Speaking is a key part of communicating with people. Having a tracheostomy tube can change your ability to talk and interact with others.
However, you can learn how to speak with a tracheostomy tube. It just takes practice. There are even speaking devices that can help you.
Tracheostomy Tubes and Speaking
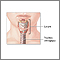
Air passing through your vocal cords (larynx) causes them to vibrate, creating sounds and speech.
A tracheostomy tube blocks most of the air from passing through your vocal cords. Instead, your breath (air) goes out through your tracheostomy tube (trach).
At the time of your surgery, the first trach tube will have a balloon (cuff) that lies in your trachea.
- If the cuff is inflated (filled with air), it will prevent air from moving through your vocal cords. This will stop you from making noise or speech.
- If the cuff is deflated, the air is able to move around the trach and through your vocal cords, and you should be able to make sounds. However, most of the time the trach tube is changed after 5 to 7 days to a smaller, cuffless trach. This makes speaking much easier.
Practicing
If your tracheostomy has a cuff, it will need to be deflated. Your health care provider and caregiver should make the decision about when to deflate your cuff.
When the cuff is deflated and air can pass around your trach, you should try to talk and make sounds.
Speaking will be harder than before you had your trach. You may need to use more force to push the air out through your mouth. To speak:
- Take a deep breath in.
- Breathe out, using more force than you normally would to push the air out.
- Close off the trach tube opening with your finger and then speak.
- You may not hear much at first.
- You will build up the strength to push the air out through your mouth as you practice.
- The sounds you make will get louder.
In order to speak, it is important that you place a clean finger over the trach to prevent air from exiting through the trach. This will help the air go out through your mouth to make your voice.
Speaking Valves
If it is hard to speak with a trach in place, special devices can help you learn to create sounds.
One-way valves, called speaking valves, are placed onto your tracheostomy. Speaking valves allow air to enter through the tube and exit through your mouth and nose. This will allow you to make noises and speak more easily without needing to use your finger to block your trach each time you talk.
Some patients may not be able to use these valves. The speech therapist will work with you to ensure you are a good candidate. If a speaking valve is placed on your trach, and you have trouble breathing, the valve may not be allowing enough air to pass around your trach.
Other Factors to Think About
The width of the tracheostomy tube may play a role. If the tube takes up too much space in your throat, there may not be enough room for the air to pass around the tube.
Your trach may be fenestrated. This means the trach has extra holes built into it. These holes allow air to pass through your vocal cords. They can make it easier to eat and breathe with a tracheostomy tube.
It may take much longer to develop speech if you have:
- Vocal cord damage
- Injury to the vocal cord nerves, which can change the way the vocal cords move
- Airway damage from factors that created the need for the tracheostomy
Alternative Names
Trach - speaking
Images
References
Dobkin BH. Neurological rehabilitation. In: Jankovic J, Mazziotta JC, Pomeroy SL, Newman NJ, eds. Bradley and Daroff's Neurology in Clinical Practice. 8th ed. Philadelphia, PA: Elsevier; 2022:chap 55.
Greenwood JC, Winters ME. Tracheostomy care. In: Birnbaumer DM, ed. Roberts and Hedges' Clinical Procedures in Emergency Medicine and Acute Care. 8th ed. Philadelphia, PA: Elsevier; 2026:chap 7.
Review Date 10/15/2025
Updated by: James L. Demetroulakos, MD, F.A.C.S., Department of Otolaryngology, North Shore Medical Center, Salem, MA. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.