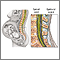
Spinal and epidural anesthesia are procedures that deliver medicines that numb parts of your body to block pain. They are given through shots in or around the spine.
Description
A health care provider who gives you epidural or spinal anesthesia is called an anesthesiologist. In some situations, this may be administered by a certified registered nurse anesthetist.
First, the area of your back where the needle is inserted is cleaned with a special solution. The area may also be numbed with a local anesthetic.
You'll likely receive fluids through an intravenous line (IV) in a vein. You may receive medicine through the IV to help you relax.
For an epidural:
- Your provider injects medicine just outside of the sac of fluid around your spinal cord. This is called the epidural space.
- The medicine numbs, or blocks, feeling in a certain part of your body so that you either feel less pain or no pain at all depending on the procedure. The medicine begins to take effect in about 10 to 20 minutes. It works well for longer procedures. Women often have an epidural during childbirth.
- A small tube (catheter) is often left in place. You can receive more medicine through the catheter to help control your pain during or after your procedure.
For a spinal:
- Your provider injects medicine into the fluid around your spinal cord. This is usually done only once, so you will not need to have a catheter placed.
- The medicine begins to take effect right away.
Your pulse, blood pressure, and oxygen level in your blood are checked during the procedure. After the procedure, you will have a bandage where the needle was inserted.
Why the Procedure is Performed
Spinal and epidural anesthesia work well for certain procedures and do not require placing a breathing tube into the windpipe (trachea). People usually recover their senses much faster. Sometimes, they have to wait for the anesthetic to wear off so they can walk or urinate.
Spinal anesthesia is often used for genital, urinary tract, or lower body procedures.
Epidural anesthesia is often used during labor and delivery, and surgery in the pelvis and legs.
Epidural and spinal anesthesia are often used when:
- The procedure or labor is too painful without any pain medicine.
- The procedure is in the belly, hips, legs, or feet.
- Your body can remain in a comfortable position during your procedure.
- You want fewer systemic medicines and less "hangover" than you would have from general anesthesia.
Risks
Spinal and epidural anesthesia are generally safe. Ask your provider about these possible complications:
- Allergic reaction to the anesthesia used
- Bleeding around the spinal column (hematoma)
- Difficulty urinating
- Drop in blood pressure
- Infection in your spine (meningitis or abscess)
- Nerve damage
- Seizures (this is rare)
- Severe headache
Before the Procedure
Tell your provider:
- If you are or could be pregnant
- What medicines you are taking, including medicines, illicit drugs, supplements, or herbs you bought without a prescription
During the days before the procedure:
- Tell your provider about any allergies or health conditions you have, what medicines you are taking, and what anesthesia or sedation you have had before.
- If your procedure is planned, you may be asked to stop taking aspirin, ibuprofen (Advil, Motrin), warfarin (Coumadin, Jantoven), and any other blood thinners.
- Ask your provider which medicines you should still take on the day of your procedure.
- Arrange for a responsible adult to drive you to and from the hospital or clinic.
- If you smoke, try to stop. Ask your provider for help quitting.
On the day of the procedure:
- Follow instructions on when to stop eating and drinking.
- Do not drink alcohol the night before and the day of your procedure.
- Take the medicines your provider told you to take with a small sip of water.
- Follow instructions on when to arrive at the hospital. Be sure to arrive on time.
After the Procedure
After either type of anesthesia:
- You will lie in bed until you have feeling in your legs and can walk.
- You may feel sick to your stomach and be dizzy. These side effects usually soon go away.
- You may be tired.
The nurse may ask you to try to urinate. This is to make sure your bladder muscles are working. Anesthesia relaxes the bladder muscles, making it hard to urinate. This can lead to urinary retention that is temporary or a bladder infection.
Outlook (Prognosis)
Most people feel no pain during spinal and epidural anesthesia and recover fully.
Alternative Names
Intrathecal anesthesia; Subarachnoid anesthesia; Epidural
Images
References
Hernandez A, Sherwood ER. Anesthesiology principles, pain management, and conscious sedation. In: Townsend CM Jr, Beauchamp RD, Evers BM, Mattox KL, eds. Sabiston Textbook of Surgery: The Biological Basis of Modern Surgical Practice. 21st ed. St Louis, MO: Elsevier; 2022:chap 14.
Macfarlane AJR, Hewson DW, Brull R. Spinal, epidural, and caudal anesthesia. In: Pardo MC, ed. Miller's Basics of Anesthesia. 8th ed. Philadelphia, PA: Elsevier; 2023:chap 17.
Review Date 4/30/2025
Updated by: Mark Gjolaj, MD, MBA, Anesthesiology and Pain Medicine Specialist, The Permanente Medical Group and Clinical Assistant Professor Adjunct, Stanford Health Care, Stanford, CA. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.