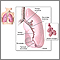
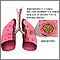
Pulmonary aspergilloma is a mass caused by an infection by the fungus aspergillus. It usually grows in preexisting lung cavities. The infection can also appear in the brain, kidney, or other organs.
Causes
Aspergillosis is an infection caused by the fungus aspergillus. Aspergillomas are formed when the fungus grows in a clump in a lung cavity. The cavity is often created by a previous condition. Cavities in the lung may be caused by diseases such as:
The most common species of fungus that causes disease in humans is Aspergillus fumigatus.
Aspergillus is a common fungus. It grows on dead leaves, stored grain, bird droppings, compost piles, and other decaying vegetation.
Symptoms
You may not have any symptoms. When symptoms do develop, they can include:
- Chest pain
- Cough
- Coughing up blood, which can be a life-threatening sign
- Fatigue
- Fever
- Unintentional weight loss
Exams and Tests
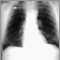
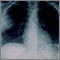
Your health care provider may suspect you have a fungal infection after x-rays of your lungs show the ball of fungus. Other tests that may be done include:
- Biopsy of lung tissue
- Blood test for presence of aspergillus in the body (galactomannan)
- Blood test to detect immune response to aspergillus (aspergillus precipitin)
- Bronchoscopy or bronchoscopy with lavage
- Chest CT
- Sputum culture
Treatment
Many people never develop symptoms. Often, no treatment is needed, unless you are coughing up blood.
Sometimes, antifungal medicines may be used.
If you have bleeding in the lungs, your provider may recommend a test to inject dye into the blood vessels (angiography) to find the site of bleeding. The bleeding is stopped by either:
- Surgery to remove the aspergilloma
- A procedure that inserts material into the blood vessels to stop the bleeding (embolization)
Outlook (Prognosis)
The outcome can be good for many people. However, it depends on the severity of the condition and your overall health.
Surgery may be very successful in some cases, but it is complex and can have a high risk of serious complications.
Possible Complications
Complications of pulmonary aspergilloma may include:
- Difficulty breathing that gets worse
- Massive bleeding from the lung
- Spread of the infection
When to Contact a Medical Professional
Contact your provider if you cough up blood, and be sure to mention any other symptoms that have developed.
Prevention
People who have had related lung infections or who have weakened immune systems should try to avoid environments where the aspergillus fungus is found.
Alternative Names
Fungus ball; Mycetoma; Aspergilloma; Aspergillosis - pulmonary aspergilloma
References
Patterson TF, Thompson GR 3rd, Denning DW, et al. Practice guidelines for the diagnosis and management of aspergillosis: 2016 update by the Infectious Diseases Society of America. Clin Infect Dis. 2016;63(4):e1-e60. PMID: 27365388 pubmed.ncbi.nlm.nih.gov/27365388/.
Saullo JL, Alexander BD. Fungal infections: opportunistic. In: Broaddus VC, Ernst JD, King TE, et al, eds. Murray and Nadel's Textbook of Respiratory Medicine. 7th ed. Philadelphia, PA: Elsevier; 2022:chap 57.
Walsh TJ, Patterson TF. Aspergillosis. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 311.
Review Date 8/29/2024
Updated by: Jatin M. Vyas, MD, PhD, Roy and Diana Vagelos Professor in Medicine, Columbia University Vagelos College of Physicians and Surgeons, Division of Infectious Diseases, Department of Medicine, New York, NY. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.