Aldolase is a protein (called an enzyme) that helps break down certain sugars to produce energy. It is found in high amount in muscle and liver tissue. It is also found in brain tissue.
A test can be done to measure the amount of aldolase in your blood.
How the Test is Performed
A blood sample is needed.
How to Prepare for the Test
You may be told not to eat or drink anything for 6 to 12 hours before the test. You may be also told to avoid vigorous exercise for 12 hours before the test. Your health care provider will tell you if it is necessary to stop taking any medicines that may interfere with this test. Tell your provider about all the medicines you are taking, both prescription and nonprescription.
How the Test will Feel
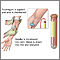
When the needle is inserted to draw blood, some people feel moderate pain. Others feel only a prick or stinging. Afterward, there may be some throbbing or slight bruising. This soon goes away.
Why the Test is Performed
This test is done to diagnose or monitor muscle or liver damage.
Other tests that may be ordered to check for liver damage include:
- Alanine aminotransferase (ALT) test
- Aspartate aminotransferase (AST) test
Other tests that may be ordered to check for muscle cell damage include:
- Creatine phosphokinase (CPK) test
- Lactate dehydrogenase (LDH) test
- Myoglobin test
In some cases of myositis, especially dermatomyositis, the aldolase level may be elevated even when CPK is normal.
Normal Results
Normal results range between 2.5 to 10 units per liter (0.02 to 0.13 microkat/L). There is a slight difference between men and women.
Normal value ranges may vary slightly among different laboratories. Some labs use different measurements or test different samples. Talk to your provider about the meaning of your specific test results.
What Abnormal Results Mean
A higher than normal level may be due to:
- Damage to skeletal muscles
- Heart attack
- Liver, pancreatic, or prostate cancer
- Muscle disease such as dermatomyositis, muscular dystrophy, polymyositis
- Swelling and inflammation of the liver (hepatitis)
- Viral infection called mononucleosis
Risks
There is little risk involved with having your blood taken. Veins and arteries vary in size from one person to another and from one side of the body to the other. Taking blood from some people may be more difficult than from others.
Other risks associated with having blood drawn are slight but may include:
- Excessive bleeding
- Fainting or feeling lightheaded
- Multiple punctures to locate veins
- Hematoma (blood accumulating under the skin)
- Infection (a slight risk any time the skin is broken)
Images
References
Greenberg SA. Inflammatory myopathies. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 248.
Panteghini M. Serum enzymes. In: Rifai N, Chiu RWK, Young I, Burnham Carey-Ann D, Wittwer CT, eds. Tietz Textbook of Laboratory Medicine. 7th ed. St Louis, MO: Elsevier; 2023:chap 32.
Vleugels RA, Jorizzo JL. Dermatomyositis. In: Bolognia JL, Schaffer JV, Cerroni L, eds. Dermatology. 5th ed. Philadelphia, PA: Elsevier; 2025:chap 42.
Review Date 10/9/2025
Updated by: Diane M. Horowitz, MD, Rheumatology and Internal Medicine, Northwell Health, Great Neck, NY. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.