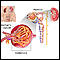
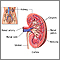
Acute nephritic syndrome is a group of symptoms that occur with some conditions that cause swelling and inflammation of the glomeruli in the kidney, or glomerulonephritis.
Causes
Acute nephritic syndrome is often caused by an immune response triggered by an infection or other disease.
Common causes in children and adolescents include:
- Hemolytic uremic syndrome (condition that occurs when an infection in the digestive system produces toxic substances that destroy red blood cells and cause kidney injury)
- Henoch-Schönlein purpura (disease that involves purple spots on the skin, joint pain, gastrointestinal problems and glomerulonephritis)
- IgA nephropathy (condition in which antibodies called IgA build up in kidney tissue)
- Post-streptococcal glomerulonephritis (kidney condition that occurs after infection with certain strains of streptococcus bacteria)
Common causes in adults include:
- Abdominal abscesses
- Goodpasture syndrome (also called anti-glomerular basement membrane disease in which the immune system attacks the glomerular basement membrane)
- Hepatitis B or C
- Endocarditis (inflammation of the inside lining of the heart chambers and heart valves caused by a bacterial or fungal infection)
- Membranoproliferative glomerulonephritis (condition that involves inflammation and changes to kidney cells)
- Rapidly progressive (crescentic) glomerulonephritis (a form of glomerulonephritis that leads to a rapid loss of kidney function)
- Lupus nephritis (kidney complication of systemic lupus erythematosus)
- Vasculitis (inflammation of the blood vessels)
- Viral diseases such as mononucleosis, measles, and mumps
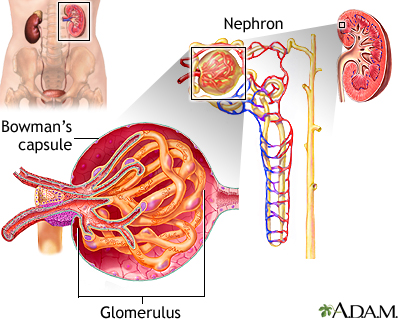
The inflammation affects the function of the glomerulus. This is the part of the kidney that filters blood to make urine and remove waste. As a result, blood and protein appear in the urine, and excess fluid builds up in the body.
Swelling of the body occurs when the blood loses a protein called albumin. Albumin keeps fluid in the blood vessels. When it is lost, fluid collects in the body tissues.
Blood loss from the damaged kidney structures leads to blood in the urine.
Symptoms
Common symptoms of nephritic syndrome are:
- Blood in the urine (urine appears dark, tea-colored, or cloudy)
- Decreased urine output (little or no urine may be produced)
- Swelling of the face, eye socket, legs, arms, hands, feet, abdomen, or other areas
- High blood pressure
Other symptoms that may occur include:
- Blurred vision, usually from burst blood vessels in the retina of the eye
- Cough containing mucus or pink, frothy material from fluid buildup in the lungs
- Shortness of breath, from fluid buildup in the lungs
- General ill feeling (malaise), drowsiness, confusion, aches and pains, headache
Symptoms of acute kidney failure or long-term (chronic) kidney disease may develop.
Exams and Tests
During an examination, your health care provider may find the following signs:
- High blood pressure
- Abnormal heart and lung sounds
- Signs of excess fluid (edema) such as swelling in the legs, arms, face, and belly
- Enlarged liver
- Enlarged veins in the neck
Tests that may be done include:
- Blood creatinine
- Blood electrolytes
- Blood urea nitrogen (BUN)
- Creatinine clearance
- Urine protein
- Urinalysis
A kidney biopsy will show inflammation of the glomeruli, which may indicate the cause of the condition.
Tests to find the cause of acute nephritic syndrome may include:
- ANA titer for lupus
- Antiglomerular basement membrane antibody
- Antineutrophil cytoplasmic antibody for vasculitis (ANCA)
- Blood culture
- Culture of the throat or skin
- Serum complement (C3 and C4)
Treatment
The goal of treatment is to reduce inflammation in the kidney and control high blood pressure. You may need to stay in a hospital to be diagnosed and treated.
Your provider may recommend:
- Bedrest until you feel better with treatment
- A diet that limits salt, fluids, and potassium
- Medicines to control high blood pressure, reduce inflammation, or to remove fluid from your body
- Kidney dialysis, if needed
Outlook (Prognosis)
The outlook depends on the disease that is causing the nephritis. When the condition improves, symptoms of fluid retention (such as swelling and cough) and high blood pressure may go away in 1 or 2 weeks. Urine tests may take months to return to normal.
Children tend to do better than adults and usually recover completely. Only rarely do they develop complications or progress to chronic glomerulonephritis and chronic kidney disease.
Adults do not recover as well or as quickly as children. Although it is unusual for the disease to return, in some adults, the disease does return and they will develop end-stage kidney disease and may need dialysis or a kidney transplant.
When to Contact a Medical Professional
Contact your provider if you have symptoms of acute nephritic syndrome.
Prevention
Often, the condition cannot be prevented, although treatment of illness and infection may help to reduce the risk.
Alternative Names
Glomerulonephritis - acute; Acute glomerulonephritis; Nephritis syndrome - acute
References
Flores FX. Isolated glomerular diseases associated with recurrent gross hematuria. In: Kliegman RM, St. Geme JW, Blum NJ, et al, eds. Nelson Textbook of Pediatrics. 22nd ed. Philadelphia, PA: Elsevier; 2025:chap 559.
Radhakrishnan J, Stokes MB. Glomerular disorders and nephrotic syndromes. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 107.
Saha M, Pendergraft WF, Jennette JC, Falk RJ. Primary glomerular disease. In: Yu ASL, Chertow GM, Luyckx VA, Marsden PA, Skorecki K, Taal MW, eds. Brenner and Rector's The Kidney. 11th ed. Philadelphia, PA: Elsevier; 2020:chap 31.
Review Date 9/2/2025
Updated by: Walead Latif, MD, Nephrologist and Clinical Associate Professor, Rutgers Medical School, Newark, NJ. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.