Absence of a woman's monthly menstrual period is called amenorrhea.
Primary amenorrhea is when a girl has not yet started her monthly periods, and she:
- Has gone through other normal changes that occur during puberty
- Is older than 15
Causes
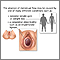
Most girls begin their periods between ages 9 and 18. The average is around 12 years old. If no periods have occurred when a girl is older than 15, further testing may be needed. The need is more urgent if she has gone through other normal changes that occur during puberty.
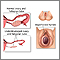
Being born with incompletely formed genital or pelvic organs can lead to a lack of menstrual periods. Some of these defects include:
- Blockages or narrowing of the cervix
- Hymen that has no opening
- Missing uterus or vagina
- Vaginal septum (a wall that divides the vagina into 2 sections)
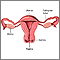
Hormones play a big role in a woman's menstrual cycle. Hormone problems can occur when:
- Changes occur to the parts of the brain where hormones that help manage the menstrual cycle are produced.
- The ovaries are not working correctly.
Either of these problems may be due to:
- Anorexia (loss of appetite) with low body mass index (BMI)
- Chronic or long-term illnesses, such as cystic fibrosis or heart disease
- Genetic defects or disorders
- Infections that occurred before or after the woman's birth
- Other birth defects
- Poor nutrition
- Tumors
In many cases, the cause of primary amenorrhea is not known.
Symptoms
A female with amenorrhea will have no menstrual flow. She may have other signs of puberty.
Exams and Tests
The health care provider will perform a physical exam to check for birth defects of the vagina or uterus.
The provider will ask questions about:
- Your medical history
- Medicines and supplements you may be taking
- How much exercise you do
- Your eating habits
A pregnancy test will be done.
Blood tests to measure different hormone levels may include:
- Estradiol
- Follicle stimulating hormone (FSH)
- Luteinizing hormone (LH)
- Prolactin
- 17 hydroxyprogesterone
- Serum progesterone
- Serum testosterone level
- Thyroid stimulating hormone (TSH)
- T3 and T4
Other tests that may be done include:
- Chromosome or genetic testing
- Head CT scan or head MRI scan to look for brain tumors
- Pelvic ultrasound or MRI to look for birth defects
Treatment
Treatment depends on the cause of the missing period. Lack of periods that is caused by birth defects may require hormone medicines, surgery, or both.
If the amenorrhea is caused by a tumor in the brain:
- Medicines may shrink certain types of tumors.
- Surgery to remove the tumor may also be needed.
- Radiation therapy is usually only done when other treatments have not worked.
If the problem is caused by a systemic disease, treatment of the disease may allow menstruation to begin.
If the cause is bulimia, anorexia or too much exercise, periods will often begin when the weight returns to normal or the exercise level is decreased.
If the amenorrhea cannot be corrected, hormone medicines can sometimes be used. Medicines can help the woman feel more like her friends and female family members. They can also protect the bones from becoming too thin (osteoporosis).
Outlook (Prognosis)
The outlook depends on the cause of the amenorrhea and whether it can be corrected with treatment or lifestyle changes.
Periods are not likely to start on their own if the amenorrhea was caused by one of the following conditions:
- Birth defects of the female organs
- Craniopharyngioma (a tumor near the pituitary gland at the base of the brain)
- Cystic fibrosis
- Genetic disorders
You may have emotional distress because you feel different from friends or family. Or, you may worry that you might not be able to have children.
When to Contact a Medical Professional
Contact your provider if your daughter is older than 15 and has not yet begun menstruating, or if she is 14 or older and shows no other signs of puberty.
Alternative Names
Primary amenorrhea; No periods - primary; Absent periods - primary; Absent menses - primary; Absence of periods - primary
References
Bulun SE. Physiology and pathology of the female reproductive axis. In: Melmed S, Auchus RJ, Goldfine AB, Koenig RJ, Rosen CJ, eds. Williams Textbook of Endocrinology. 14th ed. Philadelphia, PA: Elsevier; 2020:chap 17.
Cameron S. Menstruation and amenorrhoea. In: Magowan B, ed. Clinical Obstetrics and Gynaecology. 5th ed. Elsevier; 2023:chap 4.
Lobo RA. Primary and secondary amenorrhea and precocious puberty: etiology, diagnostic evaluation, management. In: Gershenson DM, Lentz GM, Valea FA, Lobo RA, eds. Comprehensive Gynecology. 8th ed. Philadelphia, PA: Elsevier; 2022:chap 36.
Review Date 4/16/2024
Updated by: John D. Jacobson, MD, Professor Emeritus, Department of Obstetrics and Gynecology, Loma Linda University School of Medicine, Loma Linda, CA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.