Sarcoidosis is a disease in which inflammation occurs in the lymph nodes, lungs, liver, eyes, skin, and other tissues.
Causes
The exact cause of sarcoidosis is unknown. What is known is that when a person has the disease, tiny clumps of abnormal tissue (granulomas) form in certain organs of the body. Granulomas are clusters of immune cells and are a type of inflammation.
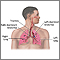
The disease can affect almost any organ. It most commonly affects the lungs.
Health experts think that having certain genes makes it more likely for a person to develop sarcoidosis. Things that may trigger the disease include infections with bacteria or viruses. Contact with dust or chemicals may also be triggers.
The disease is more common in African Americans and White people of Scandinavian heritage. More women than men have the disease.
The disease often begins between ages 20 and 40. Sarcoidosis is rare in young children.
A person with a close blood relative who has sarcoidosis is nearly 5 times as likely to develop the condition.
Symptoms
There may be no symptoms. When symptoms do occur, they can involve almost any body part or organ system.
Almost all people affected by sarcoidosis have lung or chest symptoms:
- Chest pain (most often behind the breast bone)
- Dry cough
- Shortness of breath
- Coughing up blood (rare, but serious)
Symptoms of general discomfort may include:
- Fatigue
- Fever
- Joint ache or pain (arthralgia)
- Weight loss
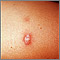
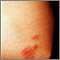
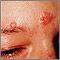
Skin symptoms may include:
- Hair loss
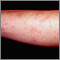
- Raised, red, firm skin sores (erythema nodosum), almost always on the front part of the lower legs
- Rash
- Scars that become raised or inflamed
Nervous system symptoms may include:
Eye symptoms may include:
Other symptoms of this disease may include:
- Dry mouth
- Fainting spells, if the heart is involved
- Nosebleed
- Swelling in the upper part of the abdomen
- Liver disease
- Swelling of the legs if heart and lungs are involved
- Abnormal heart rhythm if the heart is involved
Exams and Tests
Your health care provider will perform a physical exam and ask about the symptoms.
Different imaging tests may help diagnose sarcoidosis:
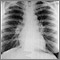
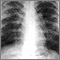
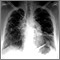
- Chest x-ray to see if the lungs are involved or lymph nodes are enlarged
- CT scan of the chest
- Lung gallium scan (rarely done now)
- Imaging tests of the brain and liver
- PET scan of the whole body (or specific body parts)
- Echocardiogram or MRI of the heart
To diagnose this condition, a biopsy is often needed. A biopsy of the lung using bronchoscopy sometimes with an ultrasound to enable a biopsy of a lymph node in or near the lung is done. Biopsies of other body tissues may also be done.
The following lab tests may be done:
- Calcium levels (urine, blood)
- CBC
- Immunoelectrophoresis
- Liver function tests
- Quantitative immunoglobulins
- Phosphorus (blood)
- Angiotensin converting enzyme (ACE)
Treatment
Sarcoidosis symptoms will often get better without treatment, especially if there are only small lung abnormalities.
If the eyes, heart, nervous system, or lungs are affected, corticosteroids are usually prescribed. This medicine may need to be taken for 1 to 2 years.
Medicines that suppress the immune system are sometimes also needed.
In rare cases, people with very severe heart or lung damage (end-stage disease) may need an organ transplant.
With sarcoidosis that affects the heart, an implantable cardioverter-defibrillator (ICD) may be needed to treat heart rhythm problems.
Outlook (Prognosis)
Many people with sarcoidosis are not seriously ill, and get better without treatment. Up to half of all people with the disease get better in 3 years without treatment. People whose lungs are affected may develop lung damage.
Overall the death rate from sarcoidosis is less than 5%. Causes of death include:
- Bleeding from the lung tissue
- Heart damage, leading to heart failure and abnormal heart rhythms
- Lung scarring (pulmonary fibrosis)
Possible Complications
Sarcoidosis may lead to these health problems:
- Fungal lung infections (aspergillosis)
- Glaucoma and blindness from uveitis (rare)
- Kidney stones from high calcium levels in the urine
- Osteoporosis and other complications of taking corticosteroids for long periods of time
- High blood pressure in the arteries of the lungs (pulmonary hypertension)
When to Contact a Medical Professional
Contact your provider promptly if you have:
- Vision changes
- Other symptoms of this disorder
Patient Instructions
References
Crouser ED, Maier LA, Wilson KC, et al. Diagnosis and detection of sarcoidosis. an official American Thoracic Society clinical practice guideline. Am J Respir Crit Care Med. 2020;201(8):e26-e51. PMID: 32293205 pubmed.ncbi.nlm.nih.gov/32293205/.
Iannuzzi MC. Sarcoidosis. Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 83.
Judson MA, Koth LL, Baughman RP. Sarcoidosis. In: Broaddus VC, Ernst JD, King TE, et al, eds. Murray & Nadel's Textbook of Respiratory Medicine. 7th ed. Philadelphia, PA: Elsevier; 2022:chap 93.
Review Date 4/10/2025
Updated by: Allen J. Blaivas, DO, Division of Pulmonary, Critical Care, and Sleep Medicine, VA New Jersey Health Care System, Clinical Assistant Professor, Rutgers New Jersey Medical School, East Orange, NJ. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.