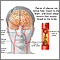
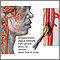
Carotid artery disease is when the carotid arteries become narrowed or blocked.
The carotid arteries provide part of the main blood supply to your brain. They are located on each side of your neck. You can feel their pulse under your jawline.
Causes
Carotid artery disease occurs when fatty material called plaque builds up inside the arteries. This buildup of plaque is called hardening of the arteries (atherosclerosis).
The plaque may slowly block or narrow the carotid artery. Or it may cause a clot to form suddenly. A clot that blocks the artery enough to reduce blood flow can lead to a stroke.
Risk factors for blockage or narrowing of the arteries include:
- Smoking (people who smoke one pack a day double their risk for stroke)
- Diabetes
- High blood pressure
- High cholesterol and triglycerides
- Older age
- Family history of stroke or blood vessel disorder
- Alcohol use
- Recreational drug use
- Trauma to the neck area, which may cause a tear in the carotid artery
- Radiation therapy to the neck
Symptoms
At early stages, you may not have any symptoms. After plaque builds up, the first symptoms of carotid artery disease may be a stroke or a transient ischemic attack (TIA). A TIA is due to a temporary reduction in blood flow to the brain that doesn't cause any lasting damage.
Symptoms of stroke and TIA include:
- Blurred vision
- Confusion
- Loss of memory
- Loss of sensation in one part of your body
- Problems with speech and language, including loss of speech
- Vision loss (partial or complete blindness)
- Weakness in one part of your body
- Problems with thinking, reasoning, and memory
Exams and Tests
Your health care provider will perform a physical exam. Your provider may use a stethoscope to listen to the blood flow in your neck for an abnormal sound called a bruit. This sound may be a sign of carotid artery disease.
Your provider also may find clots in the blood vessels of your eye. If you have had a stroke or TIA, a nervous system (neurological) exam will show other problems.
You may also have the following tests:
- Blood cholesterol and triglycerides test
- Blood sugar (glucose) test
- Ultrasound of the carotid arteries (carotid duplex ultrasound) to see how well blood is flowing through the carotid artery
The following imaging tests may be used to examine the blood vessels in the neck and brain:
Treatment
Treatment options for carotid artery disease include:
- Blood-thinning medicines such as aspirin, clopidogrel (Plavix), ticagrelor (Brilinta), warfarin (Coumadin), dabigatran (Pradaxa), or others to lower your risk for stroke
- Medicine and diet changes to lower your cholesterol or blood pressure
- No treatment, other than checking your carotid artery periodically
You may have certain procedures to treat a narrowed or blocked carotid artery:
- Carotid endarterectomy -- This surgery removes the plaque buildup in the carotid arteries.
- Carotid angioplasty and stenting -- This procedure opens a blocked artery and places a tiny wire mesh (stent) in the artery to keep it open.
Outlook (Prognosis)
Because there are no symptoms, you may not know you have carotid artery disease until you have a stroke or TIA.
- Some people who have a stroke recover most or all of their functions.
- Others die of the stroke itself or from complications.
- About one half of people who have a stroke have long-term problems.
Possible Complications
Major complications of carotid artery disease are:
- Transient ischemic attack. This occurs when a blot clot briefly blocks a blood vessel to the brain. It causes the same symptoms as a stroke. Symptoms last only a few minutes to an hour or two, but no longer than 24 hours. A TIA does not cause lasting damage. TIAs are a warning sign that a stroke may happen in the future if nothing is done to prevent it.
- Stroke. When the blood supply to the brain is partly or completely blocked, it may cause a stroke. Most often, this happens when a blood clot blocks a blood vessel to the brain. A stroke can also occur when a blood vessel breaks open or leaks. Strokes can cause long-term brain damage or death.
When to Contact a Medical Professional
Go to the emergency room or call the local emergency number (such as 911) as soon as symptoms occur. The sooner you receive treatment, the better your chance for recovery. With a stroke, every second of delay can cause more brain injury.
Prevention
Here's what you can do to help prevent carotid artery disease and stroke:
- Quit smoking.
- Follow a healthy, low-fat diet with plenty of fresh vegetables and fruits.
- Do not drink more than 1 to 2 alcoholic drinks a day.
- Do not use recreational drugs.
- Exercise at least 30 minutes a day, most days of the week.
- Get your cholesterol checked every 5 years. If you are being treated for high cholesterol, you may need to have it checked more often.
- Get your blood pressure checked every 1 to 2 years. If you have high blood pressure, heart disease, diabetes, or you have had a stroke, you need to have it checked more often. Ask your provider what is best for you.
- Follow your provider's treatment recommendations if you have high blood pressure, diabetes, high cholesterol, or heart disease.
Alternative Names
Carotid stenosis; Stenosis - carotid; Stroke - carotid artery; TIA - carotid artery
References
Biller J, Schneck MJ, Ruland S. Ischemic cerebrovascular disease. In: Jankovic J, Mazziotta JC, Pomeroy SL, Newman NJ, eds. Bradley and Daroff's Neurology in Clinical Practice. 8th ed. Philadelphia, PA: Elsevier; 2022:chap 65.
Kleindorfer DO, Towfighi A, Chaturvedi S, et al. 2021 Guideline for the prevention of stroke in patients with stroke and transient ischemic attack: A Guideline from the American Heart Association/American Stroke Association. Stroke. 2021;52(7):e364-e467. PMID: 34024117 pubmed.ncbi.nlm.nih.gov/34024117/.
Nguyen TN, Jovin TG, Nogueira RG, Zaidat OO. Principles of neuroendovascular therapy. In: Jankovic J, Mazziotta JC, Pomeroy SL, Newman NJ, eds. Bradley and Daroff's Neurology in Clinical Practice. 8th ed. Philadelphia, PA: Elsevier; 2022:chap 54.
Review Date 7/17/2025
Updated by: Joseph V. Campellone, MD, Department of Neurology, Cooper Medical School at Rowan University, Camden, NJ. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.