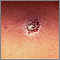
Leishmaniasis is an infectious disease spread by the bite of the female sandfly.
Causes
Leishmaniasis is caused by a tiny parasite called leishmania protozoa. Protozoa are one-celled organisms.
The different forms of leishmaniasis are:
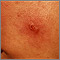
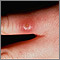
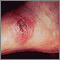
- Cutaneous leishmaniasis affects the skin and mucous membranes. Skin sores usually start at the site of the sandfly bite. In a few people, sores may develop on mucous membranes.
- Systemic, or visceral, leishmaniasis affects the entire body. This form occurs 2 to 8 months after a person is bitten by the sandfly. Most people do not remember having a skin sore. This form can lead to deadly complications. The parasites damage the immune system by decreasing the number of disease-fighting cells.
Cases of leishmaniasis have been reported on all continents except Australia and Antarctica. In the Americas, the disease can be found in Mexico and South America. It has also been reported in military personnel who have returned from the Persian Gulf.
Symptoms
Symptoms of cutaneous leishmaniasis depend on where the lesions are located and may include:
- Skin sores, which may become a skin ulcer that heals very slowly
- Stuffy nose, runny nose, and nosebleeds
- Ulcers and wearing away (erosion) in the mouth, tongue, gums, lips, nose, and inner nose
Systemic visceral infection in children usually begins suddenly with:
- Cough
- Fever
Adults usually have a fever for 2 weeks to 2 months, along with symptoms such as fatigue, weakness, and appetite loss. Weakness increases as the disease gets worse.
Other symptoms of systemic visceral leishmaniasis may include:
- Abdominal discomfort
- Fever that lasts for weeks; may come and go in cycles
- Night sweats
- Scaly, gray, dark, ashen skin
- Thinning hair
- Weight loss
Exams and Tests
Your health care provider will examine you and may find that your spleen, liver, and lymph nodes are enlarged. You will be asked if you recall being bitten by sandflies or if you've been in an area where leishmaniasis is common.
Tests that may be done to diagnose the condition include:
- Biopsy of the spleen and culture
- Bone marrow biopsy and culture
- Direct agglutination assay
- Indirect immunofluorescent antibody test
- Leishmania-specific PCR test
- Liver biopsy and culture
- Lymph node biopsy and culture
- Montenegro skin test (not approved in the United States)
- Skin biopsy and culture
Other tests that may be done include:
- Complete blood count with differential
- Serologic testing
- Serum albumin
- Serum immunoglobulin levels
- Serum protein
Treatment
Antimony-containing compounds are the main medicines used to treat leishmaniasis. These include:
- Meglumine antimoniate
- Sodium stibogluconate
Other medicines that may be used include:
- Amphotericin B
- Ketoconazole
- Miltefosine
- Paromomycin
- Pentamidine
Plastic surgery may be needed to correct the disfigurement caused by sores on the face (cutaneous leishmaniasis).
Outlook (Prognosis)
Cure rates are high with the proper medicine, mostly when treatment is started before it affects the immune system. Cutaneous leishmaniasis may lead to disfigurement.
Death is usually caused by complications (such as other infections), rather than from the disease itself. Death often occurs within 2 years.
Possible Complications
Leishmaniasis may lead to the following:
- Bleeding (hemorrhage)
- Deadly infections due to immune system damage
- Disfigurement of the face
When to Contact a Medical Professional
Contact your provider if you have symptoms of leishmaniasis after visiting an area where the disease is known to occur.
Prevention
Taking measures to avoid sandfly bites can help prevent leishmaniasis:
- Putting fine mesh netting around the bed (in areas where the disease occurs)
- Screening windows
- Wearing insect repellent
- Wearing protective clothing
Public health measures to reduce sandflies are important. There are no vaccines or medicines that prevent leishmaniasis.
Alternative Names
Kala-azar; Cutaneous leishmaniasis; Visceral leishmaniasis; Old world leishmaniasis; New world leishmaniasis
References
Aronson NE, Copeland NK. Leishmania species: visceral, cutaneous, and mucosal leishmaniasis. In: Blaser MJ, Cohen JI, Holland SM, et al, eds. Mandell, Douglas, and Bennett's Principles and Practice of Infectious Diseases. 10th ed. Philadelphia, PA: Elsevier; 2026:chap 281.
Buffet PA, Croft SL, Chatterjee M. Leishmaniasis. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 319.
Dinulos JGH. Infestations and bites. In: Dinulos JGH, ed. Habif's Clinical Dermatology. 7th ed. Philadelphia, PA: Elsevier; 2021:chap 15.
Review Date 8/5/2025
Updated by: Jatin M. Vyas, MD, PhD, Roy and Diana Vagelos Professor in Medicine, Columbia University Vagelos College of Physicians and Surgeons, Division of Infectious Diseases, Department of Medicine, New York, NY. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.