Syphilis is a bacterial infection that is most often spread through sexual contact.
Causes
Syphilis is a sexually transmitted infection (STI) caused by the bacterium Treponema pallidum. This bacterium causes infection when it gets into broken skin or mucus membranes, usually of the genitals. Syphilis is most often transmitted through sexual contact, although it also can be transmitted in other ways.
Syphilis occurs worldwide, most commonly in urban areas. The number of cases is rising fastest in men who have sex with men (MSM). Young adults ages 20 to 35 are the highest-risk population. Because people may be unaware that they are infected with syphilis, many states require tests for syphilis before marriage. All pregnant women who receive prenatal care should be screened for syphilis to prevent the infection from passing to their newborn (congenital syphilis). Also, people at increased risk for getting syphilis should be screened for it.
Syphilis has three stages:
- Primary syphilis
- Secondary syphilis
- Tertiary syphilis (the late phase of the illness)
Secondary syphilis, tertiary syphilis, and congenital syphilis are not seen as often in the United States because of education, screening, and treatment.
Symptoms
The incubation period for primary syphilis is 14 to 21 days. Symptoms of primary syphilis are:
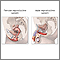
- Small, painless open sore or ulcer (called a chancre) on the genitals, mouth, skin, or rectum that heals by itself in 3 to 6 weeks
- Enlarged lymph nodes in the area of the sore
The bacteria continue to grow in the body, but there are few symptoms until the second stage.
The symptoms of secondary syphilis start 4 to 8 weeks after the primary syphilis. The symptoms may include:
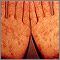
- Skin rash, usually on the palms of the hands and soles of the feet
- Sores called mucous patches in or around the mouth, vagina, or penis
- Moist, warty patches (called condylomata lata) on the genitals or in skin folds
- Fever
- General ill feeling (malaise)
- Loss of appetite
- Muscle and joint pain
- Swollen lymph nodes
- Vision changes
- Hair loss
Primary and secondary syphilis usually resolve without treatment. At that point, syphilis becomes latent and may have no symptoms for many years. But, during this time, it may be damaging organs leading to tertiary syphilis.
Tertiary syphilis develops in untreated people. The symptoms depend on which organs have been affected. They vary widely and can be difficult to diagnose. Symptoms include:
- Damage to the heart, causing aneurysms or valve disease
- Central nervous system disorders (neurosyphilis)
- Masses of dead, inflamed tissue in the skin, bones, or liver (gummas)
Exams and Tests
Your health care provider will perform a physical exam and ask about the symptoms. Tests that may be done include:
- Examination of fluid from sore (rarely done)
- Echocardiogram, aortic angiogram, and cardiac catheterization to look at the major blood vessels and the heart
- Spinal tap and examination of spinal fluid
- Blood tests to screen for syphilis bacteria (RPR, VDRL, or TRUST)
If the RPR, VDRL, or TRUST tests are positive, additional tests will be done to confirm the diagnosis:
Treatment
Syphilis can be treated with antibiotics, such as:
- Penicillin G benzathine
- Doxycycline (a type of tetracycline given to people who are allergic to penicillin)
The length of treatment depends on how severe the syphilis is, and factors such as the person's overall health.
To treat syphilis during pregnancy, penicillin is the medicine of choice. Tetracycline cannot be used for treatment because it is dangerous to the unborn baby. Erythromycin may not prevent congenital syphilis in the baby. People who are allergic to penicillin should ideally be desensitized to it, and then treated with penicillin.
Several hours after getting treatment for the early stages of syphilis, people may experience the Jarisch-Herxheimer reaction. This process is caused by an immune reaction to the breakdown products of the infection and not an allergic reaction to the antibiotic.
Symptoms and signs of this reaction include:
- Chills
- Fever
- General ill feeling (malaise)
- Headache
- Muscle and joint pain
- Nausea
- Rash
These symptoms usually disappear within 24 hours.
Follow-up blood tests must be done at 3, 6, 12, and 24 months to ensure that the infection is gone. Avoid sexual contact when the chancre is present. Use condoms until two follow-up tests have shown that the infection has been cured, to reduce the chance of transmitting the infection.
All sexual partners of the person with syphilis should also be treated. Syphilis can spread very easily in the primary and secondary stages.
Outlook (Prognosis)
Primary and secondary syphilis can be cured if it is diagnosed early and completely treated.
Although secondary syphilis usually goes away within weeks, in some cases it may last for up to 1 year. Without treatment, up to one-third of people will have late complications of syphilis.
Tertiary syphilis may be permanently disabling, and it may lead to death.
Possible Complications
Complications of syphilis may include:
- Cardiovascular problems (aortitis and aneurysms)
- Destructive sores of skin and bones (gummas)
- Neurosyphilis
- Syphilitic myelopathy - a complication that involves muscle weakness and abnormal sensations
- Syphilitic meningitis
In addition, untreated secondary syphilis during pregnancy may spread the disease to the developing baby. This is called congenital syphilis.
When to Contact a Medical Professional
Contact your provider for an appointment if you have symptoms of syphilis.
Also contact your provider or get screened at an STI clinic if you have:
- Had intimate contact with a person who has syphilis or any other STI
- Engaged in any high-risk sexual practices, including having multiple or unknown partners or using intravenous drugs
Prevention
If you are sexually active, practice safer sex and always use a condom.
All pregnant women should be screened for syphilis. Also, people at increased risk for getting syphilis should be screened for it. Common examples include men who have sex with men, people with HIV infection, young adults, and people with a history of incarceration, sex work, military service or illicit drug use.
Alternative Names
Primary syphilis; Secondary syphilis; Late syphilis; Tertiary syphilis; Treponema - syphilis; Lues; Sexually transmitted disease - syphilis; Sexually transmitted infection - syphilis; STD - syphilis; STI - syphilis
References
Dionne JA, Ghanem KG. Syphilis. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 295.
Radolf JD, Tramont EC, Salazar JC. Syphilis (Treponema pallidum). In: Bennett JE, Dolin R, Blaser MJ, eds. Mandell, Douglas, and Bennett's Principles and Practice of Infectious Diseases. 9th ed. Philadelphia, PA: Elsevier; 2020:chap 237.
Stary G, Stary A. Sexually transmitted infections. In: Bolognia JL, Schaffer JV, Cerroni L, eds. Dermatology. 5th ed. Philadelphia, PA: Elsevier; 2025:chap 82.
US Preventive Services Task Force website. Syphilis infection in nonpregnant adolescents and adults: Screening. www.uspreventiveservicestaskforce.org/uspstf/announcements/final-recommendation-statement-screening-syphilis-infection-nonpregnant-adolescents-and-adults. Updated September 27, 2022. Accessed November 9, 2024.
Review Date 8/29/2024
Updated by: Jatin M. Vyas, MD, PhD, Roy and Diana Vagelos Professor in Medicine, Columbia University Vagelos College of Physicians and Surgeons, Division of Infectious Diseases, Department of Medicine, New York, NY. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.