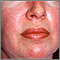
Dermatomyositis is a disease that involves muscle inflammation and a skin rash. Polymyositis is a similar inflammatory condition that also involves muscle weakness, swelling, tenderness, and tissue damage but no skin rash. Both are part of a larger group of diseases called myopathies, more specifically inflammatory myopathies.
Causes
The cause of dermatomyositis is unknown. Experts think it may be due to a viral infection of the muscles or a problem with the body's immune system. It may also occur in people who have cancer in the abdomen, lung, or other parts of the body.
Anyone can develop this condition. It most often occurs in children age 5 to 15 and adults age 40 to 60. It affects women more often than men.
Symptoms
Symptoms may include:
- Muscle weakness, stiffness, or soreness
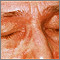
- Purple color to the upper eyelids
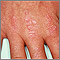
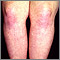
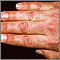
- Purple-red skin rash
- Shortness of breath
- Difficulty swallowing
The muscle weakness may come on suddenly or develop slowly over weeks or months. You may have trouble raising your arms over your head, getting up from a sitting position, and climbing stairs.
The rash may appear on your face, knuckles, neck, shoulders, upper chest, and back.
Exams and Tests
The health care provider will do a physical exam. Tests may include:
- Bloods test to check levels of muscle enzymes called creatine phosphokinase and aldolase
- Blood tests for autoimmune diseases
- Electrocardiogram (ECG)
- Electromyography (EMG)
- Magnetic resonance imaging (MRI)
- Muscle biopsy
- Skin biopsy
- Screening tests for cancer
- Chest x-ray and CT scan of the chest
- Lung function tests
- Swallowing study
- Myositis specific and associated autoantibodies
Treatment
The initial treatment is the use of corticosteroid medicines. The dose of medicine is slowly tapered off as muscle strength improves. This takes about 4 to 6 weeks. You may stay on a low dose of a corticosteroid medicine after that.
Medicines to suppress the immune system may be used to replace the corticosteroids. These medicines may include azathioprine, methotrexate or mycophenolate.
Treatments that may be tried when disease that remains active in spite of these medicines are:
- Intravenous gamma globulin
- Biologic medicines
When your muscles get stronger, your provider may tell you to slowly cut back on your doses. Many people with this condition must take a medicine called prednisone for the rest of their lives.
If a tumor is causing the condition, the muscle weakness and rash may get better when the tumor is removed.
Outlook (Prognosis)
It is important to be followed by a health care provider when you have dermatomyositis. Severe illness can lead to disability and can sometimes result in death.
Symptoms may go away completely in some people, such as children.
The condition may be fatal in adults due to:
- Severe muscle weakness
- Malnutrition
- Pneumonia
- Lung failure
The major causes of death with this condition are cancer and lung disease.
People with lung disease with the anti-MDA-5 antibody have a poor prognosis in spite of current treatment.
Possible Complications
Complications may include:
- Lung disease
- Acute renal failure
- Cancer (malignancy)
- Inflammation of the heart
- Joint pain
When to Contact a Medical Professional
Contact your provider if you have muscle weakness or other symptoms of this condition.
References
Dinulos JGH. Connective tissue diseases. In: Dinulos JGH, ed. Habif's Clinical Dermatology. 7th ed. Philadelphia, PA: Elsevier; 2021:chap 17.
Greenberg SA. Inflammatory myopathies. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 248.
Nagaraju K, Aggarwal R, Lundberg IE. Inflammatory diseases of muscle and other myopathies. In: Firestein GS, McInnes IB, Koretzky GA, Mikuls TR, Neogi T, O'Dell JR, eds. Firestein & Kelley's Textbook of Rheumatology. 12th ed. Philadelphia, PA: Elsevier; 2025:chap 86.
National Organization for Rare Disorders website. Dermatomyositis. rarediseases.org/rare-diseases/dermatomyositis/. Updated May 4, 2018. Accessed February 27, 2025.
Review Date 1/28/2025
Updated by: Diane M. Horowitz, MD, Rheumatology and Internal Medicine, Northwell Health, Great Neck, NY. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.