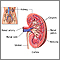
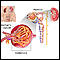
Poststreptococcal glomerulonephritis (GN) is a kidney condition that occurs after infection with certain strains of streptococcus bacteria.
Causes
Poststreptococcal GN is a form of glomerulonephritis. It is caused by an infection with a type of streptococcus bacteria. The infection does not occur in the kidneys, but in a different part of the body, such as the skin or throat. The condition may develop 1 to 2 weeks after an untreated throat infection, or 3 to 4 weeks after a skin infection.
It may occur in people of any age, but it most often occurs in children ages 6 through 10. Although skin and throat infections are common in children, poststreptococcal GN is rarely a complication of these infections. Poststreptococcal GN causes the tiny blood vessels in the filtering units of the kidneys (glomeruli) to become inflamed. This makes the kidneys less able to filter the blood to create urine.
The condition is not common today because infections that can lead to the disorder are treated with antibiotics.
Risk factors include:
- Strep throat
- Streptococcal skin infections (such as impetigo)
Symptoms
Symptoms may include any of the following:
- Decreased urine output
- Rust-colored urine (due to blood)
- Swelling (edema), general swelling, swelling of the abdomen, swelling of the face or eyes, swelling of the feet, ankles, hands
- Visible blood in the urine
- Joint pain
- Joint stiffness or swelling
Exams and Tests
A physical exam shows swelling (edema), especially in the face. Abnormal sounds may be heard when listening to the heart and lungs with a stethoscope. Blood pressure is often high.
Other tests that may be done include:
- Anti-DNase B
- Serum ASO (and streptolysin O)
- Serum complement levels
- Serum creatinine
- Urinalysis
- Kidney biopsy (usually not needed)
Treatment
There is no specific treatment for this condition. Treatment is focused on relieving symptoms.
- Antibiotics, such as penicillin, will likely be used to destroy any streptococcal bacteria that remain in the body.
- Blood pressure medicines and diuretic medicines may be needed to control swelling and high blood pressure.
- Corticosteroids and other anti-inflammatory medicines are generally not effective.
You may need to limit salt in your diet to control swelling and high blood pressure.
Outlook (Prognosis)
Poststreptococcal GN usually goes away by itself after several weeks to months.
In small number of adults, it may get worse and lead to long-term (chronic) kidney failure. Sometimes, it can progress to end-stage kidney disease, which requires dialysis and a kidney transplant.
Possible Complications
Health problems that may result from this condition include:
- Acute renal failure (rapid loss of kidneys' ability to remove waste and help balance fluids and electrolytes in the body)
- Chronic glomerulonephritis
- Chronic kidney disease
- Heart failure or pulmonary edema (fluid buildup in the lungs)
- End-stage renal disease
- Hyperkalemia (abnormally high potassium level in the blood)
- High blood pressure (hypertension)
- Nephrotic syndrome (group of symptoms that include protein in the urine, low blood protein levels in the blood, high cholesterol levels, high triglyceride levels, and swelling)
When to Contact a Medical Professional
Contact your health care provider if:
- You have symptoms of poststreptococcal GN
- You have poststreptococcal GN, and you have decreased urine output or other new symptoms
Prevention
Treating known streptococcal infections may help prevent poststreptococcal GN. Also, practicing good hygiene such as washing hands often prevents the spread of the infection.
Alternative Names
Glomerulonephritis - poststreptococcal; Postinfectious glomerulonephritis
References
Flores FX. Isolated glomerular diseases associated with recurrent gross hematuria. In: Kliegman RM, St. Geme JW, Blum NJ, et al, eds. Nelson Textbook of Pediatrics. 22nd ed. Philadelphia, PA: Elsevier; 2025:chap 559.
Radhakrishnan J, Stokes MB. Glomerular disorders and nephrotic syndromes. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 107.
Saha MK, Pendergraft WF, Jennette JC, Falk RJ. Primary glomerular disease. In: Yu ASL, Chertow GM, Luyckx VA, Marsden PA, Skorecki K, Taal MW, eds. Brenner and Rector's The Kidney. 11th ed. Philadelphia, PA: Elsevier; 2020:chap 31.
Stevens DL, Bryant AE, Hagman MM. Nonpneumococcal streptococcal infections and rheumatic fever. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 269.
Review Date 9/2/2025
Updated by: Walead Latif, MD, Nephrologist and Clinical Associate Professor, Rutgers Medical School, Newark, NJ. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.