The triglyceride level is a blood test to measure the amount of triglycerides in your blood. Triglycerides are a type of fat.
Your body makes some triglycerides. Triglycerides also come from the food you eat. Extra calories are turned into triglycerides and stored in fat cells for later use.
A test for high blood cholesterol levels is a related measurement and usually done at the same time.
How the Test is Performed
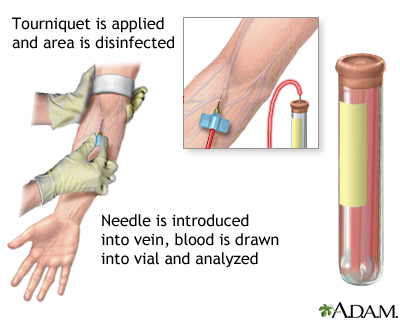
A blood sample is needed. Most of the time, blood is drawn from a vein located on the inside of the elbow or the back of the hand.
How to Prepare for the Test
You should not eat for 8 to 12 hours before the test.
Alcohol and some medicines can interfere with blood test results.
- Make sure your health care provider knows what medicines you take, including non-prescription medicines, drugs and supplements.
- Your provider will tell you if you need to stop taking any medicines before you have this test.
- Do not stop or change your medicines without talking to your provider first.
How the Test will Feel
You may feel slight pain or a sting when the needle is inserted. You may also feel some throbbing at the site after the blood is drawn.
Why the Test is Performed
Triglycerides are usually measured together with other blood fats. Often it is done to help determine your risk of developing heart disease. A high triglyceride level may lead to atherosclerosis, which increases your risk for heart attack and stroke.
A very high triglyceride level may also cause inflammation of your pancreas (called pancreatitis).
Normal Results
Results may indicate:
- Normal: Less than 150 mg/dL (1.69 mmol/L)
- Borderline high: 150 to 199 mg/dL (1.69 to 2.25 mmol/L)
- High: 200 to 499 mg/dL (2.26 to 5.64 mmol/L)
- Very high: 500 mg/dL or above (5.65 mmol/L)
Normal value ranges may vary slightly among different labs. Talk to your provider about the meaning of your specific test results.
The examples above show the common measurements for results for these tests. Some labs use different measurements or may test different specimens.
What Abnormal Results Mean
High triglyceride levels may be due to:
- Cirrhosis or liver damage
- Diet low in protein and high in carbohydrates
- Underactive thyroid
- Nephrotic syndrome (a kidney disorder)
- Other medicines, such as female hormones
- Poorly controlled diabetes
- Disorder passed down through families in which there are high amounts of cholesterol and triglycerides in the blood
Overall, the treatment of elevated triglyceride levels focuses on increased exercise and changes in the diet. Medicines to lower triglyceride levels may be used to prevent pancreatitis for levels above 500 mg/dL.
Low triglyceride levels may be due to:
- Low fat diet
- Hyperthyroidism (overactive thyroid)
- Malabsorption syndrome (conditions in which the small intestine does not absorb fats well)
- Malnutrition
Considerations
Pregnancy can affect test results.
Alternative Names
Triacylglycerol test
Images
References
Arnett DK, Blumenthal RS, Albert MA, et al. 2019 ACC/AHA guideline on the primary prevention of cardiovascular disease: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Circulation. 2019;140(11):e596-e646. PMID: 30879355 pubmed.ncbi.nlm.nih.gov/30879355/.
Bredefeld CL, Lau R, Hussain MM. Lipids and dyslipoproteinemia. In: McPherson RA, Pincus MR, eds. Henry's Clinical Diagnosis and Management by Laboratory Methods. 24th ed. Philadelphia, PA: Elsevier; 2022:chap 18.
Grundy SM, Stone NJ, Bailey AL, et al. 2018 AHA/ACC/AACVPR/AAPA/ABC/ACPM/ADA/AGS/APhA/ASPC/NLA/PCNA Guideline on the management of blood cholesterol: executive summary: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Circulation. 2019;139(25):e1046-e1081. PMID: 30565953 pubmed.ncbi.nlm.nih.gov/30565953/.
Mora S, Libby P, Ridker PM. Primary prevention of cardiovascular disease. In: Bonow RO, Mann DL, Tomaselli GF, et al, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine. 13th ed. Philadelphia, PA: Elsevier; 2026:chap 23.
Robinson JG. Disorders of lipid metabolism. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 190.
Tokgözoglu L, Libby P. Lipoprotein disorders and cardiovascular disease. In: Bonow RO, Mann DL, Tomaselli, GF, et al, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine. 13th ed. Philadelphia, PA: Elsevier; 2026:chap 25.
Review Date 7/14/2024
Updated by: Michael A. Chen, MD, PhD, Associate Professor of Medicine, Division of Cardiology, Harborview Medical Center, University of Washington Medical School, Seattle, WA. Internal review and update on 07/01/2025 by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.