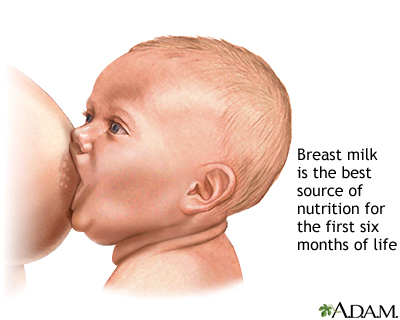
Health experts agree that breastfeeding is the healthiest option for both mom and baby. They recommend that babies feed only on breast milk for the first 6 months, and then continue to have breast milk as a main part of their diet until they are at least 1 to 2 years old.
It is true that breastfeeding is not always easy for moms and babies. It can take some time for you both to get the hang of it. It is important to know this up front, so that you can make sure you have all the support and commitment you need if a problem does come up.
Recommendations
Breastfeeding (nursing) your baby can be a good experience for both the mother and the baby. It takes time and practice to get comfortable with breastfeeding. Things you can do to help the process include:
- Start breastfeeding your baby in the hospital, right after birth.
- Ask for help from a lactation consultant or nurse to get you started.
- Read about breastfeeding before your baby is born.
NIPPLE SORENESS
Most women are able to breastfeed with no pain. Sometimes, breast tenderness and nipple soreness will occur in the first week. Getting help with a proper latch right away from a breastfeeding support person can help this go away more quickly.
Nipple soreness may be caused by many things, including:
- Poor feeding techniques
- Wrong position of the baby when breastfeeding
- Not taking care of your nipples
For many women, there is no clear cause of nipple soreness. A simple change in your baby's position while feeding may ease soreness.
You might have sore nipples if your baby keeps sucking as they come off the breast. You can help your baby learn to let go by gently inserting a finger into the side of the mouth to break the suction.
Skin that is too dry or too moist can also cause nipple soreness.
- Bras made from man-made (synthetic) fabrics may cause moisture to collect. These fabrics may increase sweating and slow evaporation.
- Using soaps or solutions that remove natural skin oils can cause dry skin. Olive oil, expressed milk, and ointments containing lanolin can help soothe dry or cracking nipples.
Some babies chew or bite on the nipples when they start teething.
- Giving your baby something cold and wet to chew on a few minutes before breastfeeding can help avoid this problem. A clean, wet washcloth from the refrigerator works well.
- Offer your baby another cold, wet washcloth before feeding on the other breast.
BREAST ENGORGEMENT OR BREAST FULLNESS
Breast fullness is the slow buildup of blood and milk in the breast a few days after birth. It is a sign that your milk is coming in. It will not prevent you from breastfeeding.
Breast engorgement is caused by back up in the blood vessels in the breast. The breasts are swollen, hard, and painful. The nipples may not stick out enough to allow the baby to latch on correctly.
The let-down reflex is a normal part of breastfeeding. Milk made in the milk glands is released into the milk ducts. Pain, stress, and anxiety can interfere with the reflex. As a result, milk will build up. Treatment includes:
- Learning to relax and finding a comfortable position
- Reducing distractions during nursing, performing a gentle massage, and applying heat to the breast
Nursing often (8 times or more in 24 hours) and for at least 15 minutes at each feeding can also prevent engorgement.
Other ways to relieve breast engorgement:
- Feed more often or express milk manually or with a pump. Electric breast pumps work best.
- Alternate between taking warm showers and using cold compresses to help ease the discomfort.
NOT ENOUGH MILK FOR THE BABY'S NEEDS
Almost all women can produce enough milk for their babies. Though many women are very worried about this, it is quite rare that a mother will produce too little milk.
Making too little milk can happen for a few reasons, including using infant formula to feed your baby in addition to breastfeeding. If you are worried about how your baby is growing, you should talk with your baby's health care provider right away before starting to supplement with formula.
The mother's supply is based on the baby's demand for milk. Frequent feedings, adequate rest, good nutrition, and drinking enough fluids can help maintain a good milk supply.
PLUGGED MILK DUCT
A milk duct can become plugged. This may happen if the baby does not feed well, if the mother skips feedings (common when the child is weaning), or if the mother's bra is too tight. Symptoms of a plugged milk duct include:
- Tenderness
- Heat and redness in one area of the breast
- A lump that can be felt close to the skin
Sometimes, a tiny white dot can be seen at the opening of the duct on the nipple. Massaging the area and putting gentle pressure on it can help to remove the plug.
A breast infection (mastitis) causes aching muscles, fever, and a red, hot, tender area on one breast. Contact your provider if you develop these symptoms.
Treatment often includes:
- Taking antibiotics for the infection
- Applying moist, warm compresses to the infected area
- Getting rest
- Wearing a comfortable bra between feedings
Continuing to nurse from the infected breast will help healing take place. Breast milk is safe for your baby, even when you have a breast infection. This will prevent further breast engorgement.
If nursing is too uncomfortable, you may try pumping or manual expression to move milk out of the breast. You can try offering the unaffected breast first until let-down occurs, to prevent discomfort. Talk to your provider about ways to manage the problem.
THRUSH
Thrush is a common yeast infection that can be passed between the mother and the baby during breastfeeding. The yeast (Candida albicans) thrives in warm, moist areas.
The baby's mouth and the mother's nipples are good places for this yeast to grow. Yeast infections often occur during or after antibiotic treatments.
Symptoms of yeast infection in the mother are deep-pink nipples that are tender or uncomfortable during, and right after, nursing. White patches and increased redness in your baby's mouth are symptoms of a yeast infection.
Your baby may also have a diaper rash, a change in mood, and will want to suckle more frequently. Contact your provider to get advice about an antifungal medicine for affected members of your family.
ILLNESS
If you develop a fever or illness, contact your provider. You can safely continue breastfeeding during most illnesses. Your baby is likely to benefit from your antibodies.
Alternative Names
Plugged milk ducts; Nipple soreness when breastfeeding; Breastfeeding - overcoming problems; Let-down reflex
Images
References
Barrett KJ, Gilley SP, Haemer MA, Krebs NF, Johnson SL. Feeding healthy infants, children, and adolescents. In: Kliegman RM, St. Geme JW, Blum NJ, et al, eds. Nelson Textbook of Pediatrics. 22nd ed. Philadelphia, PA: Elsevier; 2025:chap 61.
Gontasz MM, Keiser AM, Aucott SW. Care of the newborn. In: Gleason CA, Sawyer T, eds. Avery's Diseases of the Newborn. 11th ed. Philadelphia, PA: Elsevier; 2024:chap 16.
Meek JY, Noble L. Policy statement: Breastfeeding and the use of human milk. Pediatrics. 2022;150(1):e2022057988. PMID: 35921640 pubmed.ncbi.nlm.nih.gov/35921640/.
Newton ER. Lactation and breastfeeding. In: Landon MB, Galan HL, Jauniaux ERM, et al, eds. Gabbe's Obstetrics Essentials: Normal and Problem Pregnancies. Philadelphia, PA: Elsevier; 2019:chap 24.
Rosen-Carole C, Stuebe AM. Practical management of the nursing "dyad". In: Lawrence RA, Lawrence RM, eds. Breastfeeding: A Guide for the Medical Profession. 9th ed. Philadelphia, PA: Elsevier; 2022:chap 7.
Review Date 7/1/2025
Updated by: Neil K. Kaneshiro, MD, MHA, Clinical Professor of Pediatrics, University of Washington School of Medicine, Seattle, WA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.