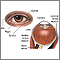
The optic nerve carries images of what the eye sees to the brain. When this nerve becomes swollen or inflamed, it is called optic neuritis. It may cause sudden, reduced vision in the affected eye.
Causes
The exact cause of optic neuritis is unknown.
The optic nerve carries visual information from your eye to the brain. The nerve can swell when it becomes inflamed. The swelling can damage nerve fibers. This can cause short or long-term loss of vision.
Conditions that have been linked with optic neuritis include:
- Autoimmune diseases, including lupus, sarcoidosis, and Behcet disease
- Cryptococcosis, a fungal infection
- Bacterial infections, including tuberculosis, syphilis, Lyme disease, and meningitis
- Viral infections, including viral encephalitis, measles, rubella, chickenpox, herpes zoster, mumps, and mononucleosis
- Respiratory infections, including mycoplasma pneumonia and other common upper respiratory tract infections
- Multiple sclerosis
Symptoms
Symptoms may include:
- Loss of vision in one eye over an hour or a few hours
- Changes in the way the pupil reacts to bright light
- Loss of color vision
- Pain when you move your eye
Exams and Tests
A complete medical exam can help check for related diseases. Tests may include:
- Color vision testing
- MRI of the brain, including special images of the optic nerve
- Visual acuity testing
- Visual field testing
- Examination of the optic disc using indirect ophthalmoscopy
Treatment
Vision often returns to normal within 2 to 3 weeks with no treatment.
Corticosteroids given through a vein (IV) or taken by mouth (oral) may speed up recovery. However, the final vision is no better with steroids than without. Oral steroids may actually increase the chance of recurrence.
If tests suggest that there is also multiple sclerosis, other types of treatment may be helpful.
Further tests may be needed to try to find the cause of the neuritis. If there is a condition causing the problem, it may be treated.
Ongoing research is underway to explore treatments that can help protect the optic nerve and promote recovery in the case of a recurrence.
Outlook (Prognosis)
When optic neuritis occurs without other diseases, the prognosis is better. An MRI is an important test because it can help predict if multiple sclerosis or other similar autoimmune diseases are present or may develop.
Optic neuritis caused by multiple sclerosis or other autoimmune diseases has a poorer outlook. However, vision in the affected eye may still return to normal.
Possible Complications
Complications may include:
- Body-wide side effects from corticosteroids
- Vision loss
Some people who have an episode of optic neuritis will develop nerve problems in other places in the body or develop multiple sclerosis.
When to Contact a Medical Professional
Contact your health care provider right away if you have a sudden loss of vision in one eye, especially if you have eye pain.
If you have been diagnosed with optic neuritis, contact your provider if:
- Your vision decreases.
- The pain in the eye gets worse.
- Your symptoms do not improve within 2 to 3 weeks.
Alternative Names
Retro-bulbar neuritis; Multiple sclerosis - optic neuritis; Optic nerve - optic neuritis
Patient Instructions
References
Calabresi PA. Multiple sclerosis and demyelinating conditions. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 380.
Chaitanuwong P, Moss HE. Optic neuritis: a comprehensive review of current therapies and emerging treatment strategies. Front Neurol. 2025;16:1605075. PMID: 40606143 pubmed.ncbi.nlm.nih.gov/40606143/.
Kuchlin S, Ihorst G, Heinrich SP, et al. Clinical predictors in acute optic neuritis: analysis based on clinical trial data. Ophthalmology. 2025;132(6):631-643. PMID: 39827907 pubmed.ncbi.nlm.nih.gov/39827907/.
Moss HE, Balcer LJ. Inflammatory optic neuropathies and neuroretinitis. In: Yanoff M, Duker JS, eds. Ophthalmology. 6th ed. Philadelphia, PA: Elsevier; 2023:chap 9.7.
Thurtell MJ, Prasad S, Tomsak RL. Neuro-ophthalmology: afferent visual system. In: Jankovic J, Mazziotta JC, Pomeroy SL, Newman NJ, eds. Bradley and Daroff's Neurology in Clinical Practice. 8th ed. Philadelphia, PA: Elsevier; 2022:chap 16.
Review Date 1/27/2026
Updated by: Franklin W. Lusby, MD, Ophthalmologist, Lusby Vision Institute, La Jolla, CA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.