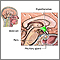
Hypothalamic dysfunction is a problem with part of the brain called the hypothalamus. The hypothalamus helps control the pituitary gland and thus regulates many body functions.
Causes
The hypothalamus helps keep the body's internal functions in balance. It helps regulate:
- Appetite and weight
- Body temperature
- Childbirth
- Emotions, behavior, memory
- Growth
- Production of breast milk
- Salt and water balance
- Sex drive
- Sleep-wake cycle and the body clock
Another important function of the hypothalamus is to control the pituitary gland. The pituitary is a small gland at the base of the brain. It lies just below the hypothalamus. The pituitary, in turn, controls the:
- Adrenal glands
- Ovaries
- Testes
- Thyroid gland
There are many causes of hypothalamic dysfunction. The most common are:
- Surgery
- Brain injury
- Brain tumors
- Radiation treatment to the brain
Other causes include:
- Nutrition problems, such as eating disorders (anorexia), extreme weight loss
- Blood vessel problems in the brain, such as aneurysm, pituitary apoplexy, subarachnoid hemorrhage
- Genetic disorders, such as Prader-Willi syndrome, familial diabetes insipidus, Kallmann syndrome
- Infections and swelling (inflammation) due to certain immune system diseases
Symptoms
Symptoms are usually due to the hormones or brain signals that are missing. In children, there may be growth problems, either too much or too little growth. In other children, puberty occurs too early or too late.
Tumor symptoms may include headache or loss of vision.
If the thyroid is affected, there may be symptoms of an underactive thyroid (hypothyroidism). Symptoms may include feeling cold all the time, constipation, fatigue, or weight gain, among others.
If the adrenal glands are affected, there may be symptoms of low adrenal function. Symptoms may include fatigue, weakness, poor appetite, weight loss, and lack of interest in activities.
Exams and Tests
Your health care provider will perform a physical examination and ask about your symptoms.
Blood or urine tests may be ordered to determine levels of hormones or chemicals such as:
- Cortisol
- Estrogen
- Growth hormone
- Osmolality
- Pituitary hormones
- Prolactin
- Sodium
- Testosterone
- Thyroid
Other possible tests include:
- Hormone injections followed by timed blood samples
- MRI or CT scans of the brain
- Visual field eye exam (if there is a tumor)
Treatment
The treatment depends on the cause of the hypothalamic dysfunction:
- For tumors, surgery or radiation may be needed.
- For hormonal deficiencies, missing hormones need to be replaced by taking medicine. This is effective for pituitary problems and for salt and water balance.
- Medicines are usually not effective for changes in temperature or sleep regulation, though melatonin does have effects on the hypothalamus.
- Some medicines may help with problems related to appetite regulation and weight gain.
Outlook (Prognosis)
Many causes of hypothalamic dysfunction are treatable or reversible. Most of the time, missing hormones can be replaced.
Possible Complications
Complications of hypothalamic dysfunction depend on the cause.
BRAIN TUMORS
- Permanent blindness
- Problems related to the brain area where the tumor occurs
- Vision disorders
- Problems regulating salt and water balance
HYPOTHYROIDISM
- Heart problems
- High blood cholesterol
ADRENAL INSUFFICIENCY
- Inability to deal with stress (such as surgery or infection), which can be life threatening by causing low blood pressure
SEX GLAND DEFICIENCY
- Heart disease
- Erection problems
- Infertility
- Thin bones (osteoporosis)
- Problems breast feeding
- Problems with uterine contractions during delivery
GROWTH HORMONE DEFICIENCY
- High blood cholesterol
- Osteoporosis
- Short stature (in children)
- Weakness
When to Contact a Medical Professional
Contact your provider if you have:
- Headaches
- Symptoms of hormone excess or deficiency
- Vision problems
Prevention
If you have symptoms of a hormonal deficiency, discuss replacement therapy with your provider.
Alternative Names
Hypothalamic syndromes
Images
References
Christian HC. Anatomy and physiology of the hypothalamus and pituitary. In: Robertson RP, ed. DeGroot's Endocrinology. 8th ed. Philadelphia, PA: Elsevier; 2023:chap 13.
Hafida S, Apovian CM. Obesity and neuroendocrine control of energy stores. In: Melmed S, Auchus RJ, Goldfine AB, Rosen CJ, Kopp PA, eds. Williams Textbook of Endocrinology. 15th ed. Philadelphia, PA: Elsevier; 2025:chap 40.
Weiss RE. Neuroendocrinology and the neuroendocrine system. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 204.
Review Date 4/24/2025
Updated by: Sandeep K. Dhaliwal, MD, board-certified in Diabetes, Endocrinology, and Metabolism, Springfield, VA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.