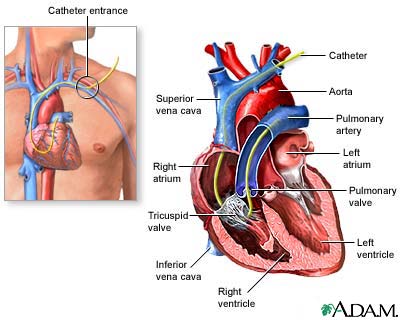
Swan-Ganz catheterization (also called right heart catheterization or pulmonary artery catheterization) is the passing of a thin tube (catheter) into the right side of the heart and the arteries leading to the lungs. It is done to monitor the heart's function and blood flow and pressures in and around the heart.
How the Test is Performed
The test can be done while you are in bed in an intensive care unit (ICU) of a hospital. It can also be done in special procedure areas such as a cardiac catheterization laboratory.
Before the test starts, you may be given medicine (sedative) to help you relax.
You will lie on a padded table. Your doctor (most often a heart specialist called a cardiologist) will make a puncture into a vein near the groin or in your arm, or neck. A flexible tube (catheter or sheath) is placed through the puncture. Sometimes, it will be placed in your leg or your arm. You will be awake during the procedure.
A longer catheter is inserted. It is then carefully moved into the upper chamber of the right side of the heart. X-ray images may be used to help the health care provider see where the catheter should be placed.
Blood may be removed from the catheter. This blood is tested to measure the amount of oxygen in the blood.
During the procedure, your heart's rhythm will be constantly watched using an electrocardiogram (ECG).
How to Prepare for the Test
You should not eat or drink anything for 8 hours before the test starts (your cardiologist may give you different directions).
You may need to stay in the hospital the night before the test. Otherwise, you will check in to the hospital the morning of the test. In some cases, this procedure may be done after you have already been admitted to the hospital, possibly on an emergency basis.
You will wear a hospital gown. You must sign a consent form before the test. Your cardiologist will explain the procedure and its risks.
How the Test will Feel
You may be given medicine to help you relax before the procedure. You will be awake and able to follow instructions during the test.
You may feel some discomfort when the IV is placed into your arm. You may also feel some pressure at the site when the catheter is inserted. In people who are critically ill, the catheter may stay in place for several days.
You may feel discomfort when the area of the vein is numbed with anesthetic.
Why the Test is Performed
The procedure is done to evaluate how the blood moves (circulates) in people who have:
- Abnormal pressures in the heart arteries
- Burns
- Congenital heart disease
- Heart failure
- Kidney disease
- Leaky heart valves
- Lung problems
- Shock (very low blood pressure)
It may also be done to monitor for complications of a heart attack or heart surgery. It also shows how well certain heart medicines are working.
Swan-Ganz catheterization can also be used to detect abnormal blood flow between two areas of the heart that are not normally connected.
Conditions that can also be diagnosed or evaluated with Swan-Ganz catheterization include:
- Cardiac tamponade
- Congenital heart disease
- Pulmonary hypertension
- Restrictive or dilated cardiomyopathy
Normal Results
Normal results for this test are:
- Cardiac index is 2.8 to 4.2 liters per minute per square meter (of body surface area)
- Pulmonary artery systolic pressure is 17 to 32 millimeters of mercury (mm Hg)
- Pulmonary artery mean pressure is 9 to 19 mm Hg
- Pulmonary diastolic pressure is 4 to 13 mm Hg
- Pulmonary capillary wedge pressure is 4 to 12 mm Hg
- Right atrial pressure is 0 to 7 mm Hg
What Abnormal Results Mean
Abnormal results may be due to:
- Blood flow problems, such as heart failure or shock
- Heart valve disease
- Lung disease
- Structural problems with the heart, such as a shunt from an atrial or ventricular septal defect
Risks
Risks of the procedure include:
- Bruising around the area where the catheter was inserted
- Injury to the vein
- Puncture to the lung if the neck or chest veins are used, causing lung collapse (pneumothorax)
Very rare complications include:
- Cardiac arrhythmias requiring treatment
- Embolism caused by blood clots at the tip of the catheter
- Infection
- Low blood pressure
Alternative Names
Right heart catheterization; Catheterization - right heart
Images
References
Kern MJ, Seto AH, Hermann J. Invasive hemodynamic diagnosis of cardiac disease. In: Libby P, Bonow RO, Mann DL, Tomaselli GF, Bhatt DL, Solomon SD, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine. 12th ed. Philadelphia, PA: Elsevier; 2022:chap 22.
Kapur NK, Sorajja P. Invasive hemodynamics. In: Sorajja P, Lim MJ, Kern MJ, eds. Kern's Cardiac Catheterization Handbook. 7th ed. Philadelphia, PA: Elsevier; 2020:chap 4.
Shreenivas SS, Lilly SM, Herrmann HC. Interventions in cardiogenic shock. In: Topol EJ, Teirstein PS, eds. Textbook of Interventional Cardiology. 8th ed. Philadelphia, PA: Elsevier; 2020:chap 22.
Review Date 7/14/2024
Updated by: Michael A. Chen, MD, PhD, Associate Professor of Medicine, Division of Cardiology, Harborview Medical Center, University of Washington Medical School, Seattle, WA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.