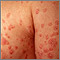
Guttate psoriasis is a skin condition in which small, red, scaly, teardrop-shaped spots with silvery scale appear on the arms, legs, and middle of the body. Gutta means "drop" in Latin.
Causes
Guttate psoriasis is a type of psoriasis. Guttate psoriasis is usually seen in people younger than 30, especially in children. The condition often develops suddenly. It usually appears after an infection, most notably strep throat caused by group A streptococcus. Guttate psoriasis is not contagious. This means it can't spread to other people.
Psoriasis is a common disorder. The exact cause isn't known. But health care providers think genes and the immune system are involved. Certain things can trigger an attack of symptoms.
With guttate psoriasis, in addition to strep throat, the following may trigger an attack:
- Bacterial or viral infections, including upper respiratory infections
- Injury to the skin, including cuts, burns, and insect bites
- Some medicines, including those used to treat malaria and certain heart conditions
- Stress
- Sunburn
- Too much alcohol
Psoriasis may be severe in people who have a weakened immune system. This may include people who have:
- HIV/AIDS
- Autoimmune disorders, including rheumatoid arthritis
- Taken chemotherapy for cancer
Symptoms
Symptoms may include:
- Itching
- Spots on the skin that are pinkish-red and look like teardrops
- Spots may be covered with silver, flaky skin called scales
- Spots usually occur on the arms, legs, and middle of the body (the trunk), but may appear in other body areas
Exams and Tests
Your provider will look at your skin. The diagnosis is usually based on what the spots look like.
Often, a person with guttate psoriasis has recently had a sore throat or upper respiratory infection.
Tests to confirm the diagnosis may include:
- Skin biopsy
- Throat culture
- Blood tests for recent exposure to strep bacteria
Treatment
If you are recently infected with group A strep, your provider may give you antibiotics.
Mild cases of guttate psoriasis are usually treated at home. Your provider may recommend any of the following:
- Cortisone or other anti-itch and anti-inflammatory creams
- Dandruff shampoos (over-the-counter or prescription)
- Lotions that contain coal tar
- Moisturizers
- Prescription medicines that have vitamin D to apply to the skin (topically) or that have vitamin A (retinoids) to take by mouth (orally)
People with severe guttate psoriasis may receive medicines to suppress the body's immune response. These include cyclosporine and methotrexate. A newer group of medicines called biologics that alter parts of the immune system may also be used.
Your provider may suggest phototherapy. This is a medical procedure in which your skin is carefully exposed to ultraviolet light. Phototherapy may be given alone or after you take a medicine that makes the skin sensitive to light.
Outlook (Prognosis)
Guttate psoriasis may clear up completely following treatment, especially phototherapy treatment. Sometimes, it may become a chronic (lifelong) condition, or worsen to the more common plaque-type psoriasis.
When to Contact a Medical Professional
Contact your provider if you have symptoms of guttate psoriasis.
Alternative Names
Psoriasis - guttate; Group A streptococcus - guttate psoriasis; Strep throat - guttate psoriasis
References
Dinulos JGH. Psoriasis and other papulosquamous diseases. In: Dinulos JGH, ed. Habif's Clinical Dermatology. 7th ed. Philadelphia, PA: Elsevier; 2021:chap 8.
James WD. Papulosquamous, pustular and keratotic disorders. In: James WD, ed. Andrews' Diseases of the Skin. 14th ed. Philadelphia, PA: Elsevier; 2026:chap 10.
Review Date 4/1/2025
Updated by: Elika Hoss, MD, Assistant Professor of Dermatology, Mayo Clinic, Scottsdale, AZ. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.