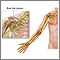
Brachial plexopathy is a form of peripheral neuropathy. It occurs when there is damage to the brachial plexus. This is a group of nerves that run from the lower neck through the upper shoulder area. These nerves provide the shoulder, arm, and hand with movement and sensation through the radial, median, and ulnar nerves.
Damage to the nerves of the brachial plexus results in pain, decreased movement, or decreased feeling in the arm and shoulder.
Causes
Damage to the brachial plexus may occur due to:
- Direct injury to the nerve
- Stretching injuries (including birth trauma)
- Pressure from tumors in the area (especially from lung tumors)
- Damage from radiation therapy
Brachial plexus dysfunction may also be associated with:
- Birth defects that put pressure on the neck area
- Exposure to toxins, chemicals, or medicines and illegal drugs
- General anesthesia, used during surgery
- Inflammatory conditions, such as those due to a virus or immune system problem
- Hereditary causes, such as hereditary neuralgic amyotrophy
In some cases, no cause can be identified.
Symptoms
Symptoms may include:
- Numbness of the shoulder, arm, or hand
- Shoulder pain
- Tingling, burning, pain, or abnormal sensations (location depends on the area injured)
- Weakness of the shoulder, arm, hand, or wrist
Exams and Tests
An exam of the arm, hand and wrist can reveal a problem with the nerves of the brachial plexus. Signs may include:
- Deformity of the arm or hand
- Difficulty moving the shoulder, arm, hand, or fingers
- Diminished arm reflexes
- Wasting of the muscles
- Weakness of hand flexing
A detailed history may help determine the cause of the brachial plexopathy. Age and sex are important, because some brachial plexus problems are more common in certain groups. For example, young men more often have inflammatory or post-viral brachial plexus disease called Parsonage-Turner syndrome.
Tests that may be done to diagnose this condition include:
- Blood tests
- Chest x-ray
- Electromyography (EMG) to check the muscles and nerves that control the muscles
- MRI of the head, neck, and shoulder
- Nerve conduction to check how fast electrical signals move through a nerve
- Nerve biopsy to examine a piece of nerve under the microscope (rarely needed)
- Ultrasound
- Genetic tests to look for hereditary causes of neuropathy
Treatment
Treatment is aimed at correcting the underlying cause and allowing you to use your hand and arm as much as possible. In some cases, no treatment is needed and the problem gets better on its own.
Treatment options include any of the following:
- Medicines to control pain
- Physical therapy to help maintain muscle strength
- Braces, splints, or other devices to help you use your arm
- Nerve block, in which medicine is injected into the area near the nerves to reduce pain
- Surgery to repair the nerves or remove something pressing on the nerves
You may need occupational therapy or counseling to suggest changes in the workplace.
Medical conditions such as diabetes and kidney disease can damage nerves. In these cases, treatment is also directed at the underlying medical condition.
Outlook (Prognosis)
A good recovery is possible if the cause is found and properly treated. In some cases, there is partial or complete loss of movement or sensation. Nerve pain may be severe and may last for a long time.
Possible Complications
Complications may include:
- Deformity of the hand or arm, mild to severe, which can lead to contractures
- Partial or complete arm paralysis
- Partial or complete loss of sensation in the arm, hand, or fingers
- Recurrent or unnoticed injury to the hand or arm due to diminished sensation
When to Contact a Medical Professional
Contact your health care provider if you experience pain, numbness, tingling, or weakness in the shoulder, arm, or hand.
Alternative Names
Neuropathy - brachial plexus; Brachial plexus dysfunction; Parsonage-Turner syndrome; Pancoast syndrome
References
Chad DA, Bowley MP. Disorders of nerve roots and plexuses. In: Jankovic J, Mazziotta JC, Pomeroy SL, Newman NJ, eds. Bradley and Daroff's Neurology in Clinical Practice. 8th ed. Philadelphia, PA: Elsevier; 2022:chap 105.
Waldman SD. Cervicothoracic interspinous bursitis. In: Waldman SD, ed. Atlas of Uncommon Pain Syndromes. 4th ed. Philadelphia, PA: Elsevier; 2020:chap 23.
Review Date 6/13/2024
Updated by: Joseph V. Campellone, MD, Department of Neurology, Cooper Medical School at Rowan University, Camden, NJ. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.