will do a physical exam. Signs on an exam depend on the type of disease.
Tests that may be done to diagnose an autoimmune disease include:
- Antinuclear antibody (ANA) tests
- Autoantibody tests
- Complete blood count (CBC) with white blood cell differential (CBC with WBC differential)
- Comprehensive metabolic panel
- C-reactive protein (CRP)
- Erythrocyte sedimentation rate (ESR)
- Urinalysis
Treatment
The goals of treatment are to:
- Control the autoimmune process
- Maintain your body's ability to fight disease
- Reduce symptoms
Treatments will depend on your disease and symptoms. Types of treatments include:
- Supplements to replace a substance that the body lacks, such as thyroid hormone, vitamin B12, or insulin, due to the autoimmune disease
- Blood transfusions if blood is affected
- Physical therapy to help with movement if the bones, joints, or muscles are affected
Many people take medicines to reduce the immune system's abnormal response. These are called immunosuppressive medicines. Examples include corticosteroids (such as prednisone) and nonsteroid medicines such as azathioprine, cyclophosphamide, mycophenolate, sirolimus, or tacrolimus. Targeted medicines such as tumor necrosis factor (TNF) blockers and Interleukin inhibitors can be used for some diseases.
Outlook (Prognosis)
The outcome depends on the disease. Most autoimmune diseases are chronic, but many can be controlled with treatment.
Symptoms of autoimmune diseases can come and go. When symptoms get worse, it is called a flare-up.
Possible Complications
Complications depend on the disease. Medicines used to suppress the immune system can cause severe side effects, such as higher risk for infections.
When to Contact a Medical Professional
Contact your provider if you develop symptoms of an autoimmune disease.
Prevention
There is no known prevention for most autoimmune disorders.
References
Abbas AK, Lichtman AH, Pillai S, Henrickson SH. Congenital and acquired immunodeficiencies. In: Abbas AK, Lichtman AH, Pillai S, eds. Cellular and Molecular Immunology. 11th ed. Philadelphia, PA: Elsevier; 2026:chap 21.
Aster JC, Abbas AK, Kumar V, Debnath J, Das A. Diseases of the immune system. In: Aster JC, Abbas AK, Kumar V, Debnath J, Das A, eds. Robbins, Cotran, and Kumar Pathologic Basis of Disease. 11th ed. Philadelphia, PA: Elsevier; 2026:chap 6.
Buckland M, Thaventhiran JE. Immunity. In: Randall D, Booth J, Wiles M, eds. Kumar and Clarke's Clinical Medicine. 11th ed. Philadelphia, PA: Elsevier Limited; 2026:chap 6.
Kono DH, Peterson EJ, Theofilopoulos AN. Immune tolerance and autoimmunity. In: Firestein GS, McInnes IB, Koretzky GA, Mikuls TR, Neogi T, O'Dell JR, eds. Firestein & Kelley's Textbook of Rheumatology. 12th ed. Philadelphia, PA: Elsevier; 2025:chap 21.
Review Date 5/19/2025
Updated by: Jacob Berman, MD, MPH, Clinical Assistant Professor of Medicine, Division of General Internal Medicine, University of Washington School of Medicine, Seattle, WA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.