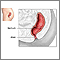
Rectal prolapse repair is surgery to fix a rectal prolapse. This is a condition in which the last part of the intestine (called the rectum) sticks out through the anus.
Description
Rectal prolapse may be partial, involving only the inner lining of the bowel (mucosa). Or, it may be complete, involving the entire wall of the rectum.
For most adults, surgery is used to repair the rectum because there is no other effective treatment.
Children with rectal prolapse do not always need surgery, unless their prolapse does not improve over time. In infants, prolapse often disappears without treatment.
Most surgical procedures for rectal prolapse are done under general anesthesia. For older or sicker people, epidural or spinal anesthesia may be used.
There are three basic types of surgery to repair rectal prolapse. Your surgeon will decide which one is best for you.
For healthy adults, an abdominal procedure has the best chance of success. While you are under general anesthesia, your surgeon makes a cut in the abdomen and removes a portion of the colon. The rectum may be attached (sutured) to the surrounding tissue so it will not slide and fall out through the anus. Sometimes, a soft piece of mesh is wrapped around the rectum to help it stay in place. These procedures can also be done with laparoscopic surgery.
For older adults or those with other medical problems, an approach through the anus (perineal approach) might be less risky. It might also cause less pain and lead to a shorter recovery. But with this approach, the prolapse is more likely to come back (recur).
One of the surgical repairs through the anus involves removing the prolapsed rectum and colon and then suturing the rectum to the surrounding tissues. This procedure can be done under general, epidural, or spinal anesthesia.
Very frail or sick people may need a smaller procedure that reinforces the sphincter muscles. This technique encircles the muscles with a band of soft mesh or a silicone tube. This approach provides only short-term improvement and is rarely used.
Risks
Risks of anesthesia and surgery in general include:
- Reactions to medicines
- Breathing problems
- Bleeding, blood clots, infection
Risks of this surgery include:
- Infection. If a piece of rectum or colon is removed, the bowel needs to be reconnected. In rare cases, this connection can leak, causing infection. More procedures may be needed to treat the infection.
- Constipation is very common, although most people have constipation before the surgery.
- In some people, incontinence (loss of bowel control) can get worse.
- Return of prolapse after abdominal or perineal surgery.
Before the Procedure
Tell your surgeon or nurse if:
- You are or could be pregnant
- You are taking any medicines, including medicines, drugs, supplements, or herbs you bought without a prescription
- You have been drinking a lot of alcohol, more than 1 or 2 drinks a day
Planning for your surgery:
- If you have diabetes, heart disease, or other medical conditions, your surgeon may ask you to see the provider who treats you for these conditions.
- If you smoke, it's important to cut back or quit. Smoking can slow healing and increase the risk for blood clots. Ask your provider for help quitting smoking.
- If needed, prepare your home to make it easier to recover after surgery.
- Ask your surgeon if you need to arrange to have someone drive you home after your surgery.
During the week before your surgery:
- You may be asked to stop taking medicines that make it harder for your blood to clot. These medicines are called blood thinners. This includes over-the-counter medicine and supplements such as aspirin, ibuprofen (Advil, Motrin), naproxen (Aleve, Naprosyn), and vitamin E. Many prescription medicines are also blood thinners.
- Ask your surgeon which medicines you should still take on the day of your surgery.
- Let your surgeon know about any illness you may have before your surgery. This includes COVID-19, a cold, flu, fever, herpes outbreak, or other illness. If you do get sick, your surgery may need to be postponed.
On the day of your surgery:
- Follow instructions about when to stop eating and drinking.
- Take any medicines your surgeon told you to take with a small sip of water.
- Be sure to arrive at the hospital on time.
After the Procedure
How long you stay in the hospital depends on the procedure. For open abdominal procedures it may be 5 to 8 days. You will go home sooner if you had laparoscopic surgery. The stay for perineal surgery may be 2 to 3 days.
You should make a complete recovery in 4 to 6 weeks.
Outlook (Prognosis)
The surgery usually works well at repairing the prolapse. Constipation and incontinence can be problems for some people.
Alternative Names
Rectal prolapse surgery; Anal prolapse surgery
References
Horesh N, Emile S, Wexner SD. Colon and rectum. In: Tyler DS, Hayes-Dixon A, Hines OJ, et al, eds. Sabiston Textbook of Surgery. 22nd ed. Philadelphia, PA: Elsevier; 2026:chap 95.
Leannec IL, O'Connell E, Safar B. Management of rectal prolapse. In: Cameron JL, Cameron AM, eds. Current Surgical Therapy. 15th ed. Philadelphia, PA: Elsevier; 2026:chap 39.
Review Date 1/1/2026
Updated by: Ann M. Rogers, MD, FACS, Professor Emeritus, Department of Surgery, Penn State College of Medicine, Hershey, PA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.