Complement component 4 is a blood test that measures the activity of a certain protein. This protein is part of the complement system. The complement system is a group of nearly 60 proteins that are found in the blood plasma or on the surface of some cells.
The proteins work with your immune system and play a role in protecting from infection. They also help to remove dead cells and foreign material from the body. Rarely, people may inherit deficiency of one or more complement proteins. These people are prone to certain infections or autoimmune disorders.
There are nine major complement proteins. They are labeled C1 through C9. This article describes the test that measures C4.
How the Test is Performed
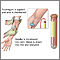
Blood is drawn from a vein. A vein from the inside of the elbow or the back of the hand is most often used.
The procedure is as follows:
- The site is cleaned with an antiseptic.
- The health care provider wraps an elastic band around the upper arm to apply pressure to the area and make the vein swell with blood.
- The provider gently inserts a needle into the vein.
- The blood collects into an airtight vial or tube attached to the needle. The elastic band is removed from your arm.
- Once the blood has been collected, the needle is removed. The puncture site is covered to stop any bleeding.
In infants or young children, a sharp tool called a lancet may be used to puncture the skin and make it bleed. The blood collects into a small glass tube called a pipette, or onto a slide or test strip. A bandage may be placed over the area if there is any bleeding.
How to Prepare for the Test
No special preparation is needed.
How the Test will Feel
When the needle is inserted to draw blood, some people feel moderate pain. Others may feel only a prick or stinging sensation. Afterward, there may be some throbbing.
Why the Test is Performed
C3 and C4 are the most commonly measured complement components. When the complement system is turned on during inflammation, levels of complement proteins may go down. Complement activity may be measured to determine how severe a disease is or if treatment is working.
A complement test may be used to monitor people with an autoimmune disorder. For example, people with active systemic lupus erythematosus may have lower-than-normal levels of the complement proteins C3 and C4.
Complement activity varies throughout the body. In people with rheumatoid arthritis, complement activity may be normal or higher-than-normal in the blood, but much lower-than-normal in the joint fluid.
Normal Results
The normal range for C4 is 15 to 45 milligrams per deciliter (mg/dL) (0.15 to 0.45 g/L).
Normal value ranges may vary slightly among different laboratories. Talk to your provider about the meaning of your specific test results.
The examples above show the common measurements for results for these tests. Some laboratories use different measurements or may test different specimens.
What Abnormal Results Mean
Increased complement activity may be seen in:
Decreased complement activity may be seen in:
- Bacterial infections (especially Neisseria)
- Cirrhosis
- Glomerulonephritis
- Hepatitis
- Hereditary angioedema
- Kidney transplant rejection
- Lupus nephritis
- Malnutrition
- Systemic lupus erythematosus
- Rare inherited complement deficiencies
- Systemic vasculitis
Alternative Names
C4
Images
References
Atkinson JP, Holers VM. Complement system in disease. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 37.
Bean KV, Massey HD, Gupta G. Mediators of inflammation: complement. In: McPherson RA, Pincus MR, eds. Henry's Clinical Diagnosis and Management by Laboratory Methods. 24th ed. Philadelphia, PA: Elsevier; 2022:chap 48.
Ram S. Complement and deficiencies. In: Bennett JE, Dolin R, Blaser MJ, eds. Mandell, Douglas, and Bennett's Principles and Practice of Infectious Diseases. 9th ed. Philadelphia, PA: Elsevier; 2020:chap 9.
Sullivan KE, Grumach AS. The complement system. In: Burks AW, Holgate ST, O'Hehir RE, et al, eds. Middleton's Allergy: Principles and Practice. 9th ed. Philadelphia, PA: Elsevier; 2020:chap 8.
Review Date 1/28/2025
Updated by: Diane M. Horowitz, MD, Rheumatology and Internal Medicine, Northwell Health, Great Neck, NY. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.