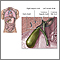
Open gallbladder removal is surgery to remove the gallbladder through a large cut in your abdomen.
When You're in the Hospital
You had surgery to remove your gallbladder. The surgeon made an incision (cut) in your belly. The surgeon then removed your gallbladder by reaching in through the incision, separating it from its attachments, and lifting it out.
What to Expect at Home
Recovering from open gallbladder removal surgery takes 4 to 8 weeks. You may have some of these symptoms as you recover:
- Incision pain for a few weeks. This pain should get better each day.
- Sore throat from the breathing tube. Throat lozenges may be soothing.
- Nausea, and maybe throwing up (vomiting). Your surgeon can provide you with nausea medicine, if needed.
- Loose stools after eating. This may last 4 to 8 weeks. Rarely, the diarrhea can continue. Your health care provider can discuss treatment options with you.
- Bruising around your wound. This will go away on its own.
- A small amount of skin redness just around the edge of your wound. This is normal.
- A small amount of watery or dark bloody fluid from the incision. This is normal for several days after surgery.
The surgeon may have left one or two drainage tubes in your belly:
- One will help remove any fluid or blood that is left in your belly.
- The second tube will drain bile while you recover. This tube will be removed by your surgeon in 2 to 4 weeks. Before the tube is removed, you will have a special x-ray called a cholangiogram.
- You will receive instructions for caring for these drains before leaving the hospital.
Activity
Plan to have someone drive you home from the hospital. You will not be allowed to drive yourself home.
You should be able to do most of your regular activities in 4 to 8 weeks. Before that:
- Do not lift anything heavy enough to cause pain or pull at the incision.
- Avoid all strenuous activity until you feel up to it. This includes heavy exercising, weightlifting, and other activities that make you breathe hard, strain, cause pain or pull on the incision. It may take several weeks for you to be able to do these kinds of activities.
- Taking short walks and using stairs are OK.
- Light housework is OK.
- Do not push yourself too hard. Slowly increase how much you exercise.
Managing pain:
- Your provider will prescribe pain medicines to use at home.
- Some providers may put you on a regiment of alternating scheduled acetaminophen (Tylenol) and ibuprofen, using narcotic pain medicine as a backup.
- If you are taking pain pills 3 or 4 times a day, try taking them at the same times each day for 3 to 4 days. They may be more effective this way.
Press a pillow over your incision when you cough or sneeze to ease discomfort and protect your incision.
Wound Care
Your incision may have been closed with a dissolving suture under the skin and glue on the surface. If so, you can shower the day after surgery without covering the incision. Leave the glue alone. It will come off on its own in a few weeks.
If your incision was closed with staples or stitches that need to be removed, it may be covered with a bandage. Change the dressing over your surgical wound once a day, or sooner if it becomes dirty. Your provider will tell you when you no longer need to keep your wound covered. Keep the wound area clean by washing it with mild soap and water. You may remove the wound dressings and take showers the day after surgery.
If tape strips (Steri-strips) were used to close your incision, cover the incision with plastic wrap before showering for the first week. Do not try to wash off the Steri-strips. Let them fall off on their own.
Do not soak in a bathtub, hot tub, or go swimming until your provider tells you it is OK.
Self-care
Eat a normal diet, but you may want to avoid greasy or spicy foods for a while.
If you have hard stools:
- Try to walk and be more active, but do not overdo it.
- If you can, take less of the narcotic pain medicine your provider gave you. Some can cause constipation. You can use acetaminophen (Tylenol) or ibuprofen instead if it is OK with your surgeon.
- Try a stool softener. You can get these at any pharmacy without a prescription.
- Ask your provider whether you can take milk of magnesia or magnesium citrate. Do not take any laxatives without first asking your provider.
- Ask your provider about foods that are high in fiber, or try using an over-the-counter fiber product such as psyllium (Metamucil).
Follow-up
You will see your provider for a follow-up appointment in the weeks after your gallbladder removal surgery.
When to Call the Doctor
Contact your provider if:
- You have a fever above 101°F (38.3°C).
- Your surgical wound is bleeding, red, or warm to the touch.
- Your surgical wound has thick, yellow or green drainage.
- You have pain that is not helped with your pain medicines.
- It is hard to breathe.
- You have a cough that does not go away.
- You cannot drink or eat.
- Your skin or the white part of your eyes turns yellow.
- Your stools are a gray color.
Alternative Names
Cholelithiasis - open discharge; Biliary calculus - open discharge; Gallstones - open discharge; Cholecystitis - open discharge; Cholecystectomy - open discharge
Images
References
American College of Surgeons. Cholecystectomy: surgical removal of the gallbladder. American College of Surgeons Operation Brochures for Patients. www.facs.org/media/sskdidat/cholecys.pdf. Updated 2022. Accessed October 17, 2024.
Quick CRG, Biers SM, Arulampalam THA. Gallstone diseases and related disorders. In: Quick CRG, Biers SM, Arulampalam THA, eds. Essential Surgery Problems, Diagnosis and Management. 6th ed. Philadelphia, PA: Elsevier; 2020:chap 20.
Radkani P, Hawksworth J, Fishbein T. Biliary system. In: Townsend CM Jr, Beauchamp RD, Evers BM, Mattox KL, eds. Sabiston Textbook of Surgery. 21st ed. Philadelphia, PA: Elsevier; 2022:chap 55.
Patient Instructions
Review Date 9/30/2024
Updated by: Linda J. Vorvick, MD, Clinical Professor, Department of Family Medicine, UW Medicine, School of Medicine, University of Washington, Seattle, WA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.