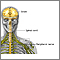
Peripheral nerves carry information to and from the brain. They also carry signals in both directions between the spinal cord and the rest of the body.
Peripheral neuropathy means these nerves don't work properly. Peripheral neuropathy may occur because of damage to a single nerve or a group of nerves. It may also affect nerves in the whole body.
Causes
Neuropathy is very common. There are many types and causes. Often, no cause can be found. Some nerve diseases run in families.
Diabetes is the most common cause of this type of nerve problem. High blood sugar levels over a long time can damage your nerves.
Other health conditions that may cause neuropathy are:
- Autoimmune disorders, such as rheumatoid arthritis or lupus
- Chronic kidney disease
- Infections such as HIV/AIDS, shingles, and hepatitis C
- Low levels of vitamin B1, B6, B12, or other vitamins
- Metabolic disease
- Poisoning due to heavy metals, such as lead
- Poor blood flow to the legs
- Underactive thyroid gland
- Bone marrow disorders
- Tumors
- Certain inherited disorders
Other things that can lead to nerve damage are:
- Trauma or pressure on a nerve
- Long-term, heavy alcohol use
- Glue, lead, mercury, and solvent poisoning
- Medicines that treat infections, cancer, seizures, and high blood pressure
- Pressure on a nerve, such as from carpal tunnel syndrome
- Being exposed to cold temperatures for a long period of time
- Pressure from bad-fitting casts, splints, a brace, or crutches
Symptoms
Symptoms depend on which nerve is damaged, and whether the damage affects one nerve, several nerves, or the whole body.
PAIN AND NUMBNESS
Tingling or burning in the arms and legs may be an early sign of nerve damage. These feelings often start in your toes and feet. You may have deep pain. This often happens in the feet and legs.
You may lose feeling in your legs and arms. Because of this, you may not notice when you step on something sharp. You may not notice when you touch something that is too hot or cold, like the water in a bathtub. You may not know when you have a small blister or sore on your feet.
Numbness may make it harder to tell where your feet are moving and can cause a loss of balance.
MUSCLE PROBLEMS
Damage to the nerves can make it harder to control muscles. It can also cause weakness. You may notice problems moving a part of your body. You may fall because your legs buckle. You may trip over your toes.
Doing tasks such as buttoning a shirt may be harder. You may also notice that your muscles twitch or cramp. Your muscles may become smaller.
PROBLEMS WITH BODY ORGANS
People with nerve damage may have problems digesting food. You may feel full or bloated and have heartburn after eating only a little food. Sometimes, you may vomit food that has not been digested well. You may have either loose stools or hard stools. Some people have problems swallowing.
Damage to the nerves to your heart may cause you to feel lightheaded, or faint, when you stand up.
Angina is the warning chest pain for some heart diseases and heart attack. Nerve damage may hide this warning sign. You should learn other warning signs of a heart attack. They are sudden fatigue, sweating, shortness of breath, nausea, and vomiting.
OTHER SYMPTOMS OF NERVE DAMAGE
- Sexual problems. Men may have problems with erections. Women may have trouble with vaginal dryness or orgasm.
- Some people may not be able to tell when their blood sugar gets too low.
- Bladder problems. You may leak urine. You may not be able to tell when your bladder is full. Some people are not able to empty their bladder.
- You may sweat too little or too much. This may cause problems controlling your body temperature.
Exams and Tests
Your health care provider will examine you and ask about your health history and symptoms.
Blood and urine tests may be done to look for causes of nerve damage.
Your provider may also recommend:
- Electromyography -- to check electrical activity in muscles
- Nerve conduction studies -- to see how fast signals travel along nerves
- Nerve biopsy -- to look at a sample of a nerve under a microscope
- Skin biopsy -- to see if there are a normal number of nerve endings in the skin
- Genetic testing -- to test for conditions that run in families
- Spinal tap (lumbar puncture) -- to analyze spinal fluid (CSF) for inflammation or infection
Treatment
Treating the cause of nerve damage, if known, may improve your symptoms.
People with diabetes should learn to control their blood sugar.
If you use alcohol, stop.
Your medicines may need to be changed. Do not stop taking any medicine before talking to your provider.
Replacing a vitamin or making other changes in your diet may help. If you have low levels of B12 or other vitamins, your provider may recommend supplements or injections.
You may need treatments that suppress your immune system if the neuropathy is due to an autoimmune disorder.
You may need surgery to remove pressure from a nerve.
You may need genetic counseling if the condition could be passed on to your children.
You may have therapy to learn exercises to improve muscle strength and control. Wheelchairs, braces, and splints may improve movement or the ability to use an arm or leg that has nerve damage.
Physical therapy may help with balance issues and falling due to neuropathy.
SETTING UP YOUR HOME
Safety is very important for people with nerve damage. Nerve damage can increase the risk for falls and other injuries. To stay safe:
- Remove loose wires and rugs from areas where you walk.
- Do not keep small pets in your home.
- Fix uneven flooring in doorways.
- Have good lighting.
- Put handrails in the bathtub or shower and next to the toilet. Place a slip-proof mat in the bathtub or shower.
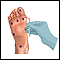
WATCHING YOUR SKIN
Wear shoes at all times to protect your feet from injury. Before you put them on, always check inside your shoes for stones or rough areas that may hurt your feet.
Check your feet every day. Look at the top, sides, soles, heels, and between the toes. Wash your feet every day with lukewarm water and mild soap. Use lotion, petroleum jelly, lanolin, or oil on dry skin.
Check bathwater temperature with your elbow before putting your feet in the water.
Avoid putting pressure on areas with nerve damage for too long.
TREATING PAIN
Medicines may help reduce pain in the feet, legs, and arms. They usually do not bring back loss of feeling. Your provider may prescribe:
- Pain pills
- Topical agents that relieve pain
- Medicines that treat seizures or depression, which can also manage pain
Your provider may refer you to a pain specialist. Talk therapy may help you better understand how your pain is affecting your life. It can also help you learn ways to better cope with pain.
TREATING OTHER SYMPTOMS
Taking medicine, sleeping with your head raised, and wearing elastic stockings may help with low blood pressure and fainting. Your provider may give you medicines to help with bowel movement problems. Eating small, frequent meals may help. To help bladder problems, your provider may suggest that you:
- Do Kegel exercises to strengthen your pelvic floor muscles.
- Use a urinary catheter, a thin tube inserted into your bladder to drain urine.
- Take medicines.
Medicines can often help with erection problems.
Support Groups
More information and support for people with peripheral neuropathy and their families can be found at:
- The Foundation for Peripheral Neuropathy -- www.foundationforpn.org/
Outlook (Prognosis)
How well you do depends on the cause and duration of nerve damage.
Some nerve-related problems do not interfere with daily life. Others get worse quickly and may lead to long-term, severe symptoms and problems.
When a medical condition can be found and treated, your outlook may be excellent. But sometimes, nerve damage can be permanent, even if the cause is treated.
Long-term (chronic) pain can be a major problem for some people. Numbness in the feet can lead to skin sores that do not heal. In rare cases, numbness in the feet may lead to amputation.
There is no cure for most neuropathies that are passed down in families.
When to Contact a Medical Professional
Contact your provider if you have symptoms of nerve damage. Early treatment increases the chance of controlling symptoms and preventing more problems.
Prevention
You can prevent some causes of nerve damage.
- Avoid alcohol or drink only in moderation.
- Follow a balanced diet.
- Keep good control over diabetes and other medical problems.
- Learn about chemicals used at your workplace.
Alternative Names
Peripheral neuritis; Neuropathy - peripheral; Neuritis - peripheral; Nerve disease; Polyneuropathy; Chronic pain - peripheral neuropathy
References
Katirji B. Disorders of peripheral nerves. In: Jankovic J, Mazziotta JC, Pomeroy SL, Newman NJ, eds. Bradley and Daroff's Neurology in Clinical Practice. 8th ed. Philadelphia, PA: Elsevier; 2022:chap 106.
Smith G, Shy ME. Peripheral neuropathies. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 388.
Review Date 6/13/2024
Updated by: Joseph V. Campellone, MD, Department of Neurology, Cooper Medical School at Rowan University, Camden, NJ. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.