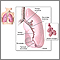
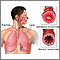
Asthma quick-relief medicines work fast to control asthma symptoms. You take them when you are coughing, wheezing, having trouble breathing, or having an asthma attack. They are also called rescue medicines.
Many of these medicines are called "bronchodilators" because they open (dilate) and help relax the muscles of your airways (bronchi).
You and your health care provider can make a plan for the quick-relief medicines that work for you. This plan will include when you should take them and how much you should take.
Plan ahead. Make sure you do not run out. Bring enough medicine with you when you travel.
Short-acting Beta-agonists
Short-acting beta-agonists are the most common quick-relief medicines for treating asthma attacks and are considered to be bronchodilators.
They can be used just before exercising to help prevent asthma symptoms caused by exercise. They work by relaxing the muscles of your airways, and this lets you breathe better during an attack.
Tell your provider if you are using quick-relief medicines twice a week or more to control your asthma symptoms. Your asthma may not be under control, and your provider may need to change your dose of daily control medicines.
Some quick-relief asthma medicines include:
- Albuterol (ProAir HFA, Proventil HFA, Ventolin HFA)
- Levalbuterol (Xopenex HFA)
- Metaproterenol
- Terbutaline
Short-acting beta-agonists may cause these side effects:
- Anxiety.
- Fast and irregular heartbeats. Contact your provider right away if you have this side effect.
- Headache.
- Restlessness.
- Tremor (your hand or another part of your body may shake).
Oral Steroids
Your provider might prescribe oral steroids when you have an asthma attack that is not going away. These are medicines that you take by mouth as pills, capsules, or liquids.
Oral steroids are not quick-relief medicines but are often given for 7 to 14 days when your symptoms flare-up.
Oral steroids include:
- Methylprednisolone
- Prednisone
- Prednisolone
Alternative Names
Asthma - quick-relief drugs - short-acting beta-agonists; Asthma - quick-relief drugs - bronchodilators; Asthma - quick-relief drugs - oral steroids; Asthma - rescue drugs; Bronchial asthma - quick relief; Reactive airway disease - quick relief; Exercise-induced asthma - quick relief
References
Drazen JM, Bel EH. Asthma. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 75.
Liu AH, Bacharier LB, Fitzpatrick AM, Sicherer SH. Childhood asthma. In: Kliegman RM, St. Geme JW, Blum NJ, et al, eds. Nelson Textbook of Pediatrics. 22nd ed. Philadelphia, PA: Elsevier; 2025:chap 185.
Lugogo N, Que LG, Carr TF, Kraft M. Asthma: diagnosis and management. In: Broaddus VC, Ernst JD, King TE, et al, eds. Murray and Nadel's Textbook of Respiratory Medicine. 7th ed. Philadelphia, PA: Elsevier; 2022:chap 62.
National Heart, Lung and Blood Institute website. Asthma management guidelines: focused updates 2020. www.nhlbi.nih.gov/health-topics/asthma-management-guidelines-2020-updates. Updated February 4, 2021. Accessed March 9, 2026.
O'Byrne PM, Satia I. Inhaled ß 2 - agonists. In: Burks AW, Holgate ST, O'Hehir RE, et al, eds. Middleton's Allergy: Principles and Practice. 9th ed. Philadelphia, PA: Elsevier; 2020:chap 93.
Viswanathan RK, Busse WW. Management of asthma in adolescents and adults. In: Burks AW, Holgate ST, O'Hehir RE, et al, eds. Middleton's Allergy: Principles and Practice. 9th ed. Philadelphia, PA: Elsevier; 2020:chap 52.
Patient Instructions
- Asthma and school
- Asthma - child - discharge
- Asthma - control drugs
- Asthma in adults - what to ask the doctor
- Asthma in children - what to ask your doctor
- Bronchiolitis - discharge
- Exercise-induced asthma
- Exercising and asthma at school
- How to use a nebulizer
- How to use an inhaler - no spacer
- How to use an inhaler - with spacer
- How to use your peak flow meter
- Make peak flow a habit
- Signs of an asthma attack
- Stay away from asthma triggers
Review Date 2/27/2026
Updated by: Jacob Berman, MD, MPH, Associate Professor of Medicine, Division of General Internal Medicine, University of Washington School of Medicine, Seattle, WA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.