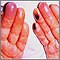
Cryoglobulinemia is the presence of abnormal proteins in the blood. These proteins thicken in cold temperatures.
Causes
Cryoglobulins are antibodies. It is not yet known why they become solid or gel-like at low temperatures in the laboratory. In the body, these antibodies can form immune complexes that can cause inflammation and block blood vessels. This is called cryoglobulinemic vasculitis. This may lead to problems ranging from skin rashes to kidney failure.
Cryoglobulinemia is part of a group of diseases that cause damage and inflammation of the blood vessels throughout the body (vasculitis). There are three main types of this condition. They are grouped based on the type of antibody that is produced:
- Type I
- Type II
- Type III
Type I cryoglobulinemia is most often related to cancer of the blood or immune systems.
Types II and III are also referred to as mixed cryoglobulinemia.
Types II and III are most often found in people who have a long-lasting (chronic) inflammatory condition, such as an autoimmune disease or hepatitis C. Most people with the type II form of cryoglobulinemia have a chronic hepatitis C infection.
Other conditions that may be related to cryoglobulinemia include:
- Leukemia
- Multiple myeloma
- Primary macroglobulinemia
- Rheumatoid arthritis
- Systemic lupus erythematosus
Symptoms
Symptoms will vary, depending on the type of disorder you have and the organs that are involved. Symptoms may include:
- Breathing problems
- Fatigue
- Glomerulonephritis (kidney inflammation)
- Joint pain
- Muscle pain
- Purpura
- Raynaud phenomenon
- Skin death
- Skin ulcers
Exams and Tests
The health care provider will do a physical exam. You will be checked for signs of liver and spleen swelling.
Tests for cryoglobulinemia include:
- Complete blood count (CBC).
- Complement assay -- complement levels will be low.
- Cryoglobulin test -- may show presence of cryoglobulins. (This is a complicated laboratory procedure that involves many steps. It is important that the lab that performs the test is familiar with the process.)
- Liver function tests -- may be high if hepatitis C is present.
- Rheumatoid factor -- positive in types II and III.
- Skin biopsy -- may show inflammation in blood vessels, vasculitis.
- Protein electrophoresis - blood -- may show an abnormal antibody protein.
- Urinalysis -- may show blood in the urine if the kidneys are affected.
- Hepatitis B and hepatitis C testing.
Other tests may include:
- Angiogram
- Chest x-ray
- ESR
- Hepatitis C test
- Nerve conduction tests, if the person has numbness or weakness in the arms or legs
Treatment
MIXED CRYOGLOBULINEMIA (TYPES II AND III)
Mild or moderate forms of cryoglobulinemia can often be treated by taking steps to deal with the underlying cause.
Current direct-acting medicines for hepatitis C eliminate the virus in nearly all people. As hepatitis C goes away, the cryoglobulins will disappear in about one half of all people over the next 12 months. Your provider will continue to monitor the cryoglobulins after treatment.
Severe cryoglobulinemia vasculitis involves vital organs or large areas of skin. It is treated with corticosteroids and other medicines that suppress the immune system.
- Rituximab is an effective drug and has fewer risks than other medicines.
- Cyclophosphamide is used in life-threatening conditions where rituximab is not working or available. This medicine was used more often in the past.
- A treatment called plasmapheresis is also used. In this procedure, blood plasma is taken out of blood circulation and abnormal cryoglobulin antibody proteins are removed. The plasma is replaced by fluid, protein, or donated plasma.
TYPE I CRYOGLOBULINEMIA
This disorder is due to a cancer of the blood or immune system such as multiple myeloma. Treatment is directed against the abnormal cancer cells that produce the cryoglobulin.
Outlook (Prognosis)
Most of the time, mixed cryoglobulinemia does not lead to death. Outlook can be poor if the kidneys are affected.
Possible Complications
Complications include:
- Bleeding in the digestive tract (rare)
- Heart disease (rare)
- Skin infections or ulcers
- Kidney failure
- Liver failure
- Skin death
- Death
When to Contact a Medical Professional
Contact your provider if:
- You develop symptoms of cryoglobulinemia.
- You have hepatitis C and develop symptoms of cryoglobulinemia.
- You have cryoglobulinemia and develop new or worsening symptoms.
Prevention
There is no known prevention for the condition.
- Staying away from cold temperatures may prevent some symptoms.
- Testing and treatment for hepatitis C infection will reduce your risk.
References
De Vita S, Gandolfo S, Quartuccio L. Cryoglobulinemia. In: Hochberg MC, Gravallese EM, Smolen JS, van der Heijde D, Weinblatt ME, Weisman MH, eds. Rheumatology. 8th ed. Philadelphia, PA: Elsevier; 2023:chap 171.
McPherson RA, Riley RS, Massey HD. Laboratory evaluation of immunoglobulin function and humoral immunity. In: McPherson RA, Pincus MR, eds. Henry's Clinical Diagnosis and Management by Laboratory Methods. 24th ed. Philadelphia, PA: Elsevier; 2022:chap 47.
Rajkumar SV. Plasma cell disorders. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 173.
Stone JH. Immune complex-mediated small-vessel vasculitis. In: Firestein GS, McInnes IB, Koretzky GA, Mikuls TR, Neogi T, O'Dell JR, eds. Firestein & Kelley's Textbook of Rheumatology. 12th ed. Philadelphia, PA: Elsevier; 2025:chap 92.
Review Date 1/28/2025
Updated by: Diane M. Horowitz, MD, Rheumatology and Internal Medicine, Northwell Health, Great Neck, NY. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.