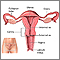
Ovarian cancer is cancer that starts in the ovaries. The ovaries are the female reproductive organs that produce eggs.
Causes
Ovarian cancer is the fifth most common cancer among women. It causes more deaths than any other type of female reproductive organ cancer.
The cause of ovarian cancer is unknown.
Risks of developing ovarian cancer include any of the following:
- The fewer children a woman has and the later in life she gives birth, the higher her risk for ovarian cancer.
- Women who have had breast cancer or have a family history of breast or ovarian cancer have an increased risk for ovarian cancer (due to variants in genes such as BRCA1 or BRCA2).
- Women who take estrogen replacement only (not with progesterone) for 5 years or more may have a higher risk for ovarian cancer. Birth control pills, though, decrease the risk for ovarian cancer.
- Fertility treatment with medicines probably does not increase the risk for ovarian cancer.
- In vitro fertilization (IVF) may increase the risk of borderline or low malignant potential ovarian tumors.
- Older women are at the highest risk of developing ovarian cancer. Most deaths from ovarian cancer occur in women age 65 to 74.
Symptoms
Ovarian cancer symptoms are often vague. Women and their health care providers often blame the symptoms on other, more common conditions. Sometimes, by the time the cancer is diagnosed, the tumor has spread beyond the ovaries.
See your provider if you have the following symptoms on a daily basis for more than a few weeks:
- Bloating or swelling in the belly area
- Difficulty eating or feeling full quickly (early satiety)
- Pelvic or lower abdominal pain (area may feel heavy)
- Back pain
- Swollen lymph nodes in groin
Other symptoms that can occur:
- Excessive hair growth that is coarse and dark
- Sudden urge to urinate
- Needing to urinate more often than usual (urinary frequency or urgency)
- Constipation
Exams and Tests
A physical exam may often be normal. With advanced ovarian cancer, your provider may find a swollen abdomen often due to accumulation of fluid (ascites).
A pelvic exam may reveal an ovarian or abdominal mass.
A CA-125 blood test is not considered a good screening test for ovarian cancer. But, it may be done if a woman has:
- Symptoms of ovarian cancer
- Already been diagnosed with ovarian cancer to determine how well treatment is working
Other tests that may be done include:
- Complete blood count and blood chemistry
- Pregnancy test (serum HCG)
- CT, positron emission tomography (PET) scan, or MRI of the pelvis or abdomen
- Ultrasound of the pelvis
Surgery, such as laparoscopy or exploratory laparotomy, may be required to find the cause of symptoms. A biopsy will be done to help make the diagnosis.
No lab or imaging test has ever been shown to be able to successfully screen for or diagnose ovarian cancer in its early stages, so no standard screening tests are recommended at this time.
Treatment
Surgery is used to treat virtually all stages of ovarian cancer. For early stages, surgery may be the only treatment needed. Surgery may involve removing both ovaries and fallopian tubes, the uterus, or other structures in the belly or pelvis. The goals of surgery for ovarian cancer are:
- Sample normal appearing areas to see if the cancer has spread (staging)
- Remove any areas of tumor spread (debulking)
Chemotherapy is used after surgery to treat any cancer that remains. Chemotherapy can also be used if the cancer comes back (relapses). Chemotherapy is typically given intravenously (through an IV). It can also be injected directly into the abdominal cavity (intraperitoneal, or IP).
Radiation therapy is rarely used to treat ovarian cancer.
After surgery and chemotherapy, follow instructions about how often you should see your oncologist and the tests you should have.
Support Groups
You can ease the stress of illness by joining a cancer support group. Sharing with others who have common experiences and problems can help you not feel alone.
Outlook (Prognosis)
Ovarian cancer is rarely diagnosed in its early stages. It is usually quite advanced by the time diagnosis is made:
- Nearly one half of women live longer than 5 years after diagnosis
- If the diagnosis is made early in the disease and treatment is received before the cancer spreads outside the ovary, the 5-year survival rate is high
When to Contact a Medical Professional
Make an appointment with your provider if you have symptoms of ovarian cancer. Experts differ on the effectiveness of routine pelvic exams for finding early stage ovarian cancer.
Prevention
There are no standard recommendations for screening women without symptoms (asymptomatic) for ovarian cancer. Pelvic ultrasound or a blood test, such as CA-125, have not been found to be effective and are not recommended.
Genetic testing for the BRCA1 or BRCA2, or other cancer-related genes, may be recommended for women at high risk for ovarian cancer. These are women who have a personal or family history of breast or ovarian cancer or have other family members with these genetic changes.
Removing the ovaries and fallopian tubes and possibly the uterus in women who have a proven mutation in the BRCA1 or BRCA2 gene may reduce the risk of developing ovarian cancer. But, ovarian cancer may still develop in other areas of the pelvis.
Alternative Names
Cancer - ovaries
References
Coleman RL, Liu J, Matsuo K, Thaker PH, Westin SN, Sood AK. Carcinoma of the ovaries and fallopian tubes. In: Niederhuber JE, Armitage JO, Kastan MB, Doroshow JH, Tepper JE, eds. Abeloff's Clinical Oncology. 6th ed. Philadelphia, PA: Elsevier; 2020:chap 86.
Coleman RL, Westin SN, Ramirez PT, Salvo G, Gershenson DM. Malignant diseases of the ovary, fallopian tube, and peritoneum. In: Lobo RA, Gershenson DM, Lentz GM, Valea FA, eds. Comprehensive Gynecology. 8th ed. Philadelphia, PA: Elsevier; 2022:chap 33.
National Cancer Institute website. BRCA gene changes: cancer risk and genetic testing. www.cancer.gov/about-cancer/causes-prevention/genetics/brca-fact-sheet. Updated July 19, 2024. Accessed October 16, 2024.
Review Date 10/8/2024
Updated by: Howard Goodman, MD, Gynecologic Oncology, Florida Cancer Specialists & Research Institute, West Palm Beach, FL. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.