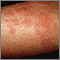
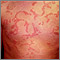
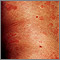
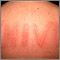
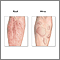
Allergic reactions are sensitivities to substances called allergens that come into contact with the skin, nose, eyes, respiratory tract, and gastrointestinal tract. Allergens can be breathed into the lungs, swallowed, or injected.
Considerations
Allergic reactions are common. The immune response that causes an allergic reaction is similar to the response that causes hay fever. Most reactions happen soon after contact with an allergen.
Many allergic reactions are mild, while others can be severe and life threatening. They can be confined to a small area of the body, or they may affect the entire body. The most severe form is called anaphylaxis or anaphylactic shock. Allergic reactions occur more often in people who have a family history of allergies.
Substances that don't bother most people (such as venom from bee stings and certain foods, medicines, and pollens) can trigger allergic reactions in certain people.
First-time exposure may produce only a mild reaction. Repeated exposures may lead to more serious reactions. Once a person has had an exposure or an allergic reaction (and thus is sensitized to an allergen), even a very limited exposure to a very small amount of allergen can trigger a reaction.
Most severe allergic reactions occur within seconds or minutes after exposure to the allergen. Some reactions can occur after several hours. In very rare cases, reactions develop after 24 hours.
Anaphylaxis is a sudden and severe allergic reaction that occurs within minutes or hours of exposure. Immediate medical attention is needed for this condition. Without treatment, anaphylaxis can get worse very quickly and lead to death within 15 minutes.
Causes
Common allergens include:
- Animal dander
- Bee stings or stings from other insects such as fire ants
- Dust
- Foods, especially milk, eggs, peanuts, tree nuts, fish, and shellfish
- Medicines
- Mold
- Pollens
Symptoms
Common symptoms of a mild allergic reaction include:
Symptoms of a moderate or severe reaction include:
- Abdominal pain
- Abnormal (high-pitched) breathing sounds
- Anxiety
- Chest discomfort or tightness
- Cough
- Diarrhea
- Difficulty breathing (wheezing)
- Difficulty swallowing
- Dizziness or lightheadedness
- Flushing or redness of the face
- Hives all over
- Nausea or vomiting
- Palpitations
- Swelling of the face, eyes, or tongue
- Unconsciousness
First Aid
For a mild to moderate reaction:
Calm and reassure the person having the reaction. Anxiety can make symptoms worse.
Try to identify the allergen and have the person avoid further contact with it.
- If the person develops an itchy rash, apply cool compresses and an over-the-counter hydrocortisone cream.
- Watch the person for signs of increasing distress.
- Get medical help. For a mild reaction, your health care provider may recommend over-the-counter medicines, such as antihistamines.
For a severe allergic reaction (anaphylaxis):
Check the person's airway, breathing, and circulation (the ABC's of Basic Life Support). A warning sign of dangerous throat swelling is a very hoarse or whispered voice, or coarse sounds when the person is breathing in air. If necessary, begin rescue breathing and CPR.
- Call 911 or the local emergency number.
- Calm and reassure the person.
- If the allergic reaction is from a bee sting, scrape the stinger off the skin with something firm (such as a fingernail or plastic credit card). Do not use tweezers -- squeezing the stinger will release more venom.
- If the person has injectable or intranasal emergency allergy medicine (Epinephrine), administer it at the beginning of a reaction. Do not wait to see if the reaction gets worse. Avoid oral medicine if the person is having difficulty breathing.
- Take steps to prevent shock. Have the person lie flat, raise the person's feet about 12 inches (in) or 30 centimeters (cm), and cover them with a coat or blanket. Do not place the person in this position if a head, neck, back, or leg injury is suspected, if it causes discomfort, or if the person is vomiting.
DO NOT
If a person is having an allergic reaction:
- Do not assume that any allergy shots the person has already received will provide complete protection.
- Do not place a pillow under the person's head if he or she is having trouble breathing. This can block the airways.
- Do not give the person anything by mouth if the person is having trouble breathing.
When to Contact a Medical Professional
Contact 911 or the local emergency number for medical assistance right away if:
- The person is having a severe allergic reaction. Do not wait to see if the reaction is getting worse.
- The person has a history of severe allergic reactions (check for a medical ID tag).
Prevention
To prevent allergic reactions:
- Avoid triggers such as foods and medicines that have caused an allergic reaction in the past. Ask detailed questions about ingredients when you are eating away from home. Carefully check ingredient labels.
- If you have a child who is allergic to certain foods, introduce one new food at a time in small amounts so you can recognize an allergic reaction.
- People who have had serious allergic reactions should wear a medical ID tag and carry emergency medicines such as a two-pack of injectable or intranasal epinephrine, according to their provider's instructions.
- There is no contraindication to using epinephrine in a severe allergic reaction.
Alternative Names
Anaphylaxis; Anaphylaxis - first aid
References
Barksdale AN, Ross W. Allergy, anaphylaxis, and angioedema. In: Walls RM, ed. Rosen's Emergency Medicine: Concepts and Clinical Practice. 10th ed. Philadelphia, PA: Elsevier; 2023:chap 106.
Custovic A, Tovey E. Allergen control for prevention and management of allergic diseases. In: Burks AW, Holgate ST, O'Hehir RE, et al, eds. Middleton's Allergy: Principles and Practice. 9th ed. Philadelphia, PA: Elsevier; 2020:chap 84.
Nadeau KC. Approach to the patient with allergic or immunologic disease. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 230.
Wang J, Lieberman JA, Wallace DV, Waserman S, Golden DBK. Anaphylaxis in practice: a guide to the 2023 practice parameter update. J Allergy Clin Immunol Pract. 2024;12(9):2325-2336. PMID: 38944199 pubmed.ncbi.nlm.nih.gov/38944199/.
Review Date 1/20/2026
Updated by: Deborah Pedersen, MD, MS, Allergy & Asthma Care, PC, Taunton, MA. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.