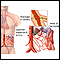
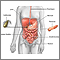
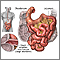
Intestinal ischemia and infarction occurs when there is a narrowing or blockage of one or more of the arteries that supply the small intestine.
Causes
There are several possible causes of intestinal ischemia and infarction.
- Hernia -- If the intestine moves into the wrong place or becomes tangled, it can cut off the blood flow.
- Adhesions -- The intestine may become trapped in scar tissue (adhesions) from past surgery. This can lead to loss of blood flow if left untreated.
- Embolus -- Blood clots can block one of the arteries supplying the intestine. People who have had a heart attack or who have arrhythmias, such as atrial fibrillation, are at risk for this problem.
- Narrowing of the arteries -- The arteries that supply blood to the bowel may become narrowed or blocked from cholesterol buildup. When this happens in the arteries to the heart, it causes a heart attack. When it happens in the arteries to the intestine, it causes intestinal ischemia.
- Narrowing of the veins -- The veins carrying blood away from the intestine may become blocked by blood clots. This blocks blood flow in the intestine. This is more common in people with liver disease, cancer, or blood clotting disorders.
- Low blood pressure -- Very low blood pressure in people who already have narrowing of the intestinal arteries may also cause loss of blood flow to the intestine. This often occurs in people with other serious medical problems.
Symptoms
The main symptom of intestinal ischemia is pain in abdomen. The pain is severe, even though the area is not very tender when touched. Other symptoms include:
- Diarrhea
- Fever
- Vomiting
- Blood in the stool
Exams and Tests
Laboratory tests may show a high white blood cell (WBC) count (a marker of infection). There may be bleeding in the GI tract.
Some tests to detect the extent of damage include:
- Increased acid in the bloodstream (lactic acidosis)
- Angiogram
- CT scan of the abdomen
- Doppler ultrasound of the abdomen
These tests do not always detect the problem. Sometimes, the only way to detect intestinal ischemia is with a surgical procedure.
Outlook (Prognosis)
Damage or death of the bowel tissue is a serious condition. This can result in death if not treated right away. The outlook depends on the cause. Prompt treatment can lead to a good outcome.
Possible Complications
Damage or death of the bowel tissue may require a colostomy or ileostomy. This may be short-term or permanent. Peritonitis is common in these cases. People who have a large amount of tissue death in the intestine can have problems absorbing nutrients. They can become dependent on getting nutrition through their veins.
Some people may become severely ill with fever and a bloodstream infection (sepsis).
When to Contact a Medical Professional
Contact your health care provider if you have any severe abdominal pain.
Prevention
Preventive measures include:
- Controlling risk factors, such as irregular heartbeat, high blood pressure, and high cholesterol
- Not smoking
- Eating a nutritious diet
- Quickly treating hernias
Alternative Names
Intestinal necrosis; Ischemic bowel - small intestine; Dead bowel - small intestine; Dead gut - small intestine; Infarcted bowel - small intestine; Atherosclerosis - small intestine; Hardening of the arteries - small intestine
References
Feuerstadt P, Brandt LJ. Intestinal ischemia. In: Feldman M, Friedman LS, Brandt LJ, eds. Sleisenger and Fordtran's Gastrointestinal and Liver Disease. 11th ed. Philadelphia, PA: Elsevier; 2021:chap 118.
Holscher CM, Reifsnyder T. Acute mesenteric ischemia. In: Cameron JL, Cameron AM, eds. Current Surgical Therapy. 13th ed. Philadelphia, PA: Elsevier; 2020:1057-1061.
Kahi CJ. Vascular diseases of the gastrointestinal tract. In: Goldman L, Schafer AI, eds. Goldman-Cecil Medicine. 26th ed. Philadelphia, PA: Elsevier; 2020:chap 134.
Roline CE, Reardon RF. Disorders of the small intestine. In: Walls RM, Hockberger RS, Gausche-Hill M, eds. Rosen's Emergency Medicine: Concepts and Clinical Practice. 9th ed. Philadelphia, PA: Elsevier; 2018:chap 82.
Review Date 2/7/2022
Updated by: Michael M. Phillips, MD, Emeritus Professor of Medicine, The George Washington University School of Medicine, Washington, DC. Also reviewed by David Zieve, MD, MHA, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.