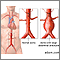
Open abdominal aortic aneurysm (AAA) repair is surgery to fix a widened part in your aorta. This is called an aneurysm. The aorta is the large artery that carries blood from your heart to your belly (abdomen), pelvis, and legs.
An aortic aneurysm is when part of this artery becomes too large or balloons outward.
Description
The surgery will take place in an operating room. You will be given general anesthesia (you will be asleep and pain-free).
Your surgeon opens up your belly and replaces the aortic aneurysm with a man-made, cloth-like material.
Here is how it can be done:
- In one approach, you will lie on your back. The surgeon will make a cut in the middle of your belly, from just below the breastbone to below the belly button. Rarely, the cut goes across the belly.
- In another approach, you will lie slightly tilted on your right side. The surgeon will make a 5- to 6-inch (13 to 15 centimeters) cut from the left side of your belly, ending a little below your belly button.
- Your surgeon will replace the aneurysm with a long tube made of man-made (synthetic) cloth. It is sewn in with stitches.
- In some cases, the ends of this tube (or graft) will be moved through blood vessels in each groin and attached to those in the leg.
- Once the surgery is done, your legs will be examined to make sure that there is a pulse. Most often a dye test using x-rays is done to confirm that there is good blood flow to the legs.
- The cut is closed with sutures or staples.
Surgery for aortic aneurysm replacement may take 2 to 4 hours. Most people recover in the intensive care unit (ICU) after the surgery.
Why the Procedure is Performed
Open surgery to repair an AAA is sometimes done as an emergency procedure when there is bleeding inside your body from the aneurysm.
You may have an AAA that is not causing any symptoms or problems. Your health care provider may have found the problem by examining you or after you had an ultrasound or CT scan done for another reason. There is a risk that this aneurysm may suddenly break open (rupture) if you do not have surgery to repair it. However, surgery to repair the aneurysm may also be risky, depending on your overall health.
You and your provider must decide whether the risk of having this surgery is smaller than the risk for rupture. Surgery is more likely to be suggested if the aneurysm is:
- Larger (about 2 inches or 5 centimeters)
- Growing more quickly (a little less than 1/4 inch over the last 6 to 12 months)
Risks
The risks for this surgery are higher if you have:
- Heart disease
- Kidney failure
- Lung disease
- Past stroke
- Other serious medical problems
Complications are also higher for older people.
Risks for any surgery are:
- Blood clots in the legs that may travel to the lungs
- Breathing problems
- Heart attack or stroke
- Infection, including in the lungs (pneumonia), urinary tract, and belly
- Reactions to medicines
Risks for this surgery are:
- Bleeding before or after surgery
- Damage to a nerve, causing pain or numbness in the leg
- Damage to your intestines or other nearby organs
- Loss of blood supply to a portion of the large intestine causing delayed bleeding in the stool
- Infection of the graft
- Injury to the ureter, the tube that carries urine from your kidneys to your bladder
- Kidney failure that may be permanent
- Problems getting or keeping an erection
- Poor blood supply to your legs, your kidneys, or other organs
- Spinal cord injury
- Wound breaks open
- Wound infections
- Death
Before the Procedure
Your will have a physical exam and get tests before you have surgery.
Always tell your provider what medicines you are taking, even medicines, supplements, or herbs you bought without a prescription.
If you are a smoker, you should stop smoking at least 4 weeks before your surgery. Your provider can help.
During the 2 weeks before your surgery:
You will have visits with your provider to make sure medical problems such as diabetes, high blood pressure, and heart or lung problems are well regulated.
- You may be asked to stop taking medicines that make it harder for your blood to clot. These include aspirin, ibuprofen (Advil, Motrin), clopidogrel (Plavix), naproxen (Aleve, Naprosyn), and other medicines like these.
- Ask which medicines you should still take on the day of your surgery.
- Always tell your surgeon if you have a cold, flu, fever, herpes breakout, or other illness before your surgery.
DO NOT drink anything after midnight the day before your surgery, including water.
On the day of your surgery:
- Take the medicines you were told to take with a small sip of water.
- You will be told when to arrive at the hospital.
After the Procedure
Most people stay in the hospital for 5 to 10 days. During a hospital stay, you will:
- Be in the intensive care unit (ICU), where you will be monitored very closely right after surgery. You may need a breathing machine (ventilator) during the first day.
- Have a urinary catheter.
- Have a tube that goes through your nose into your stomach to help drain fluids for 1 or 2 days. You will then slowly begin drinking, then eating.
- Receive medicine to keep your blood thin.
- Be encouraged to sit on the side of the bed and then walk.
- Wear special stockings to prevent blood clots in your legs.
- Be asked to use a breathing machine called an incentive spirometer to help clear your lungs.
- Receive pain medicine into your veins or into the space that surrounds your spinal cord (epidural).
Outlook (Prognosis)
Full recovery for open surgery to repair an aortic aneurysm may take 2 or 3 months. Most people make a full recovery from this surgery.
Most people who have an aneurysm repaired before it breaks open (ruptures) have a good outlook.
Alternative Names
AAA - open; Repair - aortic aneurysm - open
Patient Instructions
Images
References
Braverman AC, Schemerhorn M. Diseases of the aorta. In: Libby P, Bonow RO, Mann DL, Tomaselli GF, Bhatt DL, Solomon SD, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine. 12th ed. Philadelphia, PA: Elsevier; 2022:chap 42.
Sharafuddin MJ. Abdominal aortic aneurysms: open surgical treatment. In: Sidawy AN, Perler BA, eds. Rutherford's Vascular Surgery and Endovascular Therapy. 10th ed. Philadelphia, PA: Elsevier; 2023:chap 73.
Review Date 10/23/2024
Updated by: Deepak Sudheendra, MD, MHCI, RPVI, FSIR, Founder and CEO, 360 Vascular Institute, with an expertise in Vascular Interventional Radiology & Surgical Critical Care, Columbus, OH. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.