Anti-glomerular basement membrane disease (anti-GBM disease) is a rare disorder that can involve quickly worsening kidney failure and lung disease.
Some forms of the disease involve just the lungs or the kidneys. Anti-GBM disease used to be known as Goodpasture syndrome.
Causes
Anti-GBM disease is an autoimmune disorder. It occurs when the immune system mistakenly attacks and destroys healthy body tissue. People with this syndrome develop substances that attack a protein called collagen in the tiny air sacs in the lungs and the filtering units (glomeruli) of the kidneys.
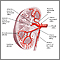
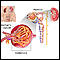
These substances are called anti-GBM antibodies. The glomerular basement membrane is a part of the kidneys that helps filter waste and extra fluid from the blood. Anti-GBM antibodies are antibodies against this membrane. They can damage the basement membrane, which can lead to kidney damage.
Sometimes, this disorder is triggered by a viral respiratory infection or by breathing in hydrocarbon solvents. In such cases, the immune system may attack organs or tissues because it mistakes them for these viruses or foreign chemicals.
The immune system's faulty response causes bleeding in the air sacs of the lungs and inflammation in the kidney's filtering units.
Symptoms
Symptoms may occur very slowly over months or even years, but they often develop very quickly over days to weeks.
Loss of appetite, fatigue, and weakness are common early symptoms.
Lung symptoms may include:
- Coughing up blood
- Dry cough
- Shortness of breath
Kidney and other symptoms include:
- Bloody urine
- Burning sensation when urinating
- Nausea and vomiting
- Pale skin
- Swelling (edema) in any area of the body, especially in the legs
Exams and Tests
A physical exam may reveal high blood pressure and signs of fluid overload. Your health care provider may hear abnormal heart and lung sounds when listening to the chest with a stethoscope.
Urinalysis results are often abnormal and show blood and protein in the urine. Abnormal red blood cells may be seen.
The following tests may also be done:
Treatment
The main goal is to remove the harmful antibodies from the blood. Treatment may include:
- Plasmapheresis, which removes harmful antibodies to help reduce inflammation in the kidneys and lungs.
- Corticosteroid medicines (such as prednisone) and other medicines, which suppress or quiet the immune system.
- Medicines such as angiotensin-converting enzyme (ACE) inhibitors or angiotensin receptor blockers (ARBs), which help control blood pressure.
- Dialysis, which may be done if kidney failure is severe and can no longer be treated by other means.
- A kidney transplant, which may be done when your kidneys no longer function.
You may be told to limit your intake of salt and fluids to control swelling. In some cases, a low-to-moderate protein diet may be recommended.
Support Groups
More information and support for people with anti-GBM disease and their families can be found at:
- National Institute of Diabetes and Digestive and Kidney Diseases -- www.niddk.nih.gov/health-information/kidney-disease/glomerular-disease/anti-gbm-goodpastures-disease
- National Kidney Foundation -- www.kidney.org/kidney-topics/goodpasture-syndrome
- National Organization for Rare Disorders -- rarediseases.org/rare-diseases/goodpasture-syndrome
Outlook (Prognosis)
An early diagnosis is very important. The outlook is much worse if the kidneys are already severely damaged when treatment begins. Lung damage can range from mild to severe.
Many people will need dialysis or a kidney transplant.
Possible Complications
Untreated, this condition can lead to any of the following:
- Chronic kidney disease
- End-stage kidney disease
- Lung failure
- Rapidly progressive glomerulonephritis
- Severe pulmonary hemorrhage (lung bleeding)
When to Contact a Medical Professional
Contact your provider for an appointment if you are producing less urine, or you have any other symptoms of anti-GBM disease.
Prevention
Never sniff glue or siphon gasoline with your mouth, which exposes the lungs to hydrocarbon solvents and can cause this disease.
Alternative Names
Goodpasture syndrome; Rapidly progressive glomerulonephritis with pulmonary hemorrhage; Pulmonary renal syndrome; Glomerulonephritis - pulmonary hemorrhage
References
Phelps RG, Turner AN. Anti-glomerular basement membrane disease and Goodpasture disease. In: Johnson RJ, Floege J, Tonelli M, eds. Comprehensive Clinical Nephrology. 7th ed. Philadelphia, PA: Elsevier; 2024:chap 25.
Radhakrishnan J, Appel GB, D'Agati VD. Secondary glomerular disease. In: Yu ASL, Chertow GM, Luyckx VA, Marsden PA, Skorecki K, Taal MW, eds. Brenner and Rector's The Kidney. 11th ed. Philadelphia, PA: Elsevier; 2020:chap 32.
Radhakrishnan J, Stokes MB. Glomerular disorders and nephrotic syndromes. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 107.
Schwarz MI, Matson S. Diffuse alveolar hemorrhage. In: Broaddus VC, Ernst JD, King TE, et al, eds. Murray and Nadel's Textbook of Respiratory Medicine. 7th ed. Philadelphia, PA: Elsevier; 2022:chap 94.
Review Date 9/2/2025
Updated by: Walead Latif, MD, Nephrologist and Clinical Associate Professor, Rutgers Medical School, Newark, NJ. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.