Adrenoleukodystrophy (ALD) describes several closely related disorders that disrupt the breakdown of certain fats. These disorders are often passed down (inherited) in families.
Causes
ALD is usually passed down from parent to child as an X-linked genetic trait. It affects mostly males. Some women who are carriers can have milder forms of the disease. It affects about 1 in 20,000 to 1 in 50,000 people from all races.
Some cases of ALD occur when the gene changes on its own. This is called sporadic and is not inherited.
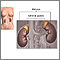
The condition results in the buildup of very-long-chain fatty acids in the nervous system, adrenal gland, and testes. This disrupts normal activity in these parts of the body.
There are three major categories of disease:
- Childhood cerebral form -- appears in mid-childhood (at ages 4 to 12)
- Adrenomyelopathy -- occurs in men between their 20s and 40s
- Impaired adrenal gland function (called Addison disease or Addison-like phenotype) -- adrenal gland does not produce enough steroid hormones
Symptoms
Childhood cerebral type symptoms include:
- Changes in muscle tone, especially muscle spasms and uncontrolled movements
- Crossed eyes
- Handwriting that gets worse
- Difficulty at school
- Difficulty understanding what people are saying
- Hearing loss
- Hyperactivity
- Worsening nervous system damage, including coma, decreased fine motor control, and paralysis
- Swallowing difficulties
- Visual impairment or blindness
Adrenomyelopathy symptoms include:
- Difficulty controlling urination
- Possible worsening muscle weakness or leg stiffness
- Problems with thinking speed and visual memory
Adrenal gland failure (Addison type) symptoms include:
- Coma
- Decreased appetite
- Increased skin color
- Loss of weight and muscle mass (wasting)
- Muscle weakness
- Vomiting
Exams and Tests
In most states, children will be screened for ALD as part of newborn screening tests. This is done with a heel stick to draw blood (as part of the routine screenings done on newborns). Newborn screening does not diagnose the condition, but it can help lead to early testing and diagnosis.
Tests for this condition include:
- Blood levels of very long chain fatty acids and hormones that are produced by the adrenal gland
- Chromosome study to look for changes in the ABCD1 gene that may make the person more likely to develop a disease
- MRI of the head
- Skin biopsy
Treatment
Adrenal dysfunction may be treated with steroids (such as cortisol) if the adrenal gland is not producing enough hormones.
A specific treatment for X-linked ALD is not available. A bone marrow transplant may stop worsening of the condition.
Supportive care and careful monitoring of impaired adrenal gland function may help in improving comfort and quality of life.
Support Groups
More information and support for people with ALD and their families can be found at:
- National Organization for Rare Disorders -- rarediseases.org/rare-diseases/adrenoleukodystrophy/
- NIH Genetic and Rare Diseases Information Center -- rarediseases.info.nih.gov/diseases/5758/x-linked-adrenoleukodystrophy
Outlook (Prognosis)
The childhood form of X-linked ALD is a progressive disease. It leads to a long-term coma (minimally conscious state) about 2 years after nervous system symptoms develop. The child can live in this condition for as long as 10 years until death occurs.
The other forms of this disease are milder.
Possible Complications
These complications can occur:
- Adrenal crisis
- Long-term coma
When to Contact a Medical Professional
Contact your health care provider if:
- Your child develops symptoms of X-linked ALD
- Your child has X-linked ALD and is getting worse
Prevention
Genetic counseling is recommended for couples with a family history of X-linked ALD. Mothers of affected sons have an 85% chance of being a carrier for this condition.
Prenatal diagnosis of X-linked ALD is also available. It is done by testing cells from chorionic villus sampling or amniocentesis. These tests look for either a known genetic change in the family or for very long chain fatty acid levels.
Alternative Names
X-linked Adrenoleukodystrophy; Adrenomyeloneuropathy; Childhood cerebral adrenoleukodystrophy; ALD; Schilder-Addison Complex
References
James WD. Errors in metabolism. In: James WD, ed. Andrews' Diseases of the Skin: Clinical Dermatology. 14th ed. Philadelphia, PA: Elsevier; 2026:chap 21.
Kliegman RM, St. Geme JW, Blum NJ, et al. Defects in metabolism of lipids. In: Kliegman RM, St. Geme JW, Blum NJ, et al, eds. Nelson Textbook of Pediatrics. 22nd ed. Philadelphia, PA: Elsevier; 2025:chap 106.
Lissauer T, Carroll W. Neurological disorders. In: Lissauer T, Carroll W, eds. Illustrated Textbook of Paediatrics. 6th ed. Philadelphia, PA: Elsevier; 2022:chap 29.
Review Date 10/27/2025
Updated by: Anna C. Edens Hurst, MD, MS, Associate Professor in Medical Genetics, The University of Alabama at Birmingham, Birmingham, AL. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.