A cochlear implant is a small electronic device that helps people hear. It can be used for people who are deaf or very hard of hearing.
Information
A cochlear implant is not the same thing as a hearing aid. It is implanted using surgery and works in a different way.
There are many different types of cochlear implants. However, they are most often made up of several similar parts.
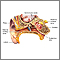
- One part of the device is surgically implanted into the bone surrounding the ear (temporal bone). It is made up of a receiver-stimulator, which accepts, decodes, and then sends an electrical signal to the brain.
- The second part of the cochlear implant is a device out of the body. This is made up of a microphone/receiver, a speech processor, and an antenna. This part of the implant receives the sound, converts the sound into an electrical signal, and sends it to the inside part of the cochlear implant.
WHO USES A COCHLEAR IMPLANT?
Cochlear implants allow deaf people to receive and process sounds and speech. However, these devices do not restore normal hearing. They are tools that allow sound and speech to be processed and sent to the brain.
A cochlear implant is not right for everyone. The way a person is selected for cochlear implants is changing as the understanding of the brain's hearing (auditory) pathways improves and the technology changes.
Both children and adults can be candidates for cochlear implants. People who are candidates for this device may have been born deaf or become deaf after learning to speak. Children as young as 1 year old are now candidates for this surgery. Although criteria are slightly different for adults and children, they are based on similar guidelines:
- The person should be completely or almost completely deaf in both ears and get almost no improvement with hearing aids. Anyone who can hear well enough with hearing aids is not a good candidate for cochlear implants.
- The person needs to be highly motivated. After the cochlear implant is placed, they must learn how to properly use the device.
- The person needs to have reasonable expectations for what will occur after surgery. The device does not restore or create "normal" hearing.
- Children need to be enrolled in programs that help them learn how to process sound.
- In order to determine if a person is a candidate for a cochlear implant, the person must be examined by an ear, nose, and throat (ENT) doctor (otolaryngologist). People will also need specific types of hearing tests performed with their hearing aids on.
- People may need a CT scan or MRI scan of the brain and the middle and inner ear.
- People (especially children) may need to be assessed by a psychologist to determine if they are good candidates.
HOW IT WORKS
Sounds are transmitted through the air. In a normal ear, sound waves cause the eardrum and then the middle ear bones to vibrate. This sends a wave of vibrations into the inner ear (cochlea). These waves are then converted by the cochlea into electrical signals, which are sent along the auditory nerve to the brain.
A deaf person does not have a functioning inner ear. A cochlear implant tries to replace the function of the inner ear by turning sound into electrical energy. This energy can then be used to stimulate the cochlear nerve (the nerve for hearing), sending "sound" signals to the brain.
- Sound is picked up by a microphone worn near the ear. This sound is sent to a speech processor, which is most often connected to the microphone and worn behind the ear.
- The sound is analyzed and converted into electrical signals, which are sent to a surgically implanted receiver behind the ear. This receiver sends the signal through a wire into the inner ear.
- From there, the electrical impulses are sent to the brain.
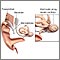
HOW IT IS IMPLANTED
To have the surgery:
- You will receive general anesthesia so you will be asleep and pain free.
- A surgical cut is made behind the ear, sometimes after shaving part of the hair behind the ear.
- A microscope and bone drill are used to open the bone behind the ear (mastoid bone) to allow the inside part of the implant to be inserted.
- The electrode array is passed into the inner ear (cochlea).
- The receiver is placed into a pocket created behind the ear. The pocket helps keep it in place and makes sure it is close enough to the skin to allow electrical information to be sent from the device. A well may be drilled into the bone behind the ear so the implant is less likely to move under the skin.
After surgery:
- There will be stitches behind the ear.
- You may be able to feel the receiver as a bump behind the ear.
- Any shaved hair should grow back.
- The outside part of the device will be placed 1 to 4 weeks after surgery to give the opening time to heal.
RISKS OF SURGERY
A cochlear implant is a relatively safe surgery. However, all surgeries pose some risks. Risks are less common now that the surgery is performed through a small surgical cut, but may include:
- Wound healing problems
- Skin breakdown over the implanted device
- Infection near the implant site
Less common complications include:
- Damage to the nerve that moves the face on the side of the operation
- Leakage of the fluid around the brain (cerebrospinal fluid)
- Infection of the fluid around the brain (meningitis)
- Temporary dizziness (vertigo)
- Failure of the device to work
- Abnormal taste
RECOVERY AFTER SURGERY
You may be admitted to the hospital overnight for observation. However, many hospitals now allow people to go home the day of surgery. Your surgeon will give you pain medicines and sometimes antibiotics to prevent infection. Many surgeons place a large dressing over the operated ear. The dressing is removed the day after surgery.
A week or more after surgery, the outside part of the cochlear implant is secured to the receiver-stimulator that was implanted behind the ear. At this point, you will be able to use the device.
Once the surgery site is well healed, and the implant is attached to the outside processor, you will begin to work with specialists to learn to "hear" and process sound using the cochlear implant. These specialists may include:
- Audiologists
- Speech therapists
- ENT doctors
This is a very important part of the process. You will need to work closely with your team of specialists to get the most benefit from the implant.
OUTLOOK
Results with cochlear implants vary widely. How well you do depends on:
- The condition of your hearing nerve before surgery
- Your mental abilities
- The device being used
- The length of time you were deaf
- The surgery
Some people can learn to communicate on the telephone. Others can only recognize sound. Getting the maximum results can take up to several years, and you need to be motivated. Many people are enrolled in hearing and speech rehabilitation programs.
LIVING WITH AN IMPLANT
Once you have healed, there are few restrictions. Most activities are allowed. However, your health care provider or surgeon may tell you to avoid contact sports to lessen the chance of injury to the implanted device.
Most people with cochlear implants cannot get MRI scans, because the implant is made of metal.
Alternative Names
Hearing loss - cochlear implant; Sensorineural - cochlear; Deaf - cochlear; Deafness - cochlear
Images
References
National Institute for Health and Care Excellence (NICE) website. Cochlear implants for children and adults with severe to profound deafness. Technology appraisal guidance. www.nice.org.uk/guidance/ta566. Published March 7, 2019. Accessed May 3, 2025.
Roland JL, Ray WZ, Leuthardt EC. Neuroprosthetics. In: Winn HR, ed. Youmans and Winn Neurological Surgery. 8th ed. Philadelphia, PA: Elsevier; 2023:chap 132.
Vohr BR. Hearing loss in the newborn infant. In: Martin RJ, Fanaroff AA, eds. Fanaroff and Martin's Neonatal-Perinatal Medicine. 12th ed. Philadelphia, PA: Elsevier; 2025:chap 61.
Wackym PA, Hirce KJ, Bernknopf HJ, Francis HW. Cochlear implantation: patient evaluation and device selection. In: Flint PW, Francis HW, Haughey BH, et al, eds. Cummings Otolaryngology: Head and Neck Surgery. 7th ed. Philadelphia, PA: Elsevier; 2021:chap 160.
Review Date 4/3/2025
Updated by: Ashutosh Kacker, MD, FACS, Professor of Clinical Otolaryngology, Weill Cornell Medical College, and Attending Otolaryngologist, New York-Presbyterian Hospital, New York, NY. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.