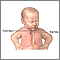
Tracheoesophageal fistula and esophageal atresia repair is a surgery to repair two coexisting birth defects in the esophagus and trachea. The defects usually occur together.
Description
The esophagus is the tube that carries food from the mouth to the stomach. The trachea (windpipe) is the tube that carries air into and out of the lungs.
The defects usually occur together. They may occur along with other problems as part of a syndrome (group of problems):
- Esophageal atresia (EA) occurs when the upper part of the esophagus does not connect with the lower esophagus and stomach.
- Tracheoesophageal fistula (TEF) is an abnormal connection between the upper part of the esophagus and the trachea or windpipe.
This surgery is almost always done soon after birth. Both defects can often be repaired at the same time. Briefly, the surgery takes place this way:
- Medicine (anesthesia) is given so that the baby is in a deep sleep and pain-free during surgery.
- The surgeon makes a cut on the side of the chest between the ribs.
- The fistula between the esophagus and windpipe is closed.
- The upper and lower portions of the esophagus are sewn together if possible.
Often the two parts of the esophagus are too far apart to sew together right away. In this case:
- Only the fistula is repaired during the first surgery.
- A gastrostomy tube (G-tube), a tube that goes through the skin into the stomach, may be placed to give your child nutrition.
- Your child will have another surgery later to repair the esophagus.
Sometimes the surgeon will wait 2 to 4 months before doing the surgery. Waiting allows your baby to grow or have other problems treated. If your child's surgery is delayed:
- A G-tube will be placed through the abdominal wall into the stomach. Numbing medicines (local anesthesia) will be used so that your baby does not feel pain.
- At the same time the tube is placed, the surgeon may lengthen your baby's esophagus with special techniques. This will make the future surgery easier. This process may need to be repeated, sometimes several times, before repair is possible.
Why the Procedure is Performed
Tracheoesophageal fistula and esophageal atresia are life-threatening problems. They need to be treated right away. If these problems are not treated:
- Your child may breathe saliva and fluids from the stomach into the lungs. This is called aspiration. It can cause choking and pneumonia (lung infection).
- Your child cannot swallow and digest at all if the esophagus does not connect to the stomach.
Risks
Risks of anesthesia and surgery in general include:
- Reactions to medicines
- Breathing problems
- Bleeding, blood clots, or infection
Risks of this surgery include:
- Collapsed lung (pneumothorax)
- Food leakage from the area that is repaired
- Low body temperature (hypothermia)
- Narrowing of the repaired organs
- Reopening of the fistula
Before the Procedure
Your baby will be admitted to the neonatal intensive care unit (NICU) as soon as the doctors diagnose either of these problems.
Your baby will receive nutrition by vein may also be on a breathing machine (ventilator). The care team may use suction to keep fluids from going into the lungs.
Some infants who are premature, have a low birth weight, or have other birth defects beside TEF and EA may not be able to have surgery until they grow larger or until other problems have been treated or have gone away.
After the Procedure
After surgery, your child will be cared for in the hospital's NICU.
Additional treatments after surgery usually include:
- Antibiotics as needed, to prevent infection
- Breathing machine (ventilator)
- Chest tube (a tube through the skin into the chest wall) to drain air and fluids from the space between the outside of the lung and the inside of the chest cavity
- IV fluids, including nutrition
- Oxygen
- Pain medicines as needed
If both the TEF and EA are repaired:
- A tube is placed through the nose into the stomach (nasogastric tube) during the surgery.
- Feedings are usually started through this tube a few days after surgery.
- Feedings by mouth are started slowly. Your baby may need feeding therapy.
If only the TEF is repaired, a G-tube is used for feedings until the atresia can be repaired. Your baby may also need continuous or frequent suction to clear secretions from the upper esophagus.
While your baby is in the hospital, the care team will show you how to use and replace the G-tube. You may also be sent home with an extra G-tube. The hospital staff will inform a home health supply company of your equipment needs.
How long your infant stays in the hospital depends on the type of defect your child has and whether there are other problems in addition to the TEF and EA. You will be able to bring your baby home once they are taking feedings by mouth or G-tube, gaining weight, and safely breathing on their own.
Outlook (Prognosis)
Surgery can usually repair a TEF and EA. Once healing from the surgery is complete, your child may have these problems:
- The part of the esophagus that was repaired may become narrower. Your child may need to have more surgery to treat this.
- Your child may have heartburn, or gastroesophageal reflux disease (GERD). This occurs when acid from the stomach goes up into the esophagus. GERD may cause breathing problems.
During infancy and early childhood, many children will have problems with breathing, growth, and feeding, and will need to continue seeing both their primary care provider and specialists.
Babies with TEF and EA who also have defects of other organs, most commonly the heart, may have long-term health problems.
Alternative Names
TEF repair; Esophageal atresia repair
Patient Instructions
References
Callaway JP. Anatomy, histology, embryology, and developmental anomalies of the esophagus. In: Chung RT, Rubin DT, Wilcox CM, eds. Sleisenger and Fordtran's Gastrointestinal and Liver Disease. 12th ed. Philadelphia, PA: Elsevier; 2026:chap 45.
Dingeldein M. Selected gastrointestinal anomalies in the neonate. In: Martin RJ, Fanaroff AA, eds. Fanaroff and Martin's Neonatal-Perinatal Medicine: Diseases of the Fetus and Infant. 12th ed. Philadelphia, PA: Elsevier; 2025:chap 88.
Rothenberg SS. Esophageal atresia and tracheoesophageal fistula malformations. In: Holcomb GW, Murphy JP, St. Peter SD, eds. Holcomb and Ashcraft's Pediatric Surgery. 7th ed. Philadelphia, PA: Elsevier; 2020:chap 27.
Review Date 10/3/2025
Updated by: Mary Terrell, MD, NABBLM-C, IBCLC, Neonatologist, Cape Fear Valley Medical Center, Fayetteville, NC. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.