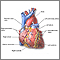
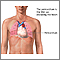
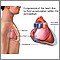
Cardiac tamponade is pressure on the heart that occurs when blood or fluid builds up in the space between the heart muscle and the outer covering sac (pericardium) of the heart.
Causes
In this condition, blood or fluid collects in the sac surrounding the heart. This prevents the heart ventricles from expanding fully. The excess pressure from the fluid prevents the heart from working properly. As a result, the body does not get enough blood.
Cardiac tamponade can occur due to:
- Dissecting aortic aneurysm (thoracic)
- End-stage lung cancer
- Heart attack (acute MI)
- Heart surgery
- Pericarditis caused by bacterial or viral infections
- Wounds to the heart
Other possible causes include:
- Heart tumors
- Underactive thyroid gland
- Kidney failure
- Leukemia
- Placement of central lines
- Radiation therapy to the chest
- Recent invasive heart procedures
- Systemic lupus erythematosus
- Dermatomyositis
- Heart failure
Cardiac tamponade due to disease occurs in about 2 out of 10,000 people.
Symptoms
Symptoms may include:
- Anxiety, restlessness
- Breathing problems
- Sharp chest pain that is felt in the neck, shoulder, back, or abdomen
- Chest pain that gets worse with deep breathing or coughing
- Problems breathing
- Discomfort, sometimes relieved by sitting upright or leaning forward
- Fainting, lightheadedness
- Pale, gray, or blue skin
- Palpitations
- Rapid breathing
- Swelling of the legs or abdomen
- Jaundice
Other symptoms that may occur with this disorder:
- Dizziness
- Drowsiness
- Weak or absent pulse
Exams and Tests
Echocardiogram is the test of choice to help make the diagnosis. This test may be done at the bedside in emergency cases.
A physical exam may show:
- Blood pressure that falls when breathing deeply
- Rapid breathing
- Heart rate over 100 (normal is 60 to 100 beats per minute)
- Heart sounds are only faintly heard through a stethoscope
- Neck veins that may be bulging (distended) but the blood pressure is low
- Weak or absent peripheral pulses
Other tests may include:
- Chest CT or MRI of chest
- Chest x-ray
- Coronary angiography
- ECG
- Right heart catheterization
Treatment
Cardiac tamponade is an emergency condition that needs to be treated in the hospital.
The fluid around the heart must be drained as quickly as possible. A procedure that uses a needle to remove fluid from the tissue that surrounds the heart will be done.
A surgical procedure to cut and remove part of the covering of the heart may also be done. This is known as surgical pericardiectomy or pericardial window.
Fluids are given to keep blood pressure normal until the fluid can be drained from around the heart. Medicines that increase blood pressure may also help keep the person alive until the fluid is drained.
Oxygen may be given to help reduce the workload on the heart by decreasing tissue demands for blood flow.
The cause of tamponade must be found and treated.
Outlook (Prognosis)
Death due to cardiac tamponade can occur quickly if the fluid or blood is not removed promptly from within the pericardium.
The outcome is often good if the condition is treated promptly. However, tamponade may come back.
Possible Complications
Complications may include:
- Heart failure
- Pulmonary edema
- Bleeding
- Shock
- Death
When to Contact a Medical Professional
Go to the emergency room or call the local emergency number (such as 911) if symptoms develop. Cardiac tamponade is an emergency condition that needs immediate medical attention.
Prevention
Many cases can't be prevented. Knowing your personal risk factors may help you get early diagnosis and treatment.
Alternative Names
Tamponade; Pericardial tamponade; Pericarditis - tamponade
References
Hoit BD, Oh JK. Pericardial diseases. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 62.
LeWinter MM, Cremer PC, Klein AL. Pericardial diseases. In: Libby P, Bonow RO, Mann DL, Tomaselli, GF, Bhatt DL, Solomon SD, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine. 12th ed. Philadelphia, PA: Elsevier; 2022:chap 86.
Mallemat HA, Tewelde SZ. Pericardiocentesis. In: Roberts JR, Custalow CB, Thomsen TW, eds. Roberts and Hedges' Clinical Procedures in Emergency Medicine and Acute Care. 7th ed. Philadelphia, PA: Elsevier; 2019:chap 16.
Review Date 5/13/2024
Updated by: Mary C. Mancini, MD, PhD, Cardiothoracic Surgeon, Shreveport, LA. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.