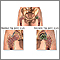
Osteonecrosis is bone death caused by poor blood supply. It is most common in the hip and shoulder but can affect other large joints such as the knee, elbow, wrist, and ankle.
Causes
Osteonecrosis occurs when part of the bone does not get blood flow and dies. After a while, the bone can collapse. If osteonecrosis is not treated, the nearby joint deteriorates, leading to severe arthritis.
Osteonecrosis can be caused by disease or by severe trauma, such as a fracture or dislocation, that affects the blood supply to the bone. Osteonecrosis can also occur without trauma or disease. This is called idiopathic -- meaning it occurs without any known cause.
The following are possible causes:
- Using oral or intravenous steroids
- Excessive alcohol use
- Sickle cell disease or any blood condition that causes abnormal blood clotting
- Dislocation or fractures around a joint
- Clotting disorders
- HIV or taking HIV drugs
- Radiation therapy or chemotherapy
- Gaucher disease (disease in which harmful substances build-up in certain organs and the bones)
- Systemic lupus erythematosus (an autoimmune disease in which the body's immune system mistakenly attacks healthy tissue such as the skin, joints, and certain organs)
- Legg-Calve-Perthes disease (childhood disease in which the thigh bone in the hip doesn't get enough blood, causing the bone to die)
- Decompression sickness from a lot of deep sea diving
When osteonecrosis occurs in the shoulder joint, it is usually due to long-term treatment with steroids, a history of trauma to the shoulder, or the person has sickle cell disease or any abnormal blood clotting conditions.
Symptoms
There are no symptoms in the early stages. As bone damage worsens, you may have the following symptoms:
- Pain in the joint that may increase over time and becomes severe if the bone collapses
- Pain that occurs even at rest
- Limited range of motion when the joint collapses
- Groin pain, if the hip joint is affected
- Limping, if the condition occurs in the leg
- Difficulty with overhead movement, if the shoulder joint is affected
- Worsening arthritic symptoms in the joint when the condition deteriorates
Exams and Tests
Your health care provider will do a physical exam to find out if you have any diseases or conditions that may affect your bones. You will be asked about your symptoms and medical history.
Be sure to let your provider know about any medicines or vitamin supplements you are taking, even over-the-counter medicine.
After the exam, your provider will order one or more of the following tests:
Treatment
If your provider knows the cause of your osteonecrosis, part of the treatment will be aimed at the underlying condition. For example, if a blood disorder is the cause, treatment will consist, in part, of medicine to treat it.
If the condition is caught early, you will take pain relievers and limit use of the affected area. This may include using crutches if your hip, knee, or ankle is affected. You may need to do range-of-motion exercises. Nonsurgical treatment can often slow the progression of osteonecrosis, but most people will eventually need surgery.
Surgical options include:
- A bone graft
- A bone graft along with its blood supply (vascularized bone graft)
- Removing part of the inside of the bone (core decompression) to relieve pressure and allow new blood vessels to form
- Cutting the bone and changing its alignment to relieve stress on the bone or joint (osteotomy)
- Replacing the deteriorated part with a donor osteochondral allograft
- Partial or total joint replacement
Support Groups
More information and support for people with osteonecrosis and their families can be found at:
- National Institute of Arthritis and Musculoskeletal and Skin Diseases -- www.niams.nih.gov/health-topics/osteonecrosis
- Arthritis Foundation -- www.arthritis.org
Outlook (Prognosis)
How well you do depends on the following:
- The cause of the osteonecrosis
- How severe the disease is when diagnosed
- The amount of bone involved
- Your age and overall health
Outcome may vary from complete healing to permanent damage in the affected bone.
Possible Complications
Advanced osteonecrosis can lead to osteoarthritis and permanent decreased mobility. Severe cases may require joint replacement.
When to Contact a Medical Professional
Contact your provider if you have symptoms.
Prevention
Many cases of osteonecrosis do not have a known cause, so prevention may not be possible. In some cases, you can reduce your risk by doing the following:
- Avoid drinking excessive amounts of alcohol.
- When possible, avoid high doses and long-term use of corticosteroids.
- Follow safety measures when diving to avoid decompression sickness.
Alternative Names
Avascular necrosis; Bone infarction; Ischemic bone necrosis; AVN; Aseptic necrosis
Images
References
McAlindon T, Carrino JA. Osteonecrosis. In: Hochberg MC, Gravallese EM, Smolen JS, van der Heijde D, Weinblatt ME, Weisman MH, eds. Rheumatology. 8th ed. Philadelphia, PA: Elsevier; 2023:chap 208.
Whyte MP, Dahir KM. Osteonecrosis, osteosclerosis/hyperostosis, and other disorders of the bone. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 229.
Review Date 6/4/2025
Updated by: C. Benjamin Ma, MD, Professor, Chief, Sports Medicine and Shoulder Service, UCSF Department of Orthopaedic Surgery, San Francisco, CA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.