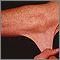
Ehlers-Danlos syndrome (EDS) is a group of inherited disorders marked by extremely loose joints, very stretchy (hyperelastic) skin that bruises easily, and easily damaged blood vessels.
Causes
There are at least 13 types of EDS. Hypermobile EDS is the most common type (90% of cases). Other forms include the classic and vascular forms.
A variety of gene variations cause problems with collagen. This is the material that provides strength and structure to:
- Skin
- Bone
- Blood vessels
- Internal organs
The variant collagen leads to the symptoms associated with EDS. In some forms of the syndrome, the rupture of internal organs or abnormal heart valves can occur.
Family history is a risk factor in some cases.
Symptoms
Symptoms of EDS vary by type and may include:
- Back pain
- Double-jointedness
- Easily damaged, bruised, and stretchy skin
- Easy scarring and poor wound healing
- Flat feet
- Increased joint mobility, joints popping, early arthritis
- Joint dislocation
- Joint pain
- Premature rupture of membranes during pregnancy
- Very soft and velvety skin
- Vision problems
Exams and Tests
An exam by your health care provider may show:
- Deformed surface of the eye (cornea)
- Excess joint looseness and joint hypermobility
- Mitral valve in the heart does not close tightly (mitral valve prolapse)
- Gum infection (periodontitis)
- Rupture of intestines, uterus, or eyeball (seen only in vascular EDS, which is rare)
- Soft, thin, or very stretchy skin
Tests to diagnose EDS include:
- Collagen typing (performed on a skin biopsy sample)
- Collagen gene variation testing for some types of EDS
- Echocardiogram (heart ultrasound)
- Lysyl hydroxylase or oxidase activity (to check collagen formation)
Treatment
There is no specific cure for EDS. Individual problems and symptoms are evaluated and cared for appropriately. Physical therapy or an evaluation by a specialist in rehabilitation medicine is often needed.
Support Groups
More information and support for people with Ehlers-Danlos and their families can be found at:
The Ehlers-Danlos Society -- www.ehlers-danlos.com/support/
Outlook (Prognosis)
People with EDS generally have a normal life span. Intelligence is normal.
Those with the rare vascular type of EDS are at greater risk for rupture of a major organ or blood vessel. These people have a high risk for sudden death.
Possible Complications
Possible complications of EDS include:
- Chronic joint pain
- Early-onset arthritis
- Failure of surgical wounds to close (or stitches tear out)
- Premature rupture of membranes during pregnancy
- Rupture of major vessels, including a ruptured aortic aneurysm (only in vascular EDS)
- Rupture of a hollow organ such as the uterus or bowel (only in vascular EDS)
- Rupture of the eyeball (only in vascular EDS)
When to Contact a Medical Professional
Contact your provider for an appointment if you have a family history of EDS and you are concerned about your risk or are planning to start a family.
Contact your provider for an appointment if you or your child has symptoms of EDS.
Prevention
Genetic counseling is recommended for prospective parents with a family history of EDS. Those planning to start a family should be aware of the type of EDS they have and how it is passed down to children. This can be determined through testing and evaluations suggested by your provider or genetic counselor.
Identifying any significant health risks may help prevent severe complications by vigilant screening and lifestyle alterations.
References
Basel D. Ehlers-Danlos syndrome. In: Kliegman RM, St. Geme JW, Blum NJ, et al, eds. Nelson Textbook of Pediatrics. 22nd ed. Philadelphia, PA: Elsevier; 2025:chap 744.
Bober NP-H, Michael B, Krakow D. Heritable diseases of connective tissue. In: Firestein GS, McInnes IB, Koretzky GA, Mikuls TR, Neogi T, O'Dell JR, eds. Firestein & Kelly's Textbook of Rheumatology. 12th ed. Philadelphia, PA: Elsevier; 2025:chap 107.
Pyeritz RE. Inherited diseases of connective tissue. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 239.
Review Date 11/6/2024
Updated by: Anna C. Edens Hurst, MD, MS, Associate Professor in Medical Genetics, The University of Alabama at Birmingham, Birmingham, AL. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.