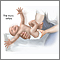
A reflex is a muscle reaction that happens automatically in response to stimulation. Certain sensations or movements produce specific muscle responses.
Considerations
The presence and strength of a reflex is an important sign of nervous system development and function.
Many infant reflexes disappear as the child grows older, although some remain through adulthood. A reflex that is still present after the age when it would normally disappear can be a sign of brain or nervous system damage.
Infant reflexes are responses that are normal in infants, but abnormal in other age groups. These include:
- Moro reflex
- Sucking reflex (sucks when area around mouth is touched)
- Startle reflex (pulling arms and legs in after hearing loud noise)
- Step reflex (stepping motions when sole of foot touches hard surface)
Other infant reflexes include:
TONIC NECK REFLEX
This reflex occurs when the head of a child who is relaxed and lying face up is moved to the side. The arm on the side where the head is facing reaches away from the body with the hand partly open. The arm on the side away from the face is flexed and the fist is clenched tightly. Turning the baby's face in the other direction reverses the position. The tonic neck position is often described as the fencer's position because it looks like a fencer's stance.
TRUNCAL INCURVATION OR GALANT REFLEX
This reflex occurs when the side of the infant's spine is stroked or tapped while the infant lies on the stomach. The infant will twitch their hips toward the touch in a dancing movement.
GRASP REFLEX
This reflex occurs if you place a finger on the infant's open palm. The hand will close around the finger. Trying to remove the finger causes the grip to tighten. Newborn infants have strong grasps and can almost be lifted up if both hands are grasping your fingers.
ROOTING REFLEX
This reflex occurs when the baby's cheek is stroked. The infant will turn toward the side that was stroked and begin to make sucking motions.
PARACHUTE REFLEX
This reflex occurs in slightly older infants when the child is held upright and the baby's body is rotated quickly to face forward (as in falling). The baby will extend their arms forward as if to break a fall, even though this reflex appears long before the baby walks.
Examples of reflexes that last into adulthood are:
- Blinking reflex: blinking the eyes when they are touched or when a sudden bright light appears
- Cough reflex: coughing when the airway is stimulated
- Gag reflex: gagging when the throat or back of the mouth is stimulated
- Sneeze reflex: sneezing when the nasal passages are irritated
- Yawn reflex: yawning when the body needs more oxygen
Causes
Infant reflexes can occur in adults who have:
- Brain damage
- Stroke
When to Contact a Medical Professional
Your health care provider will often discover abnormal infant reflexes during an exam that is done for another reason. Reflexes that remain longer than they should may be a sign of a nervous system problem.
Parents should talk to their child's provider if:
- They have worries about their child's development.
- They notice that baby reflexes continue in their child after they should have stopped.
What to Expect at Your Office Visit
Your provider will perform a physical exam and ask about the child's medical history.
Questions may include:
- What reflexes did the baby have?
- At what age did each infant reflex disappear?
- What other symptoms are present (for example, decreased alertness or seizures)?
Alternative Names
Primitive reflexes; Reflexes in infants; Tonic neck reflex; Galant reflex; Truncal incurvation; Rooting reflex; Parachute reflex; Grasp reflex
Images
References
Chaves-Gnecco D, Feldman HM. Developmental/behavioral pediatrics. In: Zitelli BJ, McIntire SC, Nowalk AJ, Garrison J, eds. Zitelli and Davis' Atlas of Pediatric Physical Diagnosis. 8th ed. Philadelphia, PA: Elsevier; 2023:chap 3.
Edelman HE, Stratton MJ. Neurology. In: Anderson CC, Kapoor S, Mark TE, eds. Harriet Lane Handbook, The. 23rd ed. Philadelphia, PA: Elsevier; 2024:chap 20.
Holler-Managan YF. Neurological evaluation. In: Kliegman RM, St. Geme JW, Blum NJ, et al, eds. Nelson Textbook of Pediatrics. 22nd ed. Philadelphia, PA: Elsevier; 2025:chap 630.
Review Date 10/7/2025
Updated by: Neil K. Kaneshiro, MD, MHA, Clinical Professor of Pediatrics, University of Washington School of Medicine, Seattle, WA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.