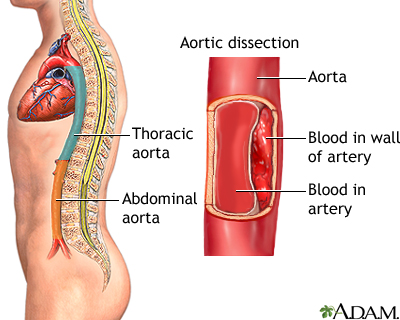
Aortic dissection is a serious condition in which there is a tear in the wall of the major artery carrying blood out of the heart (aorta). As the tear extends along the wall of the aorta, blood can flow in between the layers of the blood vessel wall (dissection). This can lead to aortic rupture or decreased blood flow (ischemia) to organs.
Causes
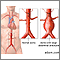
When it leaves the heart, the aorta first moves up through the chest towards the head (the ascending aorta). It then bends or arches, and finally moves down through the chest and abdomen (the descending aorta).
Aortic dissection most often happens because of a tear or damage to the inner wall of the aorta. This very often occurs in the chest (thoracic) part of the artery, but it may also occur in the abdominal aorta.
When a tear occurs, it creates 2 channels:
- One in which blood continues to travel
- Another where blood stays still
If the channel with non-traveling blood gets bigger, it can push on other branches of the aorta. This can narrow the other branches and reduce blood flow through them.
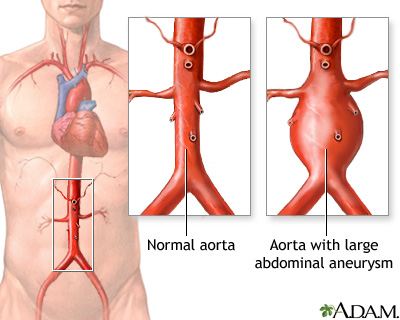
An aortic dissection may also cause abnormal widening or ballooning of the aorta (aneurysm).
The exact cause is unknown, but more common risks include:
- Aging
- Atherosclerosis
- Blunt trauma to the chest, such as hitting the steering wheel of a car during an accident
- High blood pressure
Other risk factors and conditions linked to aortic dissection include:
- Bicuspid aortic valve
- Coarctation (narrowing) of the aorta
- Connective tissue disorders (such as Marfan syndrome and Ehlers-Danlos syndrome) and rare genetic disorders
- Heart surgery or procedures
- Pregnancy
- Swelling of the blood vessels due to conditions such as arteritis and syphilis
Aortic dissection occurs in about 2 out of every 10,000 people. It can affect anyone, but is most often seen in men ages 40 to 70.
Symptoms
In most cases, the symptoms begin suddenly, and include severe chest pain. The pain may feel like a heart attack.
- Pain can be described as sharp, stabbing, tearing, or ripping.
- It is felt below the breast bone, and then moves under the shoulder blades or to the back.
- Pain can move to the shoulder, neck, arm, jaw, abdomen, or hips.
- The pain changes position, often moving to the arms and legs as the aortic dissection gets worse.
Symptoms are caused by a decrease of blood flowing to the rest of the body, and can include:
- Anxiety and a feeling of doom
- Fainting or dizziness
- Heavy sweating (clammy skin)
- Nausea and vomiting
- Pale skin (pallor)
- Rapid, weak pulse
- Shortness of breath and trouble breathing when lying flat (orthopnea)
Other symptoms may include:
- Pain in the abdomen
- Stroke symptoms
- Swallowing difficulties from pressure on the esophagus
Exams and Tests
The health care provider will take your medical and family medical history and listen to your heart, lungs, and abdomen with a stethoscope. The exam may find:
- A "blowing" murmur over the aorta, heart murmur, or other abnormal sound
- A difference in blood pressure between the right and left arms, or between the arms and legs
- Low blood pressure
- Signs resembling a heart attack
- Signs of shock, but with normal blood pressure
Aortic dissection or aortic aneurysm may be seen on:
- Aortic angiography
- Chest x-ray
- Chest MRI
- CT scan of chest with dye
- Duplex Doppler ultrasonography (occasionally performed)
- Echocardiogram
- Transesophageal echocardiogram (TEE)
Blood work to rule out a heart attack is needed.
Treatment
Aortic dissection is a life-threatening condition and needs to be treated right away.
- Dissections that occur in the part of the aorta that is leaving the heart (ascending) are treated with surgery.
- Dissections that occur in other parts of the aorta (descending) may be managed with surgery or medicines.
Two techniques may be used for surgery:
- Standard, open surgery. This requires a surgical incision that is made in the chest or abdomen.
- Endovascular aortic repair. This surgery is done without any major surgical incisions.
Medicines that lower blood pressure may be prescribed. These medicines may be given through a vein (intravenously). Beta-blockers are the medicines of first choice. Strong pain relievers are very often needed.
If the aortic valve is damaged, valve replacement is needed. If the heart arteries are involved, a coronary bypass is also performed.
Outlook (Prognosis)
Aortic dissection is life threatening. The condition can be managed with surgery if it is done before the aorta ruptures. Less than one half of people with a ruptured aorta survive.
Those who survive will need lifelong, aggressive treatment of high blood pressure. They will need to be followed up with CT scans every few months to monitor the aorta.
Possible Complications
Aortic dissection may decrease or stop the blood flow to many different parts of the body. This may result in short-term or long-term problems, or damage to the:
- Brain
- Heart
- Intestines or bowels
- Kidneys
- Legs
When to Contact a Medical Professional
If you have symptoms of an aortic dissection or severe chest pain, call 911 or the local emergency number, or go to the emergency room as quickly as possible.
Prevention
Many cases of aortic dissection cannot be prevented.
Things you can do to reduce your risk include:
- Treating and controlling hardening of the arteries (atherosclerosis)
- Keeping high blood pressure under control, especially if you are at risk for dissection
- Taking safety precautions to prevent injuries that can cause dissections
- If you have been diagnosed with Marfan or Ehlers-Danlos syndrome, making sure you regularly follow-up with your provider
Alternative Names
Aortic aneurysm - dissecting; Chest pain - aortic dissection; Thoracic aortic aneurysm - dissection
References
Beckman JA. Diseases of the aorta. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 63.
Braverman AC, Schermerhorn M. Diseases of the aorta. In: Libby P, Bonow RO, Mann DL, Tomaselli GF, Bhatt DL, Solomon SD, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine. 12th ed. Philadelphia, PA: Elsevier; 2022:chap 43.
Conrad MF. Aortic dissection: epidemiology, pathophysiology, clinical presentation, and medical and surgical management. In: Sidawy AN, Perler BA, eds. Rutherford's Vascular Surgery and Endovascular Therapy. 10th ed. Philadelphia, PA: Elsevier; 2023:chap 83.
Review Date 5/10/2024
Updated by: Neil Grossman, MD, Saint Vincent Radiological Associates, Framingham, MA. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.