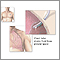
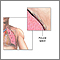
A chest tube is a hollow, flexible tube placed into the chest. It acts as a drain.
- Chest tubes drain blood, fluid, or air from around your lungs, heart, or esophagus.
- The tube is placed between your ribs and into the space between the lungs and the wall of your chest cavity. This is called the pleural space. Suction is applied through the tube, removing fluid or air. This allows your lungs to fully expand.
Description
When your chest tube is inserted, you will lie on your side or sit partly upright, with one arm over your head.
- Sometimes, you will receive medicine through a vein (intravenous, or IV) to make you relaxed and sleepy.
- Your skin will be cleaned at the site of the planned insertion.
- You will be given local anesthesia (numbing medicine to reduce pain) at and around the place where the chest tube will be.
- The chest tube is inserted through a small cut in your skin between your ribs. Then it is guided to the correct spot.
- The tube is connected to a special canister. Suction is often used to help it drain. Other times, gravity alone will allow it to drain.
- A stitch (suture) and tape keep the tube in place.
After your chest tube insertion, you will have a chest x-ray to make sure the tube is in the right place.
The chest tube most often stays in place until x-rays show that all the blood, fluid, or air has drained from your chest and your lung has fully re-expanded.
The tube is easy to remove when it is no longer needed.
Some people may have a chest tube inserted that is guided by x-ray, computerized tomography (CT), or ultrasound. If you have major lung or heart surgery, a chest tube will be placed while you are under general anesthesia (asleep) during your surgery.
Why the Procedure is Performed
Chest tubes are used to treat conditions that cause a lung to collapse. Some of these conditions are:
- Surgery or trauma to the chest
- Air leaks from inside the lung into the chest (pneumothorax)
- Fluid buildup in the chest (called a pleural effusion) due to bleeding into the chest, buildup of fatty fluid, abscess or pus buildup in the lung or the chest, or heart failure
- A tear in the esophagus (the tube that allows food to go from the mouth to the stomach)
Risks
Some risks from the insertion procedure are:
- Bleeding or infection where the tube is inserted
- Improper placement of the tube (into the tissues, abdomen, or too far in the chest)
- Injury to the lung or heart
- Injury to organs near the tube, such as the spleen, liver, stomach, or diaphragm
After the Procedure
You will most likely stay in the hospital until your chest tube is removed. In some cases, a person may go home with a chest tube.
While the chest tube is in place, your health care provider will carefully check for air leaks, breathing problems, and if you need oxygen. They will also make sure the tube stays in place. Your provider will tell you whether it is OK to get up and walk around or sit in a chair.
What you will need to do:
- Breathe deeply and cough often (your nurse will teach you how to do this). Deep breathing and coughing will help re-expand your lung and help with drainage.
- Be careful there are no kinks in your tube. The drainage system should always sit upright and be placed below your lungs. If it is not, the fluid or air will not drain and your lungs can't re-expand.
Get help right away if:
- Your chest tube comes out or shifts position.
- The tubes become disconnected.
- You suddenly have a harder time breathing or have more pain.
Outlook (Prognosis)
The outlook depends on the reason a chest tube is inserted. Pneumothorax most often improves, but sometimes surgery is needed to correct the underlying problem. This may be performed through a scope or may require a large incision depending on your underlying condition. In cases of infection, the person improves when the infection is treated, although scarring of the lining of the lung can sometimes occur (fibrothorax). This may require surgery to correct the problem.
Alternative Names
Chest drainage tube insertion; Insertion of tube into chest; Tube thoracostomy; Pericardial drain
References
Boujaoude Z, Shersher D. Chest tube thoracostomy. In: Parrillo JE, Dellinger RP, eds. Critical Care Medicine: Principles of Diagnosis and Management in the Adult. 5th ed. Philadelphia, PA: Elsevier; 2019:chap 15.
Margolis AM, Kirsch TD. Tube thoracostomy. In: Roberts JR, Custalow CB, Thomsen TW, eds. Roberts and Hedges' Clinical Procedures in Emergency Medicine and Acute Care. 7th ed. Philadelphia, PA: Elsevier; 2019:chap 10.
Watson GA, Harbrecht BG. Chest tube placement, care, and removal. In: Vincent J-L, Moore FA, Bellomo R, Marini JJ, eds. Textbook of Critical Care. 8th ed. Philadelphia, PA: Elsevier; 2024:chap E12.
Review Date 4/1/2025
Updated by: John Meilahn, MD, General Surgeon, Wyndmoor, PA. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.