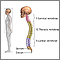
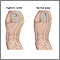
Kyphosis is a curving of the spine that causes a bowing or rounding of the back. This leads to a hunchback or slouching posture.
Causes
Kyphosis can occur at any age, although it is rare at birth.
A type of kyphosis that occurs in young teens is known as Scheuermann disease. It is caused by the wedging together of several bones of the spine (vertebrae) in a row. The cause of this condition is unknown. Kyphosis can also occur in young teens who have cerebral palsy.
In adults, kyphosis can be caused by:
- Degenerative diseases of the spine (such as arthritis or disk degeneration)
- Fractures caused by osteoporosis (osteoporotic compression fractures)
- Injury (trauma)
- Slipping of one vertebra forward on another (spondylolisthesis)
- Previous surgeries or fusion on the spine
Other causes of kyphosis include:
- Certain hormone (endocrine) diseases
- Connective tissue disorders
- Infection (such as tuberculosis)
- Muscular dystrophy (group of inherited disorders that cause muscle weakness and loss of muscle tissue)
- Neurofibromatosis (disorder in which nerve tissue tumors form)
- Paget disease (disorder that involves abnormal bone destruction and regrowth)
- Polio
- Scoliosis (curving of the spine often looks like a C or S when viewed from behind)
- Spina bifida (birth defect in which the backbone and spinal canal don't close before birth)
- Tumors of the spine or the area nearby
Symptoms
Pain in the middle or lower back is the most common symptom. Other symptoms may include any of the following:
- Round back appearance
- Tenderness and stiffness in the spine
- Fatigue
- Difficulty breathing (in severe cases)
Exams and Tests
A physical exam by your health care provider can confirm the abnormal curve of the spine. Your provider will also look for any nervous system (neurological) changes. These include weakness, paralysis, or changes in sensation below the curve. Your provider will also check for differences in your reflexes.
Tests that may be ordered include:
- Spine x-ray
- Pulmonary function tests (if kyphosis affects breathing)
- MRI of the spine (if there may be a tumor, infection, or nervous system symptoms)
- Bone density test (to check for osteoporosis)
Treatment
Treatment depends on the cause of the disorder:
- Congenital kyphosis needs corrective surgery at an early age.
- Scheuermann disease is treated with a brace and physical therapy. Sometimes surgery is needed for large (greater than 60 degrees), painful curves.
- Compression fractures from osteoporosis can be left alone if there are no nervous system problems or pain. But the osteoporosis needs to be treated to help prevent future fractures. For severe deformity or pain from osteoporosis, surgery is an option.
- Kyphosis caused by infection or tumor needs prompt treatment, often with surgery and medicines.
Treatment for other types of kyphosis depends on the cause. Surgery is needed if nervous system symptoms or constant pain develop.
Outlook (Prognosis)
Young teens with Scheuermann disease tend to do well, even if they need surgery. The disease stops once they stop growing. If the kyphosis is due to degenerative joint disease or multiple compression fractures, surgery is needed to correct the defect and improve pain.
Possible Complications
Untreated kyphosis can cause any of the following:
- Decreased lung capacity
- Disabling back pain
- Nervous system symptoms, including leg weakness or paralysis
- Round back deformity
- Increased self-consciousness or body awareness
Prevention
Treating and preventing osteoporosis can prevent many cases of kyphosis in older adults. Early diagnosis and bracing for Scheuermann disease can reduce the need for surgery, but there is no way to prevent the disease.
Alternative Names
Scheuermann disease; Roundback; Hunchback; Postural kyphosis; Neck pain - kyphosis
Images
References
Magee DJ, Manske RC. Thoracic (dorsal) spine. In: Magee DJ, Manske RC, eds. Orthopedic Physical Assessment. 7th ed. Philadelphia, PA: Elsevier; 2021:chap 8.
McClincy MP, Olgun ZD, Dede O. Orthopedics. In: Zitelli BJ, McIntire SC, Nowalk AJ, Garrison J, eds. Zitelli and Davis' Atlas of Pediatric Physical Diagnosis. 8th ed. Philadelphia, PA: Elsevier; 2023:chap 22.
Warner WC, Sawyer JR. Scoliosis and kyphosis. In: Azar FM, Beaty JH, eds. Campbell's Operative Orthopaedics. 14th ed. Philadelphia, PA: Elsevier; 2021:chap 44.
Review Date 8/27/2024
Updated by: C. Benjamin Ma, MD, Professor, Chief, Sports Medicine and Shoulder Service, UCSF Department of Orthopaedic Surgery, San Francisco, CA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.