Your child has epilepsy. People with epilepsy have seizures. A seizure is a sudden brief change in the electrical and chemical activity in the brain.
After your child goes home from the hospital, follow your health care provider's instructions on how to care for your child. Use the information below as a reminder.
When Your Child was in the Hospital
In the hospital, the provider gave your child a physical and nervous system exam and did some tests to find out the cause of your child's seizures.
What to Expect at Home
If your provider sent your child home with medicines, it is to help prevent more seizures occurring in your child. The medicine can help your child avoid having seizures, but it does not guarantee that seizures will not occur. Your provider may need to change the dosage of your child's seizure medicines or use different medicines if seizures persist despite your child taking the medicines, or because your child is having side effects.
Activity and Lifestyle
Your child should get plenty of sleep and try to have as regular schedule as possible. Try to avoid too much stress. You should still set rules and limits, along with consequences, for a child with epilepsy.
Make sure your home is safe to help prevent injuries when a seizure takes place:
- Keep bathroom and bedroom doors unlocked. Keep these doors from being blocked.
- Make sure your child stays safe in the bathroom. Younger children should not take a bath without someone present. Do not leave the bathroom without taking your child with you. Older children should only take showers.
- Put pads on sharp corners of furniture.
- Place a screen in front of the fireplace.
- Use nonslip flooring or cushioned floor covers.
- Do not use freestanding heaters.
- Avoid letting a child with epilepsy sleep on the top bunk.
- Replace all glass doors and any windows near the ground with either safety glass or plastic.
- Plastic cups should be used instead of glassware.
- Supervise the use of knives and scissors.
- Supervise your child in the kitchen.
Most children with seizures can lead an active lifestyle. You should still plan ahead for the possible dangers of certain activities. These activities should be avoided if a loss of consciousness or control would result in an injury.
- Safe activities include jogging, aerobics, moderate cross-country skiing, dancing, tennis, golf, hiking, and bowling. Games and playing in gym class or on the playground are generally OK.
- Supervise your child when swimming.
- To prevent head injury, your child should wear a helmet during bike riding, skateboarding, downhill skiing, and similar activities.
- Children should have someone to help them climb on a jungle gym or perform gymnastics.
- Ask your child's provider about your child participating in contact sports.
- Also ask if your child should avoid places or situations that expose your child to flashing lights or contrasting patterns such as checks or stripes. In some people with epilepsy, seizures can be triggered by flashing lights or patterns.
Have your child carry and take seizure medicines at school. Teachers and others at schools should know about your child's seizures and seizure medicines.
Your child should wear a medical alert bracelet. Tell family members, friends, teachers, school nurses, babysitters, swimming instructors, lifeguards, and coaches about your child's seizure disorder.
Seizure Medicines
Do not stop giving your child seizure medicines without talking with your child's provider.
Do not stop giving your child seizure medicines just because the seizures have stopped.
Tips for taking seizure medicines:
- Do not skip a dose.
- Get refills before the medicine runs out.
- Keep seizure medicines in a safe place, away from young children.
- Store medicines in a dry place, in the bottle that they came in.
- Dispose of expired medicines properly. Check with your pharmacy or online for a medicine take-back location near you.
If your child misses a dose:
- Have them take it as soon as you remember.
- If it is already time for the next dose, skip the dose that you forgot to give your child and go back to the schedule. Do not give a double dose.
- If your child misses more than one dose, talk with the child's provider.
Drinking alcohol and taking illegal drugs can change the way seizure medicines work. It is never too early to warn your child of this possible problem.
Your provider may need to check your child's blood level of the seizure medicine on a regular basis.
Seizure medicines have side effects. If your child started taking a new medicine recently, or your provider changed your child's dose, these side effects may go away. Always ask your child's provider about any possible side effects. Also, talk to your child's provider about foods or other medicines that can change the blood level of an anti-seizure medicine.
How to Respond to a Seizure
Once a seizure starts, family members and caregivers can help make sure the child is safe from further injury and call for help, if needed. Your child's provider may have prescribed a medicine that can be given during a prolonged seizure to make it stop sooner. Follow instructions on how to give the medicine to the child.
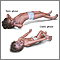
When a seizure occurs, the main goal is to protect the child from injury and make sure the child can breathe well. Try to prevent a fall. Help the child to the ground in a safe area. Clear the area of furniture or other sharp objects. Turn the child on their side to make sure the child's airway does not get obstructed during the seizure.
- Cushion the child's head.
- Loosen tight clothing, particularly around the child's neck.
- Turn the child on their side. If vomiting occurs, turning the child on their side helps make sure that they do not inhale vomit into their lungs.
- Stay with the child until they recover, or medical help arrives. Meanwhile, monitor the child's pulse and rate of breathing (vital signs).
Things to avoid:
- Do not restrain (try to hold down) the child.
- Do not place anything between the child's teeth during a seizure (including your fingers).
- Do not move the child unless they are in danger or near something hazardous.
- Do not try to make the child stop convulsing. They have no control over the seizure and are not aware of what is happening at the time.
- Do not give the child anything by mouth until the convulsions have stopped and the child is fully awake and alert.
- Do not start CPR unless the child has clearly stopped having the seizure and is still not breathing and has no pulse.
When to Call the Doctor
Contact your child's provider if your child has:
- Seizures that have been happening more often
- Side effects from medicines
- Unusual behavior that was not present before
- Weakness, problems with seeing, or balance problems that are new
Call 911 or the local emergency number if:
- A seizure lasts more than 2 to 5 minutes.
- Your child does not wake up or have normal behavior within a reasonable time after a seizure.
- Another seizure starts before your child returns to awareness after a seizure ends.
- Your child had a seizure in water or appears to have inhaled vomit or any other substance.
- The person is injured or has diabetes.
- There is anything different about this seizure compared to the child's usual seizures.
Alternative Names
Seizure disorder in children - discharge
Images
References
Mikati MA, Tchapyjnikov D, Rathke KM. Seizures in childhood. In: Kliegman RM, St. Geme JW, Blum NJ, et al, eds. Nelson Textbook of Pediatrics. 22nd ed. Philadelphia, PA: Elsevier; 2025:chap 633.
Pearl PL. Overview of seizures and epilepsy in children. In: Swaiman KF, Ashwal S, Ferriero DM, et al, eds. Swaiman's Pediatric Neurology: Principles and Practice. 6th ed. Philadelphia, PA: Elsevier; 2017:chap 61.
Review Date 8/19/2024
Updated by: Joseph V. Campellone, MD, Department of Neurology, Cooper Medical School at Rowan University, Camden, NJ. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.