Small cell lung cancer (SCLC) is a fast-growing type of lung cancer. It tends to spread more quickly than non-small cell lung cancer.
There are two types of SCLC:
- Small cell carcinoma (oat cell cancer)
- Combined small cell carcinoma and non-small cell lung cancer
Most SCLCs are of the oat cell type.
Causes
About 15% of all lung cancer cases are SCLC. Small cell lung cancer is slightly more common in men than women.
Almost all cases of SCLC are due to cigarette smoking. SCLC is very rare in people who have never smoked.
SCLC is the most aggressive form of lung cancer. It usually starts in the breathing tubes (bronchi) in the center of the chest. Although the cancer cells are small, they grow very quickly and create large tumors. These tumors often spread rapidly (metastasize) to other parts of the body, including the brain, liver, and bone.
Symptoms
Symptoms of SCLC include:
- Bloody sputum (phlegm)
- Chest pain
- Cough
- Loss of appetite
- Shortness of breath
- Weight loss
- Wheezing
Other symptoms that may occur with this disease, especially in the late stages, include:
Exams and Tests
Your health care provider will perform a physical exam and ask about your medical history. You will be asked whether you smoke, and if so, how much and for how long.
When listening to your chest with a stethoscope, your provider may hear fluid around the lungs or areas where the lung has partially collapsed. Each of these findings may suggest cancer.
SCLC has usually spread to other parts of your body by the time it is diagnosed.
Tests that may be performed include:
- Bone scan
- Chest x-ray
- Complete blood count (CBC)
- CT scan
- Liver function tests
- MRI scan
- Positron emission tomography (PET) scan
- Sputum cytology test (to look for cancer cells), seldom done today
- Thoracentesis (removal of fluid from the chest cavity around the lungs)
In most cases, a piece of tissue is removed from your lungs or other areas to be examined under a microscope. This is called a biopsy. There are several ways to do a biopsy:
- Bronchoscopy combined with biopsy
- CT scan-directed needle biopsy
- Endoscopic esophageal or bronchial ultrasound with biopsy
- Mediastinoscopy with biopsy
- Open lung biopsy
- Pleural biopsy
- Video-assisted thoracoscopy
Usually, if a biopsy shows cancer, more imaging tests are done to find out the stage of the cancer. Stage means how far it has spread. SCLC is classified as either:
- Limited -- Cancer is only in the chest and can be treated with radiation therapy.
- Extensive -- Cancer has spread outside the area that can be covered by radiation therapy.
Treatment
Because SCLC spreads quickly throughout the body, treatment will include cancer-killing medicines (chemotherapy), which are usually given through a vein (by IV).
Treatment with chemotherapy and immunotherapy, and possibly radiation, may be done for people with SCLC that has spread throughout the body (extensive). In this case, the treatment only helps relieve symptoms and prolongs life, but does not cure the disease.
Radiation therapy can be used with chemotherapy if the disease is confined to one area within the chest (limited).
Radiation therapy uses powerful x-rays or other forms of radiation to kill cancer cells.
Radiation may be used to:
- Treat the cancer, along with chemotherapy, if surgery is not possible.
- Help relieve symptoms caused by the cancer, such as breathing problems and swelling.
- Help relieve cancer pain when the cancer has spread to the bones.
Often, SCLC may have already spread to the brain. This can occur even when there are no symptoms or other signs of cancer in the brain. As a result, some people with smaller cancers, or who had a good response in their first round of chemotherapy, may receive radiation therapy to the brain. This therapy, called prophylactic cranial irradiation, is done to prevent growth of the cancer in the brain.
Surgery helps very few people with SCLC because the disease has often spread by the time it is diagnosed. Surgery may be done when there is only one tumor that has not spread. If surgery is done, chemotherapy or radiation therapy is still needed.
Support Groups
You can ease the stress of illness by joining a cancer support group. Sharing with others who have common experiences and problems can help you not feel alone.
Outlook (Prognosis)
How well you do depends on how much the lung cancer has spread. SCLC is very deadly. Not many people with this type of cancer are still alive 5 years after diagnosis.
Treatment can often prolong life to more than 12 months, even when the cancer has spread.
In rare cases, if SCLC is diagnosed early, treatment may result in a long-term cure.
When to Contact a Medical Professional
Contact your provider if you have symptoms of lung cancer, particularly if you smoke.
Prevention
If you smoke, now is the time to quit. If you are having trouble quitting, talk with your provider. There are many methods to help you quit, from support groups to prescription medicines. Also try to avoid secondhand smoke.
If you smoke or used to smoke, talk with your provider about getting screened for lung cancer. To get screened, you need to have a CT scan of the chest.
Alternative Names
Cancer - lung - small cell; Small cell lung cancer; SCLC
Images
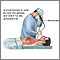 Bronchoscopy
Bronchoscopy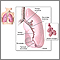 Lungs
Lungs Lung cancer - lateral chest x-ray
Lung cancer - lateral chest x-ray Lung cancer - frontal chest x-ray
Lung cancer - frontal chest x-ray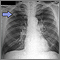 Adenocarcinoma - chest x-ray
Adenocarcinoma - chest x-ray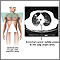 Bronchial cancer - CT scan
Bronchial cancer - CT scan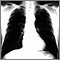 Bronchial cancer - chest x-ray
Bronchial cancer - chest x-ray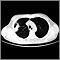 Lung with squamous cell cancer - CT scan
Lung with squamous cell cancer - CT scan Lung cancer - chemotherapy treatment
Lung cancer - chemotherapy treatment Adenocarcinoma
Adenocarcinoma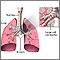 Non-small cell carcinoma
Non-small cell carcinoma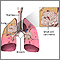 Small cell carcinoma
Small cell carcinoma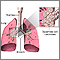 Squamous cell carcinoma
Squamous cell carcinoma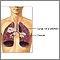 Secondhand smoke and lung cancer
Secondhand smoke and lung cancer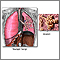 Normal lungs and alveoli
Normal lungs and alveoli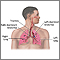 Respiratory system
Respiratory system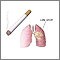 Smoking hazards
Smoking hazards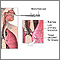 Bronchoscope
Bronchoscope
References
Araujo LH, Horn L, Merritt RE, Shilo K, Xu-Welliver M, Carbone DP. Cancer of the lung: non-small cell lung cancer and small cell lung cancer. In: Niederhuber JE, Armitage JO, Kastan MB, Doroshow JH, Tepper JE, eds. Abeloff's Clinical Oncology. 6th ed. Philadelphia, PA: Elsevier; 2020:chap 69.
National Comprehensive Cancer Network website. NCCN clinical practice guidelines in oncology: Small cell lung cancer. Version 4. 2025. www.nccn.org/professionals/physician_gls/pdf/sclc.pdf. Updated January 13, 2025. Accessed July 18, 2025.
National Cancer Institute website. Small cell lung cancer treatment (PDQ) - health professional version. www.cancer.gov/types/lung/hp/small-cell-lung-treatment-pdq. Updated May 14, 2025. Accessed July 18, 2025.
Rivera MP, Mody GN, Weiner AA. Lung cancer: treatment. In: Broaddus VC, Ernst JD, Talmadge EK, et al, eds. Murray and Nadel's Textbook of Respiratory Medicine. 7th ed. Philadelphia, PA: Elsevier; 2022:chap 77.
Review Date 7/9/2025
Updated by: Warren Brenner, MD, Oncologist, Lynn Cancer Institute, Boca Raton, FL. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.




















